🩺 Diagnosis - First Steps & Suspicions
- Initial Presentation: Most nodules are asymptomatic, discovered incidentally.
- ⚠️ Red Flags for Malignancy:
- Rapid growth, hoarseness, dysphagia.
- History of head/neck radiation.
- Family history (e.g., MEN2, RET proto-oncogene).
- Firm, fixed nodule; cervical lymphadenopathy.
⭐ The first step in evaluating a thyroid nodule is always measuring the serum TSH level. This determines if the nodule is hyperfunctioning ("hot") or non-functioning ("cold"), guiding the subsequent workup.
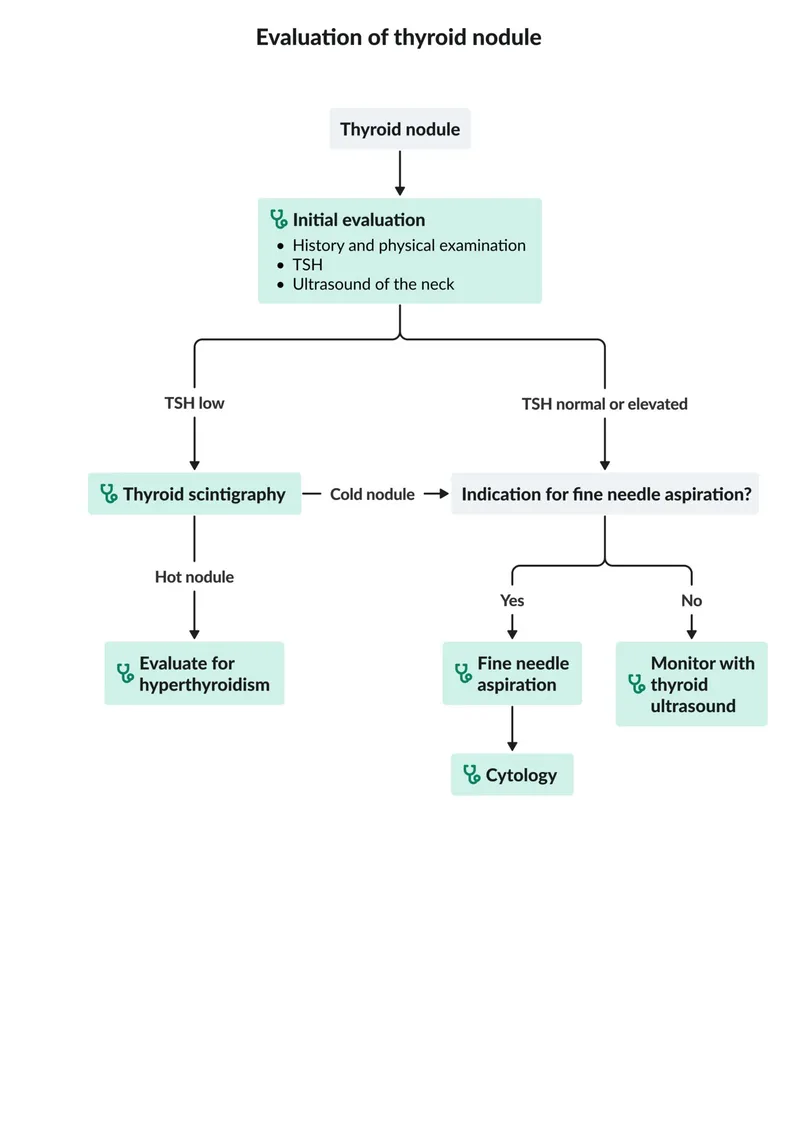
👁️ Radiology - Ultrasound's Sharp Eyes
Ultrasound is the primary imaging modality to risk-stratify nodules and determine the need for FNA. The ACR TI-RADS system standardizes reporting by assigning points to suspicious features.
- High-Risk Features (↑ Malignancy):
- Solid & Markedly Hypoechoic: Darker than adjacent strap muscle.
- Microcalcifications: Punctate echogenic foci <1 mm.
- Irregular Margins: Infiltrative, spiculated, or microlobulated.
- Taller-than-Wide Shape: Suggests aggressive, infiltrative growth.
- Extrathyroidal Extension: Obvious invasion into surrounding tissues.
- Low-Risk Features: Purely cystic (anechoic), spongiform/honeycomb appearance (aggregate of microcysts), isoechoic/hyperechoic.
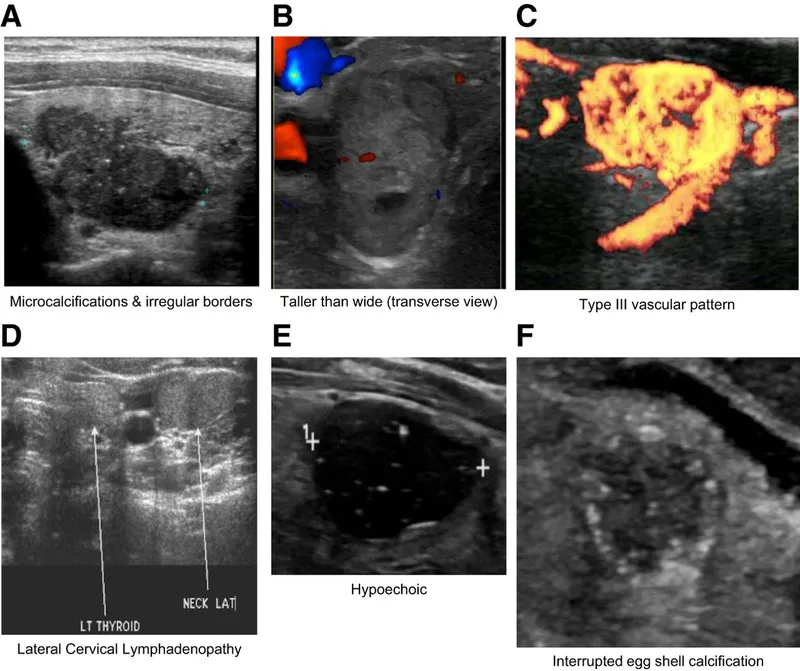
⭐ Microcalcifications are the most specific ultrasound finding for papillary thyroid carcinoma (PTC), often representing psammoma bodies.
Pathology - Cells Tell The Tale
Error: Failed to generate content for this concept group.
🔪 Management - The Decisive Cut
Management is guided by Fine Needle Aspiration (FNA) cytology (Bethesda system).
- Indeterminate (III/IV): Repeat FNA, molecular testing, or diagnostic lobectomy.
- Suspicious/Malignant (V/VI): Surgical resection.
- Lobectomy: For small (<4 cm), unifocal, low-risk tumors.
- Total Thyroidectomy: For large tumors (>4 cm), bilateral disease, or metastasis.
⭐ For indeterminate nodules (Bethesda III/IV), molecular testing (e.g., Afirma, ThyroSeq) on the FNA sample can help rule out malignancy, potentially avoiding diagnostic surgery.
⚡ Biggest Takeaways
- Initial evaluation is always TSH and thyroid ultrasound.
- If TSH is low, perform a radionuclide scan; "hot" nodules are rarely malignant and don't need FNA.
- If TSH is normal/high, use ultrasound findings to guide Fine-Needle Aspiration (FNA).
- FNA is the single most accurate test to diagnose thyroid cancer.
- High-risk US features prompting FNA: microcalcifications, irregular margins, hypoechogenicity, taller-than-wide shape.
- Malignant FNA requires surgery (thyroidectomy).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

