🧠 Tangled Vessels 101
An Arteriovenous Malformation (AVM) is a congenital tangle of vessels where arteries connect directly to veins, bypassing the capillary bed. This creates a high-flow, high-pressure central nidus, prone to rupture and cause intracranial hemorrhage (ICH).
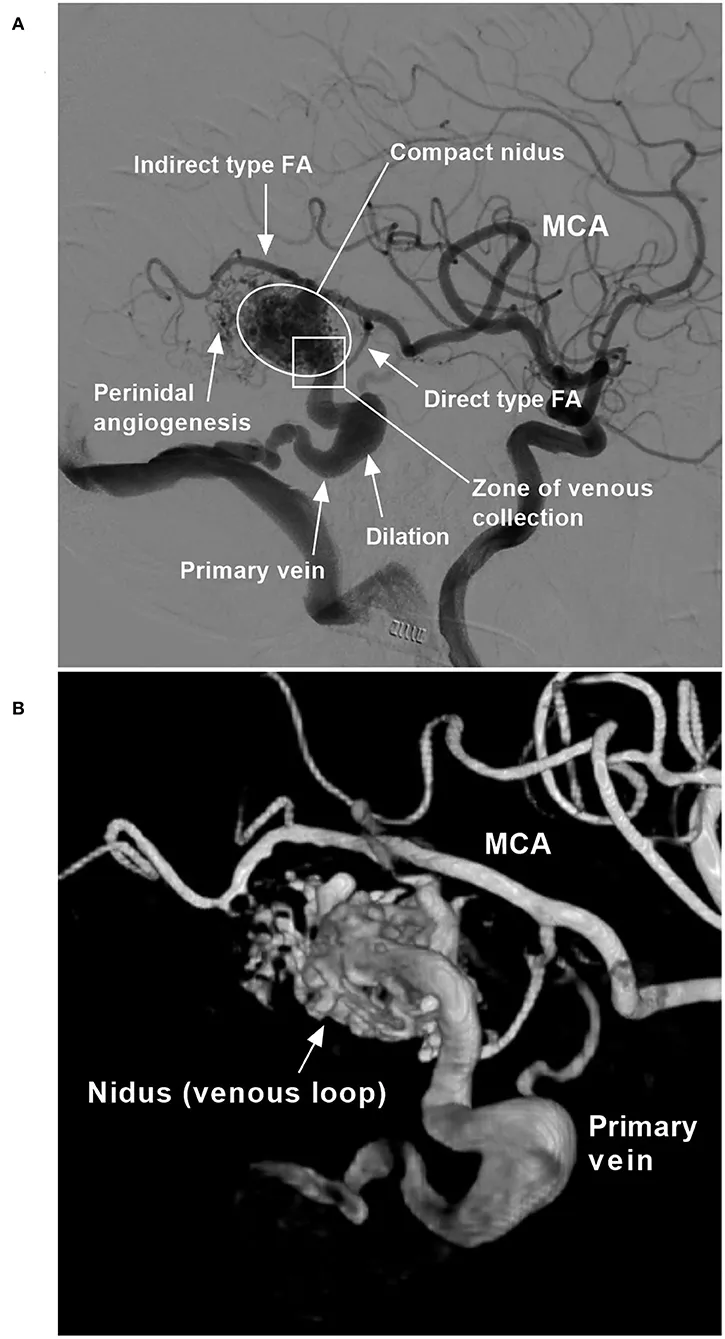
Spetzler-Martin Grading Scale (predicts surgical risk):
- Size of Nidus:
- <3 cm: 1 pt
- 3-6 cm: 2 pts
-
6 cm: 3 pts
- Eloquence of Brain Area:
- Non-eloquent: 0 pts
- Eloquent: 1 pt
- Venous Drainage Pattern:
- Superficial only: 0 pts
- Deep: 1 pt
⭐ The annual hemorrhage risk for an unruptured AVM is 2-4%. Risk is higher if previously ruptured or associated with an aneurysm.
💣 Diagnosis - Finding the Ticking Bomb
-
Clinical Presentation:
- Intracranial Hemorrhage (ICH): Most common (~50%), often a sudden, severe "worst headache of life."
- Seizures: New-onset, particularly in a young adult.
- Focal Neurological Deficits (FNDs): Weakness, sensory loss, aphasia.
- Headaches: Chronic, often pulsatile or migraine-like.
-
Imaging Pathway:
- Acute: Non-contrast CT to rapidly detect hemorrhage.
- Non-invasive: CT Angiography (CTA) or MR Angiography (MRA) to visualize the vascular tangle.
- Gold Standard: Digital Subtraction Angiography (DSA) provides definitive diagnosis and is essential for treatment planning.
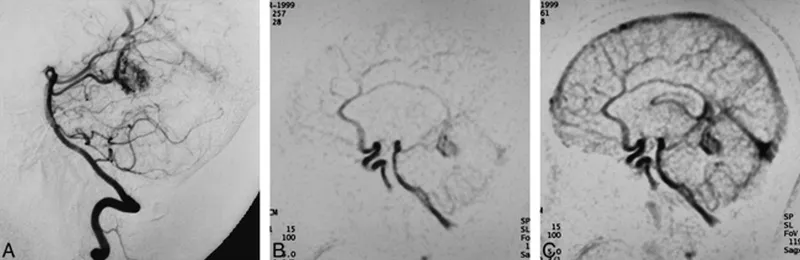
⭐ AVM is the most common cause of spontaneous intracerebral hemorrhage in children and young adults.
🧠 Management - Untangling the Knot
- Goal: Obliterate the nidus to prevent hemorrhage while preserving function. Decision balances treatment risk vs. natural history, guided by the Spetzler-Martin (SM) Grade (Size, Venous Drainage, Eloquence). Multimodality therapy is common.
| Modality | Mechanism | Best For | Pros | Cons |
|---|---|---|---|---|
| Microsurgery | Direct excision of nidus | Small, superficial, non-eloquent AVMs (SM Grade I-II) | Immediate & high rate of cure | Invasive; risk of intra-op bleed, neuro deficit |
| Embolization | Endovascular glue/coils to block feeding arteries | Adjunct to surgery/SRS; palliative for high-grade AVMs | Minimally invasive; reduces nidus size/flow | Rarely curative alone; risk of stroke, vessel perforation |
| SRS | Focused radiation induces thrombosis | Small (<3 cm), deep, eloquent AVMs | Non-invasive | Delayed effect (1-3 yrs); hemorrhage risk during latency; radiation necrosis |
Treatment Algorithm:
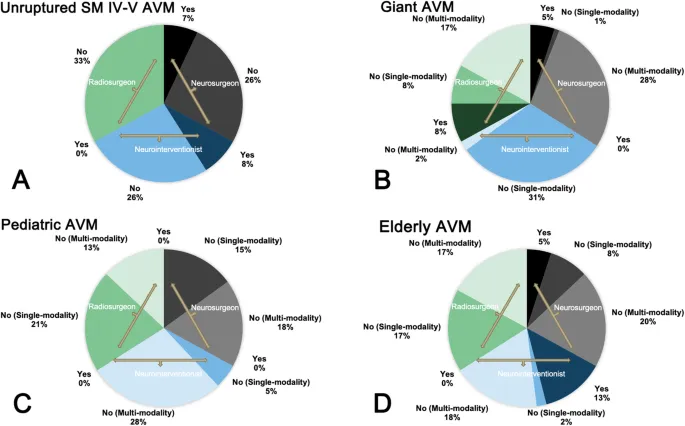
⚠️ Complications - When Things Go Wrong
- Untreated AVMs:
- Re-hemorrhage (highest risk in 1st year)
- Seizures, hydrocephalus, vasospasm
- Treatment-Related:
- Microsurgery: Infection, new neurological deficits
- Embolization: Embolic stroke, vessel perforation
- SRS: Radiation necrosis (delayed), hemorrhage before obliteration
⭐ Normal Perfusion Pressure Breakthrough (NPPB): Post-resection, chronically hypo-perfused brain tissue is suddenly exposed to normal arterial pressure. Loss of autoregulation leads to vasogenic edema, hemorrhage, and seizures.
⚡ Biggest Takeaways
- The primary goal of AVM treatment is preventing hemorrhage, the most feared complication, especially in young adults.
- Microsurgical resection is the gold standard for accessible AVMs, providing an immediate and definitive cure.
- Stereotactic radiosurgery (SRS) is ideal for small (<3 cm), deep, or eloquent-area AVMs; obliteration takes 1-3 years.
- Endovascular embolization is typically an adjunctive therapy to reduce AVM size and blood flow before surgery or SRS.
- Treatment choice is guided by the Spetzler-Martin grade.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

