🔪 Gutsy Decisions
- Primary Indications: Colorectal Cancer (CRC), Inflammatory Bowel Disease (IBD), complicated or recurrent diverticulitis, and familial polyposis syndromes (e.g., FAP).
- Pre-op Optimization: Mechanical bowel prep + oral antibiotics (Neomycin/Erythromycin) significantly reduces surgical site infection risk. IV antibiotics given pre-incision.
- Post-op Management: Enhanced Recovery After Surgery (ERAS) protocols are standard. Emphasizes early ambulation, early oral intake, and opioid-sparing analgesia to speed recovery and reduce ileus.
⭐ Anastomotic leak is the most feared complication, often presenting on post-op day 5-7. Key signs: fever, tachycardia, abdominal pain, ↑ WBC. Diagnose with CT using oral/rectal contrast.
📋 Management - Pre-Op Playbook
- Bowel Prep: Combined mechanical (e.g., polyethylene glycol) and oral antibiotics (Neomycin + Metronidazole).
- IV Antibiotics: Prophylactic dose <60 min before incision.
- Standard: Cefoxitin or Cefotetan.
- PCN Allergy: Clindamycin + Gentamicin.
- VTE Prophylaxis: Pre-op LMWH or UFH.
- Nutrition: Screen for malnutrition (albumin <3.0 g/dL, >10% weight loss).
- 💡 ERAS Protocols: Carbohydrate loading up to 2 hrs pre-op; avoid prolonged fasting.
⭐ Mechanical bowel prep combined with oral antibiotics is superior to either alone in reducing surgical site infections (SSIs).
🛠️ Management - The Surgeon's Toolkit
-
Surgical Approaches: Open, Laparoscopic, or Robotic-assisted. Laparoscopic is preferred (↓pain, ↓length of stay, faster recovery).
-
Types of Resection:
- Colectomy: Right, left, sigmoid, subtotal, or total abdominal colectomy (TAC).
- Proctectomy:
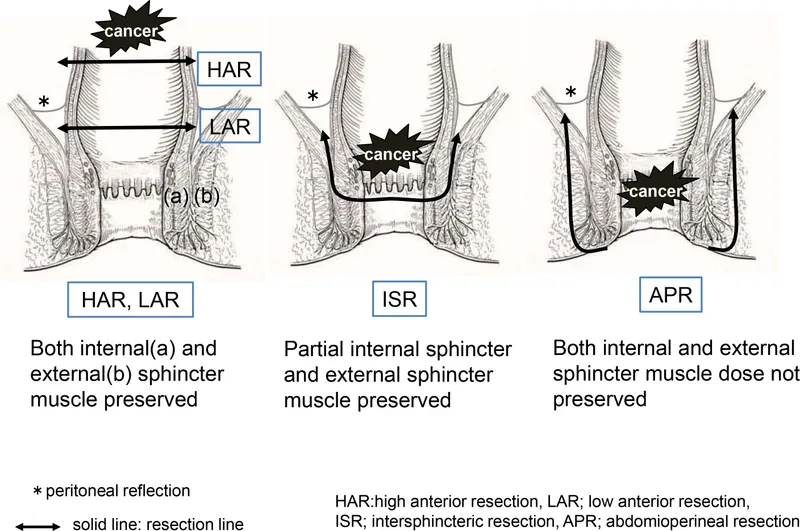
- Low Anterior Resection (LAR): Sphincter-sparing; for mid-to-upper rectal tumors.
- Abdominoperineal Resection (APR): Removes anus/sphincter; for low rectal tumors.
-
Reconstruction Options:
- Anastomosis: Primary connection of bowel ends.
- Ostomy: Ileostomy (liquid stool) or Colostomy (formed stool).
- Pouch: Ileal Pouch-Anal Anastomosis (IPAA) after TAC for FAP/UC.
⭐ LAR vs. APR: The key determinant is the tumor's distance from the anal sphincter. LAR preserves continence; APR requires a permanent end colostomy.
🚑 Complications - The Aftermath
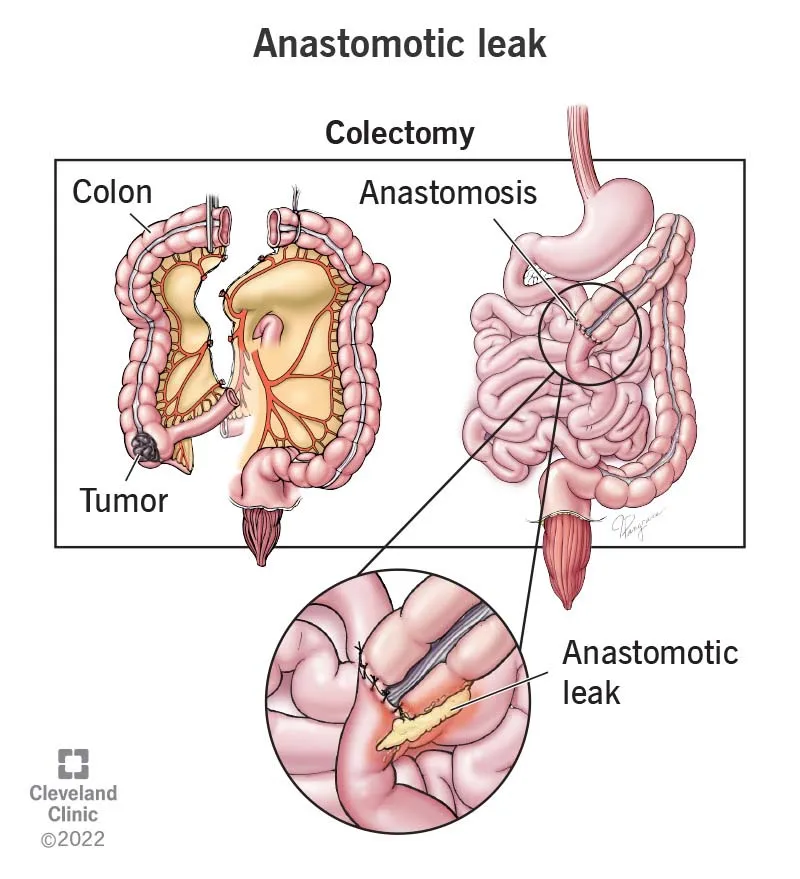
- Anastomotic Leak (POD 5-7): Most feared. Presents with fever, tachycardia, pain, ↑WBC. Highest risk in low anterior resections (LAR) and patients with risk factors (smoking, malnutrition).
- Post-op Ileus: Common (resolves in 3-5 days). Differentiate from early SBO, which presents later with a clear transition point on CT.
- Pelvic Nerve Injury (during TME):
- Superior hypogastric plexus → Retrograde ejaculation.
- Pelvic splanchnic nerves (nervi erigentes) → Erectile/bladder dysfunction.
- Surgical Site Infection (SSI): Superficial, deep, or organ/space (abscess).
⭐ A change in drain output from serosanguinous to purulent or feculent is a classic, high-yield sign of an anastomotic leak.
Management of Suspected Leak:
⚡ Biggest Takeaways
- Bowel prep with oral antibiotics (e.g., neomycin, metronidazole) is standard to decrease Surgical Site Infections (SSI).
- Right hemicolectomy for right-sided tumors involves an ileocolic anastomosis.
- Low Anterior Resection (LAR) is sphincter-sparing for upper/mid-rectal cancers.
- Abdominoperineal Resection (APR) for low rectal cancer (<5 cm from verge) requires a permanent colostomy.
- The most feared complication of LAR is an anastomotic leak, presenting with fever and peritonitis.
- Post-op surveillance includes CEA monitoring and colonoscopy at 1 year.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

