🤖 Core concept - Meet the Gyn-Bot
Robotic surgery is an advanced form of minimally invasive surgery (MIS), essentially a high-tech evolution of laparoscopy. It's a master-slave system, not an autonomous robot.
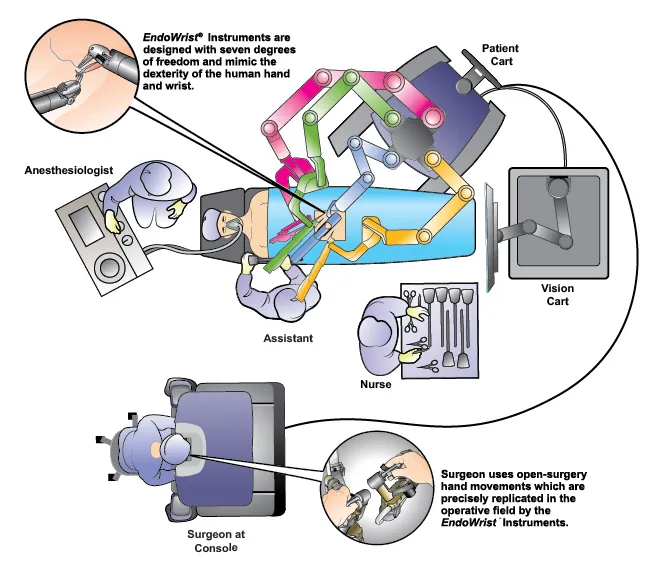
-
Key Advantages vs. Laparoscopy:
- Vision: 3D high-definition view.
- Precision: Wristed instruments with 7 degrees of freedom, tremor filtration, and motion scaling.
- Ergonomics: Seated console position reduces surgeon fatigue.
-
Key Disadvantages:
- ↑ Cost and operative time (setup/docking).
- Loss of haptic (tactile) feedback.
- Requires specialized training.
⭐ The main advantage over laparoscopy is wristed instrumentation, facilitating complex dissection and suturing in procedures like myomectomy and sacrocolpopexy.
🤖 Clinical Manifestations - When Robots Assist
-
Surgical Advantages (vs. Laparoscopy):
- Enhanced 3D high-definition vision.
- 7 degrees of freedom with EndoWrist instruments mimics human wrist (↑ dexterity).
- Tremor filtration for improved precision.
- Improved surgeon ergonomics (seated at console, reducing fatigue).
-
Key Limitations:
- ⚠️ Loss of haptic (tactile) feedback.
- ↑ Operative time, especially during initial setup/docking.
- Significantly ↑ cost.
⭐ The primary trade-off is the loss of haptic feedback, forcing surgeons to rely heavily on visual cues for tissue tension, a common exam topic.
🤖 Management - The Robotic Workflow
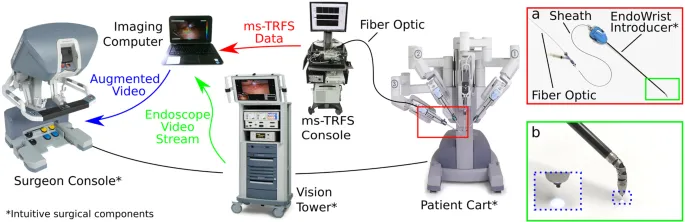
- Patient Positioning: Dorsal lithotomy with steep Trendelenburg is standard for pelvic access. Arms are tucked to prevent injury and allow robot access.
- Pneumoperitoneum: CO₂ insufflation (target pressure 12-15 mmHg) creates the operative space. Established via Veress needle or open Hasson technique.
- Docking: The patient cart is carefully positioned over the patient. Robotic arms are then attached ("docked") to the surgical trocars.
- Console Operation: The surgeon operates from a remote console, benefiting from 3D vision and wristed instruments. A skilled bedside assistant is critical.
⭐ Steep Trendelenburg position is crucial for pelvic exposure but ↑ risk of intraocular pressure, cerebral edema, and brachial plexus injury.
🤖 Complications - Robotic Mishaps & Fixes
- System Failure:
- Power Loss/System Crash: Undock instruments immediately. Convert to laparoscopy or laparotomy.
- Instrument/Vision Failure: Troubleshoot (e.g., clean camera) or replace the faulty component.
- Operator & Positioning Issues:
- Loss of Haptics: ↑ risk of tissue trauma. Rely on visual cues (tissue deformation).
- Thermal Injury: ⚠️ Capacitive coupling can cause occult bowel injury (delayed presentation). Use minimal power.
- Nerve Palsy: Brachial plexus, common peroneal. Due to prolonged steep Trendelenburg.
- Port-Site Hernia: ↑ risk with >10 mm ports. Requires fascial closure.
⭐ Steep Trendelenburg positioning (>30°) for pelvic access is a major risk factor for brachial plexus neuropathy and postoperative ocular complications like corneal abrasion or ischemic optic neuropathy.
⚡ Biggest Takeaways
- Robotic surgery enhances laparoscopy with 3D visualization and wristed instruments, improving dexterity and precision.
- Benefits mirror laparoscopy: ↓ blood loss, ↓ pain, and shorter hospital stays compared to open procedures.
- Major drawbacks include high cost, longer operative times (especially on the learning curve), and a crucial lack of haptic feedback.
- Ideal for complex procedures like hysterectomy, myomectomy, sacrocolpopexy, and certain gynecologic cancer staging.
- Specific risks include vaginal cuff dehiscence and nerve injuries (e.g., brachial plexus) from prolonged steep Trendelenburg positioning.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

