🔬 Pathology - The Cancer Quartet
| Type | Prevalence | Histology Buzzwords | Key Features |
|---|---|---|---|
| Papillary | ~85% | Orphan Annie eyes, psammoma bodies, nuclear grooves | Excellent prognosis; lymphatic spread |
| Follicular | ~10% | Capsular/vascular invasion | Hematogenous spread (bone, lung) |
| Medullary | ~3% | Amyloid stroma (Congo red+), polygonal cells | From parafollicular C-cells; ↑ Calcitonin |
| Anaplastic | <2% | Pleomorphic giant cells | Elderly; dismal prognosis; local invasion |
⭐ Medullary Thyroid Cancer (MTC) is associated with MEN 2A and 2B syndromes. Always test for RET proto-oncogene mutations.
🕵️ Diagnosis - Nodule Detective Work
The primary goal is to identify the ~5-10% of nodules that are malignant.
- Step 1: TSH Level
- If TSH is low (↓), suspect a hyperfunctioning ("hot") nodule.
- Step 2: Imaging
- Low TSH: Radionuclide Iodine Uptake (RAIU) scan.
- "Hot" nodule: Benign. Treat hyperthyroidism.
- "Cold" nodule: Higher malignancy risk. Proceed to FNA.
- Normal/High TSH: Thyroid Ultrasound (US) is the next step.
- Low TSH: Radionuclide Iodine Uptake (RAIU) scan.
- Step 3: Fine-Needle Aspiration (FNA)
- Gold standard, guided by US.
- ⚠️ Suspicious US features: Microcalcifications, hypoechogenicity, irregular margins, taller-than-wide.
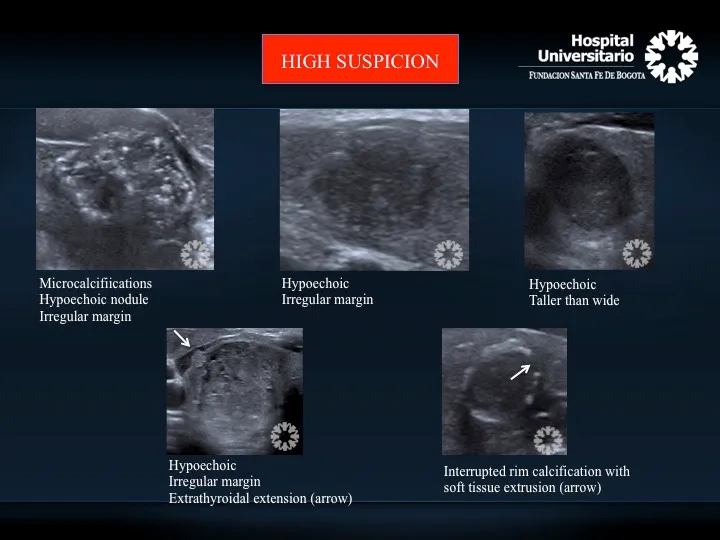
⭐ FNA is highly accurate but has a key limitation: it cannot distinguish follicular adenoma from follicular carcinoma. This distinction requires surgical excision to assess for capsular or vascular invasion.
🔪 Management - The Surgeon's Scalpel
Surgical approach is tailored to tumor type, size, and risk factors.
- Post-Op Adjuncts & Monitoring:
- Radioactive Iodine (RAI; ¹³¹I): For remnant ablation post-total thyroidectomy in high-risk differentiated cancers.
- TSH Suppression: Levothyroxine therapy to keep TSH low, reducing growth stimulus.
- Tumor Markers: Monitor Thyroglobulin (Tg) for papillary/follicular; Calcitonin for medullary.
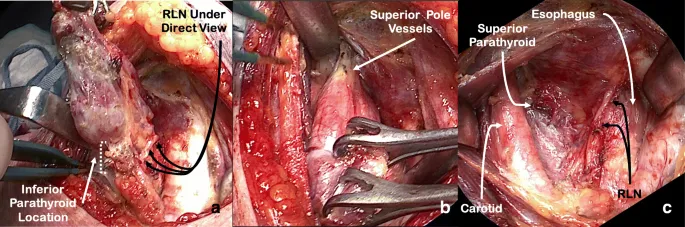
⭐ Post-thyroidectomy, always monitor for hypocalcemia (Chvostek/Trousseau signs). It's the most common complication due to inadvertent parathyroid gland removal or devascularization.
⚠️ Complications - Post-Op Pitfalls
- Hypocalcemia (↓ $Ca^{2+}$): Most common; due to parathyroid injury/removal.
- S/S: Perioral numbness, paresthesias, Chvostek/Trousseau signs.
- Tx: IV calcium gluconate (severe), oral calcium & calcitriol.
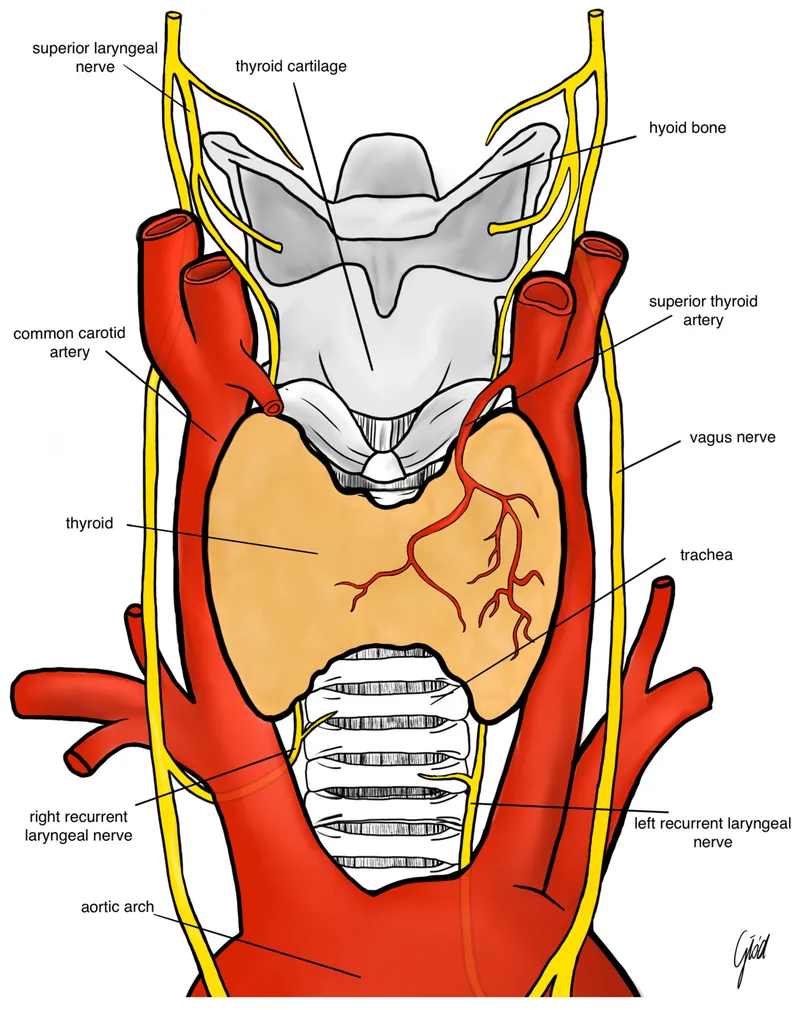
- Recurrent Laryngeal Nerve (RLN) Injury:
- Unilateral: Hoarseness, breathy voice.
- Bilateral: Stridor, airway obstruction → emergent airway.
- Superior Laryngeal Nerve (SLN) Injury: Loss of high-pitched voice.
- Hematoma: Neck swelling, can cause rapid airway compression.
⭐ Bilateral RLN injury is a surgical emergency causing acute airway obstruction from unopposed vocal cord adduction.
⚡ Biggest Takeaways
- Papillary is most common; look for Orphan Annie eyes, psammoma bodies, and lymphatic spread.
- Follicular spreads hematogenously; diagnosis requires capsular/vascular invasion on final pathology.
- Medullary arises from C-cells, produces calcitonin, and is linked to MEN 2 (RET).
- Anaplastic is a rapidly fatal cancer in the elderly.
- Workup: Ultrasound first, then Fine-Needle Aspiration (FNA) is the best initial diagnostic test.
- Treatment: Surgery is primary, followed by radioactive iodine and TSH suppression.
- Monitor recurrence with thyroglobulin (papillary/follicular) or calcitonin (medullary).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

