🚪 The Failing Gates
Intervention for severe valvular disease is indicated for:
- Symptom onset (dyspnea, angina, syncope).
- LV dysfunction (e.g., EF < 60% in MR, < 50% in AS/AR).
- Significant LV dilation.
⭐ In aortic stenosis, symptoms (Angina, Syncope, Heart Failure - 📌 "ASH") are a critical indication for replacement, as symptom onset carries a poor prognosis.
🚪 Anatomy - Heart's Hinged Doors
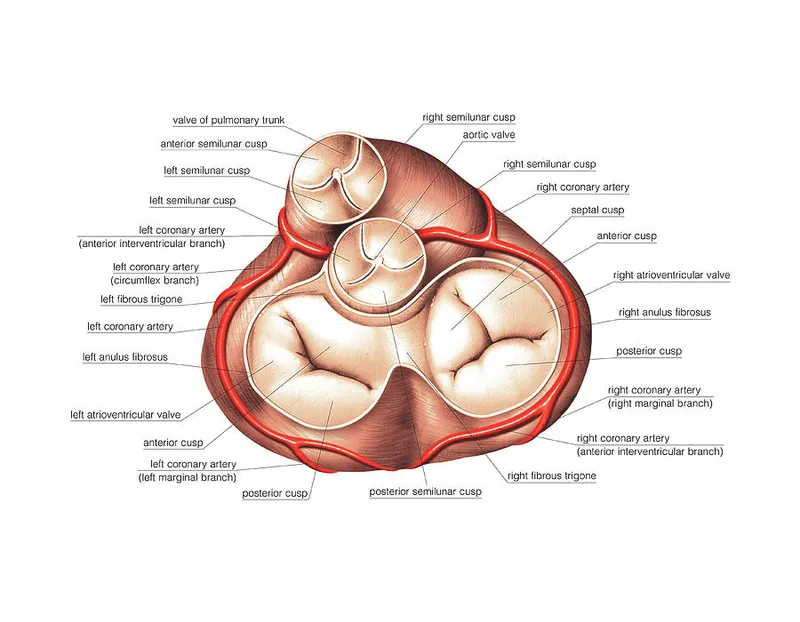
- Four Valves: Control unidirectional blood flow. 📌 Mnemonic: Try Pulling My Aorta.
- Atrioventricular (AV) Valves: Supported by chordae tendineae & papillary muscles.
- Tricuspid: 3 leaflets (RA → RV).
- Mitral (Bicuspid): 2 leaflets (LA → LV).
- Semilunar (SL) Valves:
- Aortic: 3 cusps (LV → Aorta).
- Pulmonary: 3 cusps (RV → Pulmonary Artery).
- Annulus: Fibrous ring forming the valve's "door frame"; key surgical anchor point.
⭐ The mitral valve apparatus is the most complex, making it a frequent target for intricate repair procedures over simple replacement to preserve LV function.
🔧 Management - A Mechanic's Choice
- Valve Repair: Preferred over replacement when feasible, especially for degenerative mitral regurgitation. Preserves native valve geometry, avoids lifelong anticoagulation, and has lower operative mortality.
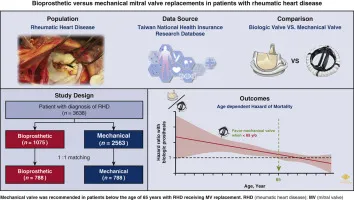
| Feature | Mechanical Valve | Bioprosthetic (Tissue) Valve |
|---|---|---|
| Durability | Very high (>20 yrs); risk of pannus | Lower (10-15 yrs); risk of structural failure |
| Thrombogenicity | High; audible "click" | Low; silent operation |
| Anticoagulation | Lifelong Warfarin | 3-6 months post-op, then often ASA |
| Ideal Patient | Younger (<60-65 yrs), compliant | Older (>65 yrs), non-compliant, pregnancy planned |
⚠️ Endocarditis Prophylaxis: Required for all prosthetic valves and valve repairs using prosthetic material before certain dental/respiratory procedures.
⚠️ Complications - Post-Op Perils
-
Early (<30 days):
- Arrhythmias: New-onset AFib (most common); heart block (risk with AVR near AV node).
- Bleeding/Tamponade: Beck's triad (hypotension, JVD, muffled heart sounds).
- Thromboembolism: Ischemic stroke risk.
- Post-pericardiotomy Syndrome: Autoimmune; fever, pleuritic pain, effusion 1-6 wks post-op.
-
Late (>30 days):
- Prosthetic Valve Endocarditis (PVE): Early (<1yr) S. aureus; Late (>1yr) Viridans strep.
- Valve Dysfunction: Thrombosis, pannus, paravalvular leak (PVL), structural deterioration (bioprosthetic).
- Hemolysis: Mechanical valves > bioprosthetic; see schistocytes, ↑LDH.
⭐ Pearl: New-onset heart block after aortic valve replacement suggests potential injury to the AV node or a perivalvular abscess. Requires immediate investigation.
⚡ Biggest Takeaways
- Mechanical valves are durable but require lifelong warfarin (INR 2.5-3.5 for mitral, 2.0-3.0 for aortic).
- Bioprosthetic valves are less durable (10-15 yrs) but avoid long-term anticoagulation; preferred in older patients.
- Indications: Symptomatic severe disease or asymptomatic with LV dysfunction (EF < 50%).
- Prosthetic valves require endocarditis prophylaxis for high-risk procedures (e.g., dental).
- TAVR is a less invasive option for high-risk aortic stenosis patients.
- Mitral valve repair is favored over replacement for regurgitation to preserve LV function.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

