🧬 Pathophysiology - Gland Gone Wild
- Primary: Autonomous PTH secretion.
- Solitary Adenoma (
85%), 4-Gland Hyperplasia (15%), Carcinoma (<1%).
- Solitary Adenoma (
- Secondary: Compensatory ↑PTH from chronic hypocalcemia (e.g., Chronic Renal Failure → ↓Vit D, ↑$PO_4^{3-}$).
- Tertiary: Autonomous PTH secretion after prolonged secondary stimulation (e.g., post-renal transplant).
Core Mechanism: ↑PTH → ↑Serum $Ca^{2+}$, ↓Serum $PO_4^{3-}$.
📌 Classic Presentation: "Stones (renal), bones (pain, fractures), groans (abdominal pain), and psychiatric overtones (fatigue, depression)."
⭐ In primary hyperparathyroidism, urine calcium is high/normal. In Familial Hypocalciuric Hypercalcemia (FHH), a key mimic, urine calcium is low.
🔬 Diagnosis - Pinpointing the Problem
First, confirm biochemically: ↑ Serum Calcium ($Ca^{2+}$), ↑ PTH, ↓ Serum Phosphate ($PO_4^{3-}$), and ↑ 24-hr Urine Calcium.
⭐ The diagnostic hallmark is an elevated or inappropriately normal PTH level in the setting of hypercalcemia. This distinguishes it from other causes where PTH would be suppressed.
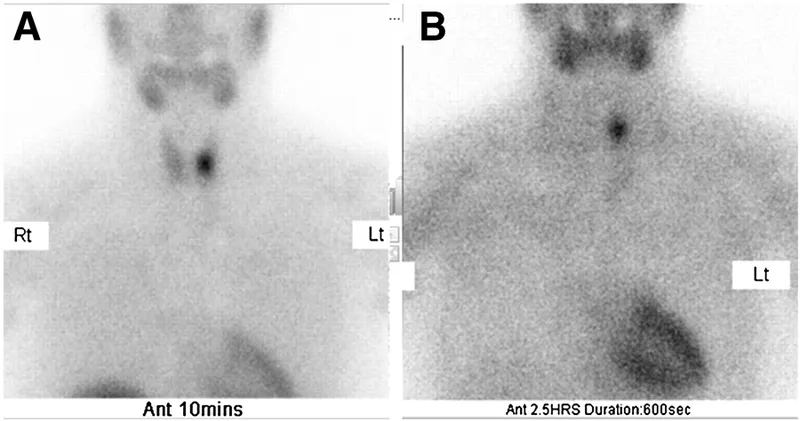
Next, pre-operative localization is key for planning minimally invasive surgery. The typical imaging workflow is:
- 4D-CT is particularly useful for localizing ectopic glands (e.g., mediastinal) or for re-operative cases.
🔪 Management - The Surgical Fix
-
Indications for Parathyroidectomy:
- Any symptomatic disease (e.g., nephrolithiasis, osteoporosis-related fractures).
- Asymptomatic patients meeting any of the following criteria:
- Age < 50 years.
- Serum Calcium > 1.0 mg/dL above the upper limit of normal.
- Creatinine clearance < 60 mL/min.
- Bone density T-score ≤ -2.5 at any site.
-
Surgical Procedures & Monitoring:
- Minimally Invasive Parathyroidectomy (MIP): For pre-operatively localized single adenomas.
- Bilateral Neck Exploration: For failed localization, suspected multigland disease (e.g., MEN), or hyperplasia.
- 💡 Intraoperative PTH (ioPTH) - Miami Criterion: Confirms successful resection with a >50% drop from baseline 10 minutes post-removal.
⭐ Post-op, beware of Hungry Bone Syndrome: severe, prolonged hypocalcemia ($Ca^{2+}$ ↓↓) due to rapid bone remineralization. Requires aggressive calcium and vitamin D supplementation.
🤕 Complications - The Aftermath
- Hypocalcemia (Most Common)
- Cause: Parathyroid stunning, devascularization, or removal.
- Symptoms: Perioral numbness, paresthesias, tetany.
- Signs: Chvostek's (facial twitch), Trousseau's (carpal spasm).
- Hungry Bone Syndrome
- Severe, prolonged ↓$Ca^{2+}$, ↓$PO_4^{3-}$, and ↓$Mg^{2+}$.
- Due to rapid bone remineralization after abrupt ↓PTH.
- Seen in severe pre-op bone disease (e.g., osteitis fibrosa cystica).
- Nerve Injury
- Recurrent Laryngeal Nerve (RLN): Unilateral → hoarseness. ⚠️ Bilateral → airway obstruction.
- Superior Laryngeal Nerve (SLN): Loss of high-pitched voice.
- Neck Hematoma
- ⚠️ Can rapidly cause airway compression; requires emergent evacuation.
⭐ Post-op hypocalcemia is the most frequent complication. Transient hypocalcemia is common, but permanent hypoparathyroidism occurs in <2% of cases.
⚡ Biggest Takeaways
- Primary hyperparathyroidism is most often a solitary adenoma; surgery is the only definitive cure.
- Indications: symptoms, age <50, serum Ca²⁺ >1 mg/dL above normal, or end-organ damage (osteoporosis, nephrolithiasis).
- Pre-op localization with Sestamibi scan and ultrasound enables minimally invasive parathyroidectomy.
- Intraoperative PTH (ioPTH) drop of >50% from baseline confirms successful resection.
- Key complications: recurrent laryngeal nerve injury (hoarseness) and post-op hypocalcemia ("hungry bone syndrome").
- Suspect MEN syndromes with multigland disease, often requiring subtotal parathyroidectomy.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

