🗺️ Anatomy - The Surgical Map
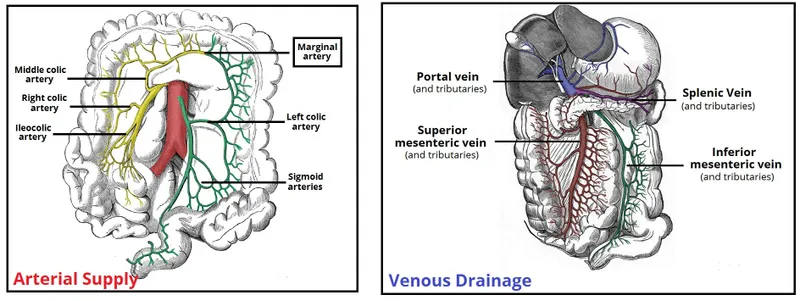
- Arterial Supply & Lymphatics (Follow Arteries):
- Midgut (SMA): Cecum to proximal 2/3 transverse colon.
- Branches: Ileocolic, Right Colic, Middle Colic arteries.
- Lymph: Drains to central SMA nodes.
- Hindgut (IMA): Distal 1/3 transverse colon to upper rectum.
- Branches: Left Colic, Sigmoid, Superior Rectal arteries.
- Lymph: Drains to central IMA nodes.
- Rectum: Dual supply & drainage.
- Superior/Middle: IMA/Internal Iliac arteries.
- Lower: Internal Pudendal artery.
- Midgut (SMA): Cecum to proximal 2/3 transverse colon.
⭐ Rectal Drainage Divide: Cancers above the dentate line drain superiorly to inferior mesenteric nodes (portal). Cancers below drain to superficial inguinal nodes (systemic). Middle rectal cancers can also drain laterally to internal iliac nodes.
🔪 Oncologic Principles
The goal is curative resection by removing the primary tumor, its lymphatic drainage, and ensuring clear margins to prevent recurrence.
- No-touch Isolation: Minimal tumor handling before vascular ligation to prevent hematogenous/lymphatic spread.
- High Ligation: Ligate the main feeding artery (e.g., IMA) at its origin to resect the entire lymphatic basin.
- En-bloc Resection: Remove the tumor with any adherent structures as one intact specimen, avoiding tumor violation.
- Oncologic Margins:
- Proximal/Distal: ≥5 cm of normal bowel.
- Radial (CRM): ≥1 mm of uninvolved circumferential tissue.
⭐ A positive Circumferential Resection Margin (CRM < 1 mm) is the strongest predictor of local recurrence in rectal cancer.
🔪 Management - The Surgical Playbook
Surgical approach is determined by tumor location, aiming for en-bloc resection with negative margins and adequate lymphadenectomy.
-
Colon Resection:
- Resect tumor segment with its primary lymphovascular pedicle.
- Margins: ≥5 cm proximal/distal.
- Lymphadenectomy: Harvest ≥12 nodes for staging.
-
Rectal Resection:
- 💡 Total Mesorectal Excision (TME): Standard of care. Removes rectum + mesorectum as an intact package, drastically ↓ local recurrence.
- Distal margin: >1-2 cm.
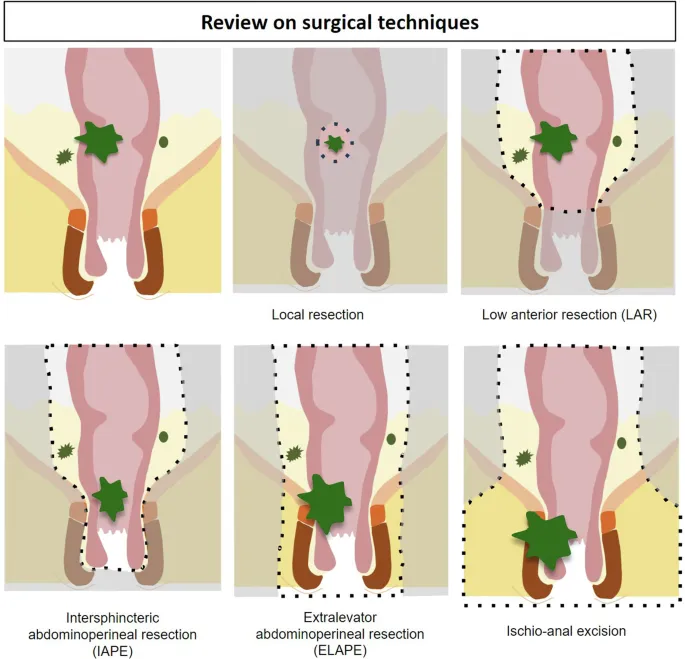
- LAR: Sphincter-sparing; anastomosis created.
- APR: Sphincter removed; permanent end colostomy.
⭐ Neoadjuvant chemoradiation (nCRT) is standard for most T3/T4 or node-positive rectal cancers. It helps downstage tumors, increasing rates of sphincter preservation and R0 resection.
⚠️ Complications - When Resections Go Rogue
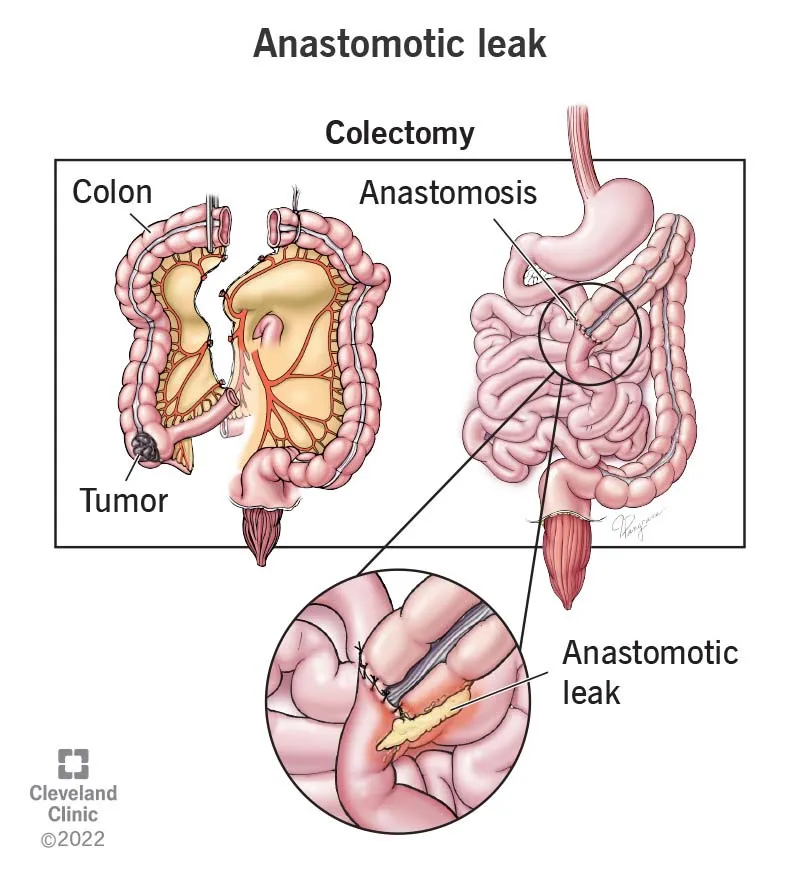
- Anastomotic Leak: Most feared complication. Presents with fever, tachycardia, ↑ WBC, and abdominal pain. Diagnosis via CT with contrast. Requires urgent intervention (drainage, antibiotics, possible re-operation/diversion).
- Surgical Site Infection (SSI): Can be superficial (cellulitis) or deep/organ space (intra-abdominal abscess). Requires drainage and antibiotics.
- Pelvic Nerve Injury: Risk in low anterior resection (LAR).
- Sympathetic (Hypogastric n.): Ejaculatory dysfunction.
- Parasympathetic (Pelvic Splanchnic n.): Erectile/bladder dysfunction.
- Stoma Complications: Includes retraction, prolapse, stenosis, parastomal hernia, and skin irritation.
⭐ Anastomotic leaks classically present on post-op days 5-7. Suspect in any patient with new-onset tachycardia, fever, or leukocytosis after colorectal surgery.
⚡ High-Yield Points - Biggest Takeaways
- Anatomic resection is key, removing the tumor with its primary lymphovascular supply.
- The goal is R0 resection (negative margins): ≥ 5 cm for colon, ≥ 2 cm distally for rectum.
- Harvesting ≥ 12 lymph nodes is mandatory for accurate pathologic N-staging.
- Total Mesorectal Excision (TME) is standard for mid/low rectal cancers to reduce local recurrence.
- Neoadjuvant chemoradiation is used for Stage II/III rectal cancers to downstage tumors.
- Resection of isolated liver or lung metastases can be curative.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

