🗺️ Anatomy - Know Your Globes
- Location: Ovaries reside in the ovarian fossa on the lateral pelvic wall.
- Key Ligaments:
- Suspensory (IP) Ligament: Connects ovary to pelvic wall. Contains the ovarian artery, vein, nerves, and lymphatics.
- Ovarian Ligament: Connects ovary to the uterus.
- Blood Supply:
- Artery: Ovarian artery (from abdominal aorta).
- Vein: Right ovarian vein → IVC; Left ovarian vein → Left renal vein.
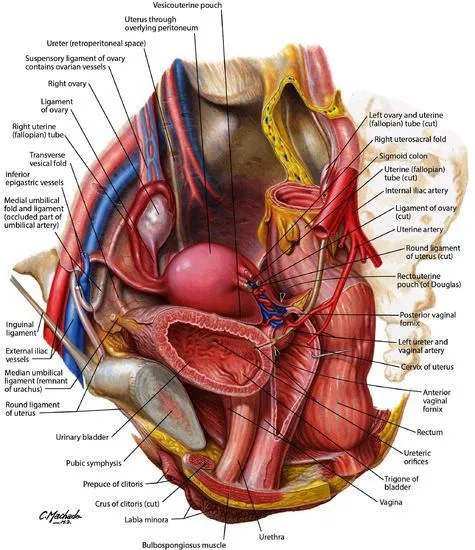
⭐ "Water under the bridge": The ureter passes under the ovarian vessels at the pelvic brim. It is at high risk of injury during oophorectomy when clamping the IP ligament.
🧐 Clinical manifestations - Cystic Conundrums
- Asymptomatic: Most common; often an incidental finding on imaging.
- Symptomatic (Non-acute):
- Dull, aching pelvic pain or pressure.
- Bloating, early satiety, dyspareunia.
- Menstrual irregularities (e.g., from hormone-producing cysts).
- Acute Complications (Surgical Emergencies):
- Torsion: Sudden, severe unilateral pain, nausea/vomiting.
- Rupture: Abrupt pain onset, potential peritoneal signs.
- Hemorrhage: Into cyst or peritoneum, may cause hypovolemia.
⭐ Ovarian torsion is a "don't miss" diagnosis. Risk ↑ with cysts >5 cm. Doppler US may show decreased or absent blood flow (whirlpool sign).
🧐 Diagnosis - Peeking at Pelvis
- Initial Imaging: Transvaginal Ultrasound (TVUS) is the primary modality to characterize adnexal masses.
- Benign Features: Simple, unilocular, thin-walled, anechoic, no solid components, typically <10 cm.
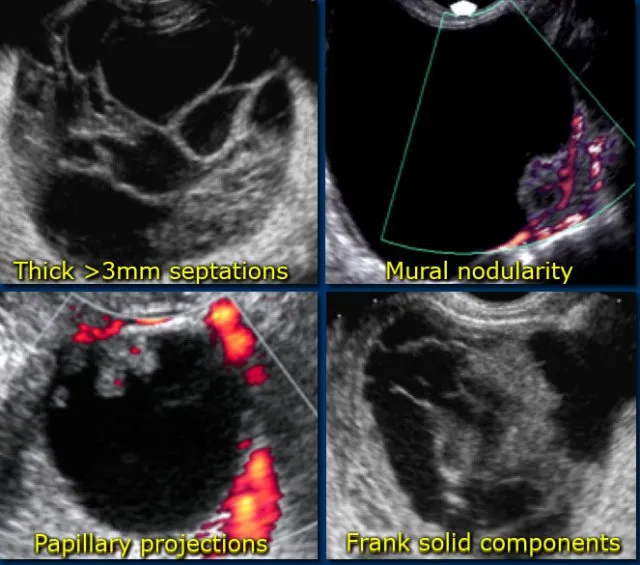
- Suspicious Features: Complex (solid & cystic), thick septations (>3 mm), papillary projections, solid nodules, increased vascularity on Doppler, ascites.
- Tumor Markers: Used adjunctively, not for screening.
- CA-125: Elevated in epithelial ovarian cancer.
- Germ Cell Tumors: Consider AFP, β-hCG, LDH in younger patients.
⭐ CA-125 is most useful in postmenopausal women. In premenopausal women, it's non-specific and can be elevated by endometriosis, fibroids, or PID.
✂️ Management - Snip or Spare?
-
Ovarian Cystectomy (Spare):
- "Shells out" the cyst, preserving ovarian tissue.
- Goal: Maintain fertility & hormonal function.
- Indicated for: Benign-appearing cysts (e.g., dermoid, endometrioma) in premenopausal women.
-
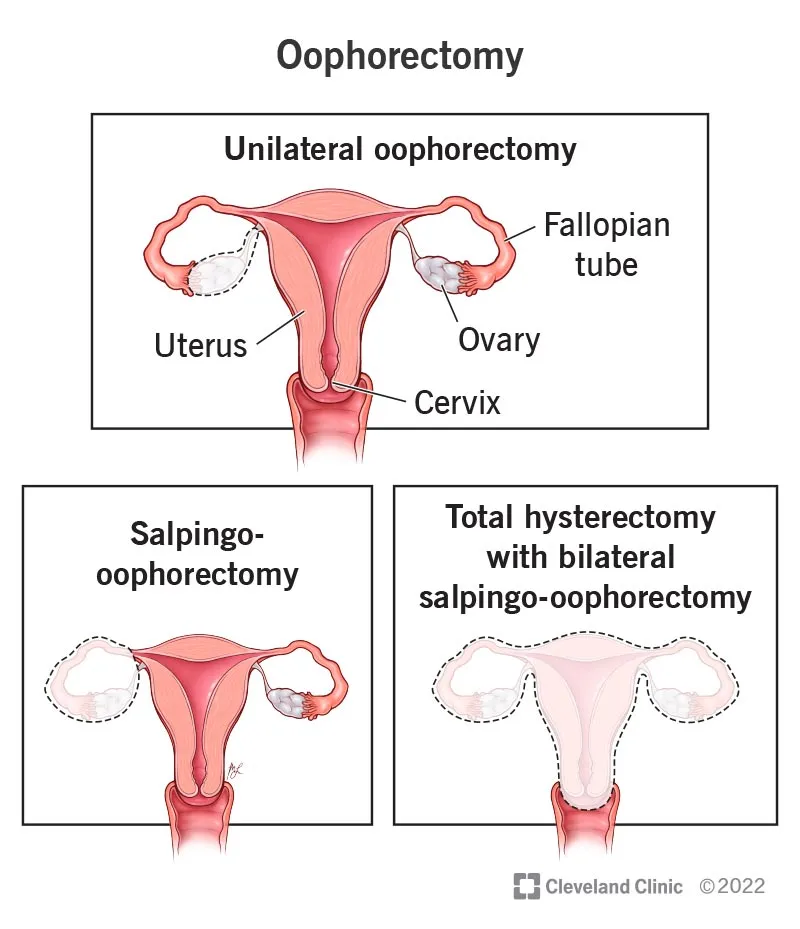
Salpingo-oophorectomy (Snip):
- Removal of ovary and fallopian tube.
- Indicated for: High suspicion of malignancy, most masses in postmenopausal women, or necrotic ovary post-torsion.
⭐ Intraoperative Frozen Section: Crucial for suspicious masses. If malignancy is found, the procedure may be staged to a full gynecologic cancer surgery (e.g., hysterectomy, BSO, lymphadenectomy).
⚠️ Complications - Post-Op Pitfalls
- Hemorrhage: From the ovarian pedicle (infundibulopelvic or utero-ovarian ligament).
- Adjacent Organ Injury: High risk to the ureter, which runs near the infundibulopelvic ligament; also bladder, bowel.
- ↓ Ovarian Reserve: Inadvertent removal of healthy tissue during cystectomy, impacting fertility.
- Surgical Menopause: Abrupt onset with bilateral oophorectomy (BSO) in premenopausal women.
- Adhesions: Can cause chronic pain or bowel obstruction.
⭐ Ovarian Remnant Syndrome (ORS): Presents as cyclical pelvic pain post-BSO. Diagnosed via imaging and labs (↓FSH, ↑estradiol) confirming functional remnant tissue.
⚡ Biggest Takeaways
- Cystectomy is the standard for premenopausal women to preserve fertility and ovarian function, especially for benign-appearing cysts.
- Oophorectomy is indicated for high suspicion of malignancy, complex masses in postmenopausal women, or a non-viable torsed ovary.
- Laparoscopy is the preferred surgical approach over laparotomy due to lower morbidity.
- Ovarian torsion is a surgical emergency requiring prompt detorsion; cystectomy or oophorectomy is performed based on ovarian viability.
- Bilateral oophorectomy induces surgical menopause; counsel on and consider hormone replacement therapy.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

