🗺️ Anatomy: Key Structures - The Pancreas Unveiled
- Location: Primarily retroperitoneal (📌 SAD PUCKER), nestled in the duodenal C-loop.
- Key Parts & Relations:
- Head: Cradled by duodenum; common bile duct (CBD) passes through.
- Uncinate Process: Hooks behind the Superior Mesenteric Vein (SMV) & Artery (SMA).
- Neck: Overlies the portal vein confluence (SMV + Splenic Vein).
- Body: Crosses aorta and L2 vertebra.
- Tail: Intraperitoneal; within splenorenal ligament, abuts splenic hilum.
- Ductal System:
- Main (Wirsung): Joins CBD at Ampulla of Vater.
- Accessory (Santorini): Drains superior head.
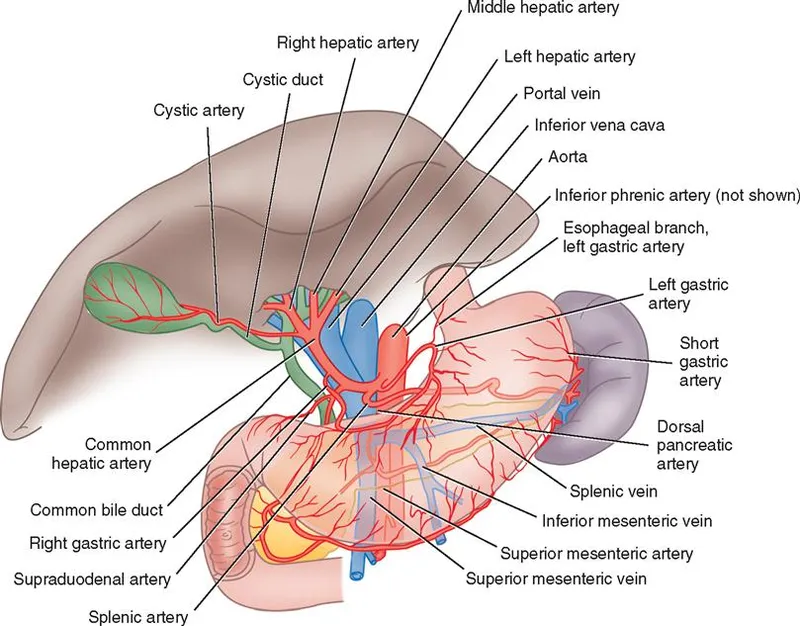
⭐ The uncinate process's posterior relationship to the SMA/SMV is a critical dissection point during a Whipple procedure.
🔪 Core concept: The Procedures - Scalpel Superstars
Decision-making is primarily based on tumor location.
| Procedure | Key Resections | Key Anastomoses |
|---|---|---|
| Whipple | Pancreatic head, duodenum, gallbladder, CBD | Pancreaticojejunostomy, Hepaticojejunostomy, Gastro/Duodenojejunostomy |
| Distal | Pancreatic body/tail ± spleen | None (stapled pancreatic stump) |
| Total | Entire pancreas, spleen, duodenum, etc. | Hepaticojejunostomy, Gastrojejunostomy |
- Drainage Procedures (for Chronic Pancreatitis):
- Puestow: For dilated duct (>6 mm); lateral pancreaticojejunostomy.
- Frey: Puestow + coring out of the pancreatic head.
⭐ Pancreatic Fistula (POPF) is the most feared complication. Defined by drain output with amylase >3x serum level after Post-Op Day 3. Delayed Gastric Emptying (DGE) is the most common.
🚧 Complications: Post-Op Problems - Surgical Setbacks
- Pancreatic Fistula (POPF): Most common & feared major complication.
- Dx: Drain fluid amylase >3x serum upper limit of normal after POD #3.
- Mgmt: NPO, TPN, octreotide, drain management, antibiotics if infected.
⭐ A new fever with leukocytosis and high drain amylase post-Whipple strongly suggests a clinically relevant POPF, which can lead to sepsis or hemorrhage.
-
Delayed Gastric Emptying (DGE):
- Inability to tolerate oral diet by POD 7-10.
- Mgmt: NGT decompression, prokinetics (e.g., metoclopramide).
-
Post-Pancreatectomy Hemorrhage (PPH):
- Early (<24h): Technical error.
- Late (>24h): Often due to fistula eroding a vessel (e.g., GDA stump).
- Dx/Tx: Angiography with embolization is preferred over surgery.
🗺️ Management: The Aftermath - Recovery Roadmap
- Immediate Care: ICU/step-down monitoring. Close watch on hemodynamics, glucose levels, and surgical drain output. Check drain fluid amylase daily.
- Nutrition Pathway: Start NPO. Early enteral nutrition via nasojejunal (NJ) tube is often preferred over TPN to maintain gut integrity. Advance oral diet as bowel function returns.
- Common Hurdles:
- Pancreatic Fistula (POPF): Drain amylase >3x serum level after POD 3.
- Delayed Gastric Emptying (DGE): Inability to tolerate oral diet by POD 7, requiring NG tube.
- Post-pancreatectomy Hemorrhage (PPH): Early (<24h) vs. Late (>24h).
⭐ Clinically relevant pancreatic fistula (CR-POPF, ISGPS Grade B/C) is the most feared complication, associated with significant morbidity and requiring interventions like drainage or reoperation.
⚡ Biggest Takeaways
- Whipple procedure (pancreaticoduodenectomy) is the standard for pancreatic head masses; removes the head, duodenum, gallbladder, and distal bile duct.
- Distal pancreatectomy is for tumors in the pancreatic body/tail, often requiring splenectomy due to shared blood supply.
- Total pancreatectomy is rare, causing brittle diabetes and exocrine insufficiency.
- The most feared complication is a pancreatic fistula, diagnosed by high amylase in drain fluid.
- Delayed gastric emptying is a common post-Whipple complication, managed conservatively.
- Frey/Puestow procedures decompress the pancreatic duct in chronic pancreatitis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

