📉 Calcium's Nosedive
- Primary Cause: Iatrogenic hypoparathyroidism from thyroid/parathyroid surgery (gland devascularization, trauma, or removal).
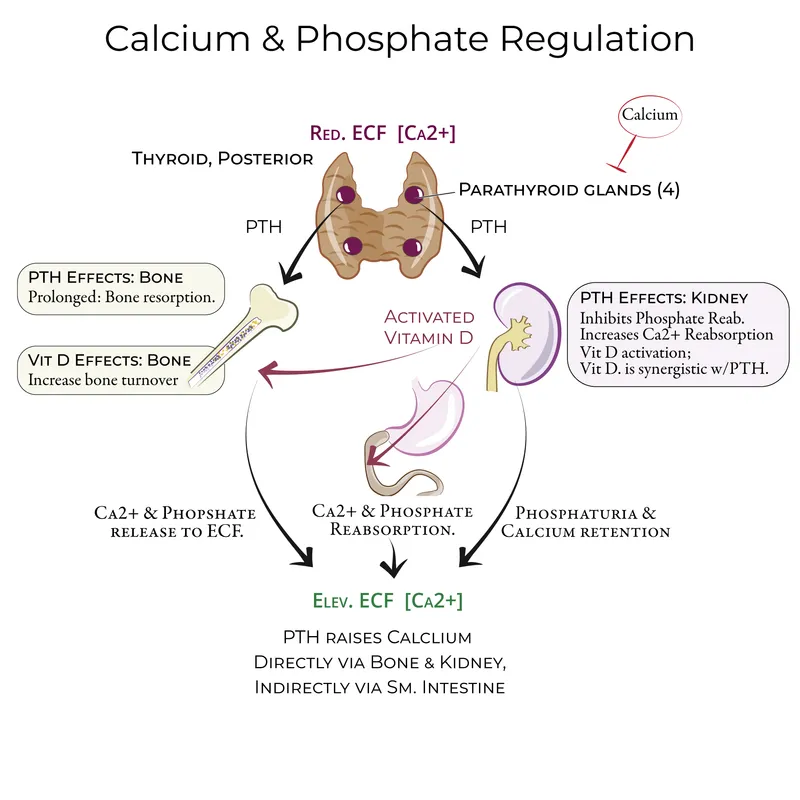
- Mechanism: Insufficient PTH (↓PTH) secretion causes:
- ↓ Bone resorption of $Ca^{2+}$.
- ↓ Renal reabsorption of $Ca^{2+}$.
- ↓ Renal 1α-hydroxylase activity → ↓ active Vitamin D.
- ↓ Intestinal $Ca^{2+}$ absorption.
- Hungry Bone Syndrome: After parathyroidectomy for severe hyperparathyroidism, bones rapidly uptake $Ca^{2+}$ and phosphate, causing profound hypocalcemia.
⭐ Hungry Bone Syndrome features severe hypocalcemia, hypophosphatemia, and hypomagnesemia, unlike transient hypoparathyroidism where phosphate is high.
📉 Clinical Manifestations - The Jittery Signs
Hypocalcemia (↓ ionized $Ca^{2+}$) increases neuronal membrane permeability to sodium, lowering the threshold for depolarization and causing neuromuscular hyperexcitability.
- Early/Mild: Paresthesias (perioral, fingers, toes), anxiety, muscle cramps.
- Latent Tetany (Provocable):
- Chvostek's Sign: Tapping the facial nerve (anterior to the ear) elicits ipsilateral facial muscle contraction.
- Trousseau's Sign: Inflating a BP cuff above systolic pressure for 3 minutes induces carpal spasm.
- Severe/Overt Tetany: Spontaneous carpopedal spasms, laryngospasm (stridor), seizures.

⭐ On EKG, hypocalcemia is classically associated with prolongation of the QT interval, which predisposes to ventricular arrhythmias like Torsades de Pointes.
🧪 Diagnosis - Confirming the Drop
- Serum Calcium: Check immediately if symptoms arise.
- Total Calcium: < 8.5 mg/dL. Requires correction for albumin.
- Ionized Calcium: < 4.65 mg/dL. The most accurate measure of active calcium.
- Albumin Correction:
- $Ca_{corrected} = Ca_{total} + 0.8 \times (4.0 - \text{Albumin})$.
- Etiology Confirmation:
- ↓ or inappropriately normal PTH level confirms iatrogenic hypoparathyroidism.
- Check Magnesium: Hypomagnesemia can cause/worsen hypocalcemia.
- ECG: Prolonged QT interval.
⭐ Ionized calcium is the gold standard. Total calcium is unreliable post-op due to ↓ albumin from surgical stress, fluid shifts, and transfusions.
🚑 Management - The Calcium Rescue
-
Acute Symptomatic Hypocalcemia:
- IV Calcium Gluconate: The immediate treatment. Administer 1-2 grams over 10-20 minutes.
- 💡 Calcium gluconate is preferred over calcium chloride for peripheral IV access due to lower risk of tissue necrosis with extravasation.
- ⚠️ Infuse slowly with EKG monitoring to prevent hypotension and life-threatening arrhythmias (bradycardia, asystole).
-
Asymptomatic or Mild Hypocalcemia:
- Oral Calcium: High-dose Calcium Carbonate (take with food) or Calcium Citrate.
- Active Vitamin D: Calcitriol ($1,25-(OH)_2D_3$) is mandatory. It acts rapidly by bypassing renal 1-alpha-hydroxylase, which is inactive without PTH.
-
Magnesium Repletion:
- Always check and correct hypomagnesemia. Low Mg²⁺ impairs PTH secretion and induces end-organ PTH resistance.
⭐ Hypocalcemia classically prolongs the QT interval on an EKG. In contrast, hypercalcemia shortens the QT interval.
⚡ Biggest Takeaways
- Most common cause is iatrogenic injury to parathyroid glands during thyroidectomy.
- Classic signs: paresthesias (perioral numbness), Chvostek's (facial twitch), and Trousseau's (carpopedal spasm) signs.
- Severe symptoms include tetany, seizures, and prolonged QT interval on EKG.
- Acute symptomatic treatment: IV calcium gluconate.
- Chronic management: Oral calcium supplements and calcitriol (activated Vitamin D).
- Hungry Bone Syndrome causes severe, prolonged hypocalcemia after parathyroidectomy for hyperparathyroidism.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

