Blood Components - The Blood Bag Breakdown
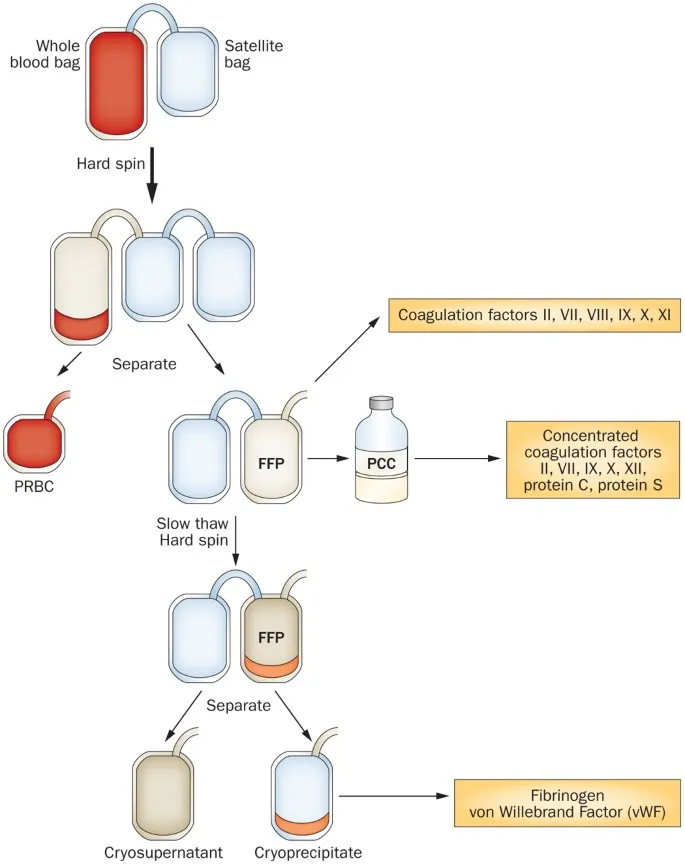
- Packed Red Blood Cells (PRBCs)
- Use: ↑ O₂ carrying capacity for anemia or acute blood loss.
- Effect: 1 unit ↑ Hb by 1 g/dL & Hct by 3%.
- Platelets
- Use: For thrombocytopenia or platelet dysfunction.
- Thresholds: Give if <50,000/μL for surgery, or <10,000/μL for spontaneous bleed risk.
- Fresh Frozen Plasma (FFP)
- Use: Replaces all clotting factors.
- Indications: Coagulopathy (liver disease, DIC), urgent warfarin reversal.
- Cryoprecipitate
- Contains: Fibrinogen, Factor VIII, vWF, Factor XIII.
- Use: Hypofibrinogenemia (<100 mg/dL).
⭐ FFP is preferred for rapid warfarin reversal over Vitamin K due to its immediate supply of all coagulation factors.
Transfusion Indications - When to Open the Tap
-
Packed Red Blood Cells (PRBCs)
- Hb < 7 g/dL in stable, hospitalized patients.
- Hb < 8 g/dL in patients with cardiovascular disease or post-op.
- Symptomatic anemia (e.g., chest pain, dyspnea) or active hemorrhage.
-
Platelets
- Prophylactically if < 10,000/μL.
- Pre-procedure or active bleeding if < 50,000/μL.
-
Fresh Frozen Plasma (FFP)
- For coagulopathy (INR > 1.5) with active bleeding or pre-procedure.
- Warfarin reversal (when PCC is unavailable).
-
Cryoprecipitate
- For hypofibrinogenemia (< 100-150 mg/dL).
⭐ Massive Transfusion Protocol (MTP): In trauma or massive hemorrhage, use a 1:1:1 ratio of PRBCs:FFP:Platelets to prevent dilutional coagulopathy.
Transfusion Reactions - When Good Blood Goes Bad
- Immediate Steps: Stop transfusion, maintain IV access (0.9% saline), check for clerical errors, and notify the blood bank.
| Reaction Type | Onset | Pathophysiology | Key Features |
|---|---|---|---|
| Acute Hemolytic | < 1 hr | ABO incompatibility | Fever, flank pain, hemoglobinuria, +Direct Coombs |
| FNHTR | 1-6 hrs | Cytokines from donor WBCs | Fever, chills. Prevent w/ leukoreduction. |
| Allergic | < 1 hr | IgE vs. plasma proteins | Urticaria, pruritus. Give antihistamines. |
| Anaphylactic | Seconds | Anti-IgA in IgA-deficient pt | Shock, angioedema. Give epinephrine. |
| TRALI | < 6 hrs | Donor anti-leukocyte Abs | Non-cardiogenic pulmonary edema (ARDS) |
| TACO | < 6 hrs | Volume overload | Cardiogenic pulmonary edema, ↑JVP, ↑BNP |
Massive Transfusion - The 1:1:1 Protocol
- Definition: Replacement of >1 blood volume in 24h, >10 units of pRBCs in 24h, or >4 units in 1h.
- 1:1:1 Protocol: Balanced transfusion with a ratio of 1 unit packed red blood cells (pRBCs) : 1 unit fresh frozen plasma (FFP) : 1 unit platelets.
- Goal: Mimic whole blood to prevent/treat coagulopathy, acidosis, & hypothermia (lethal triad).
- Complications: Hypocalcemia (citrate toxicity), hyperkalemia, hypothermia.
⭐ The 1:1:1 protocol has been shown to decrease mortality, reduce total blood product usage, and achieve hemostasis faster in trauma patients.
High‑Yield Points - ⚡ Biggest Takeaways
- Packed Red Blood Cells (PRBCs) ↑ O₂-carrying capacity; 1 unit raises Hb by 1 g/dL.
- Give platelets for thrombocytopenia or dysfunction, but avoid in TTP/HUS without severe bleeding.
- Fresh Frozen Plasma (FFP) replaces all clotting factors; reverses warfarin and treats coagulopathy.
- Cryoprecipitate provides concentrated fibrinogen, Factor VIII, and vWF; used for hypofibrinogenemia.
- Febrile non-hemolytic is the most common reaction; acute hemolytic is the most severe.
- O-negative is the universal RBC donor; AB is the universal plasma donor.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

