🧠 Pathophysiology - Weak Walls, Big Trouble
- Origin: Congenital weakness at arterial bifurcations, primarily in the Circle of Willis.
- Defect: Focal absence of internal elastic lamina and thinned tunica media.
- Growth & Rupture: Governed by the Law of Laplace, $T = (P \times r) / 2h$.
- As radius ($r$) ↑, wall tension ($T$) ↑, increasing rupture risk.
- Key Risk Factors:
- Chronic Hypertension (HTN)
- Smoking
- Autosomal Dominant Polycystic Kidney Disease (ADPKD)
- Connective tissue disorders (Marfan, Ehlers-Danlos)
⭐ 85-95% of cerebral aneurysms are saccular ("berry") type, most commonly at the Anterior Communicating Artery (ACom) junction.
🤯 Clinical Manifestations - The Worst Headache
- Classic Presentation: Sudden, explosive "thunderclap" headache, reaching maximum intensity within seconds.
- Patient often describes it as the "worst headache of my life."
- Key Associated Symptoms:
- Nausea/Vomiting
- Meningismus (nuchal rigidity, photophobia) due to blood in CSF.
- Loss of consciousness (LOC).
- Focal deficits (e.g., CN III palsy from PComm aneurysm).
- ⚠️ Sentinel Headache: A less severe, warning headache may precede rupture by days/weeks in ~30-50% of patients.
⭐ The hallmark of a ruptured aneurysm is a "thunderclap headache" from subarachnoid hemorrhage (SAH).
🧠 Diagnosis - Finding the Bubble
-
Initial Test (Suspected Rupture/SAH):
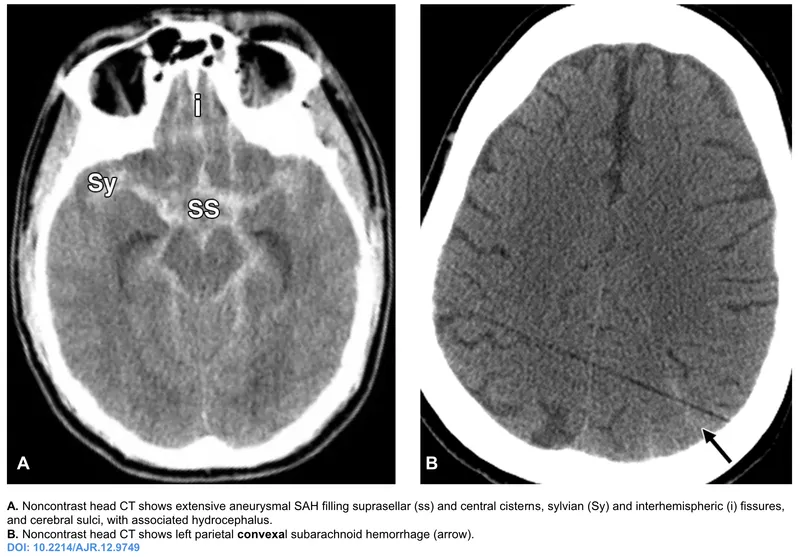
- 1st: Non-contrast head CT to detect subarachnoid blood.
- 2nd (if CT negative, high suspicion): Lumbar Puncture (LP).
-
Localization Imaging (Post-SAH confirmation):
- CT Angiography (CTA): Rapid, first-line for locating the aneurysm.
- Digital Subtraction Angiography (DSA): Gold standard; invasive, for definitive diagnosis/planning.
⭐ Xanthochromia (yellow CSF from bilirubin) on LP is diagnostic for SAH if the initial CT is negative. It appears 6-12 hours after the bleed.
🧠 Management - To Clip or Coil?
The primary goal is to exclude the aneurysm from circulation to prevent (re)rupture. The choice between open surgery and endovascular methods depends on aneurysm and patient factors.
| Feature | Surgical Clipping | Endovascular Coiling |
|---|---|---|
| Approach | Open craniotomy | Catheter-based (femoral a.) |
| Best For | Wide-neck, MCA aneurysms | Narrow-neck, posterior circ. |
| Durability | More durable, ↓ re-bleed | ↑ Retreatment rate |
| Risk | ↑ Peri-procedural risk | ↓ Peri-procedural risk |
| Ideal Pt | Young, good surgical candidate | Elderly, poor surgical candidate |
💥 Complications - Post-Pop Problems
- Rebleeding: Highest risk in first 24 hrs. Often fatal. Secure aneurysm early.
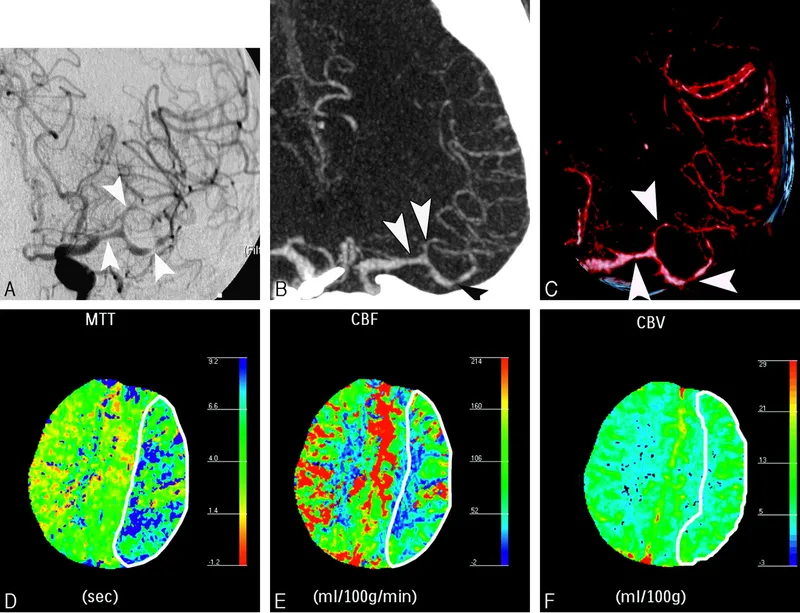
- Cerebral Vasospasm: Onset 3-14 days post-SAH, causing delayed cerebral ischemia (DCI).
- Prophylaxis: Nimodipine (oral CCB) for all SAH patients.
- Dx: Transcranial Doppler (TCD), CTA.
- Hydrocephalus: Blood obstructs arachnoid granulations → communicating hydrocephalus.
- Hyponatremia: SIADH vs. Cerebral Salt Wasting (CSW).
- Seizures: Risk is highest initially.
⭐ Vasospasm is the main cause of delayed morbidity/mortality. Its delayed onset (3-14 days) is a classic exam point.
⚡ Biggest Takeaways
- Ruptured aneurysm presents as a "worst headache of life" (thunderclap headache) from subarachnoid hemorrhage (SAH).
- Initial diagnosis is a non-contrast CT scan. If negative, a lumbar puncture showing xanthochromia is diagnostic.
- Cerebral angiography (CTA/MRA/DSA) is required to locate the aneurysm, most commonly at the ACom artery.
- Nimodipine is essential to prevent vasospasm, a major cause of delayed ischemia (days 3-10 post-SAH).
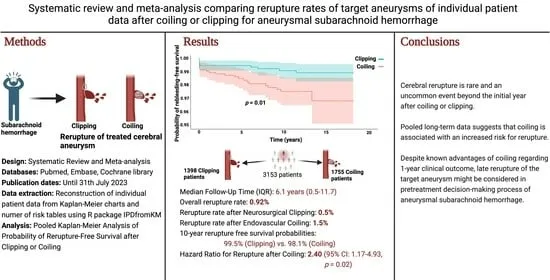
- Prevent rebleeding (highest risk <24h) with endovascular coiling or surgical clipping.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

