🌬️ Core Concept - Air in the Wrong Place
Air in the pleural space between visceral/parietal pleura, causing lung collapse due to loss of negative intrapleural pressure.
- Spontaneous:
- Primary (PSP): No underlying lung disease. Classic: tall, thin young men from ruptured apical blebs.
- Secondary (SSP): Complication of lung disease (COPD, CF, Marfan).
- Traumatic:
- Iatrogenic: From procedures (central line, thoracentesis) or barotrauma (mechanical ventilation).
- Tension: ⚠️ Life-threatening emergency.
- One-way valve mechanism. Air enters, can't exit → mediastinal shift, ↓ venous return, hemodynamic collapse.
⭐ Tension pneumothorax is a clinical diagnosis (hypotension, JVD, absent breath sounds). Do not delay needle decompression for a chest X-ray.

🩺 Diagnosis - Spotting the Collapse
-
Clinical Presentation:
- Acute onset, sharp pleuritic chest pain & dyspnea.
- Often in tall, thin young men (spontaneous) or with trauma/lung disease.
- ⚠️ Tension Pneumothorax: Hypotension, JVD, cyanosis (medical emergency).
-
Physical Exam:
- Unilateral ↓ breath sounds.
- Hyperresonance to percussion.
- ↓ Tactile fremitus.
- Tracheal deviation away from the affected side (tension).
-
Imaging:
- Chest X-ray (CXR):
- Visceral pleural line with absent lung markings peripherally.
- Best seen on expiratory film.
- Ultrasound (POCUS):
- Absence of lung sliding; "barcode sign" on M-mode.
- Chest X-ray (CXR):

⭐ Deep Sulcus Sign: On a supine CXR (e.g., trauma patient), a deep, lucent costophrenic angle is a subtle but specific sign of pneumothorax.
💨 Management - Getting the Air Out
Management strategy is dictated by patient stability and pneumothorax size/type. The goal is to remove pleural air and allow lung re-expansion.
- Observation & Oxygen: For small (<3 cm apex-to-cupola), stable, primary spontaneous pneumothorax (PSP).
- Supplemental O₂ creates a nitrogen pressure gradient, accelerating air resorption by up to 4x.
- Aspiration/Catheter: For large, stable PSP. Less invasive than a large-bore chest tube.
- Chest Tube (Thoracostomy): Definitive treatment for:
- Tension pneumothorax (always place after needle decompression).
- Large or symptomatic PSP failing aspiration.
- Nearly all secondary spontaneous pneumothoraces (SSP) due to poor pulmonary reserve.
- Recurrent pneumothorax.
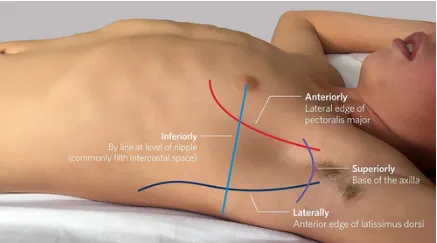
⭐ Placement Pearl: For emergent needle decompression, insert a 14-16 gauge needle superior to the 3rd rib in the 2nd intercostal space (ICS), midclavicular line (MCL). For a chest tube, use the "triangle of safety" (4th/5th ICS, anterior/mid-axillary line).
- Recurrence Prevention: Consider pleurodesis (chemical/mechanical) or VATS for recurrent episodes or persistent air leak >5 days.
📉 Complications - When Things Go South
- Tension Pneumothorax: Hemodynamic collapse, tracheal deviation. ⚠️ Emergent needle decompression → chest tube.
- Re-expansion Pulmonary Edema (RPE): Hypoxemia & cough after rapid inflation of a chronic lung collapse.
- Persistent Air Leak: Air bubbling in chest tube >5-7 days. Consider pleurodesis or VATS.
- Hemopneumothorax: Blood + air. Thoracotomy if output >1.5L initially or >200 mL/hr for 2-4 hrs.
- Subcutaneous Emphysema: Crepitus from air in tissues. Usually self-resolves; monitor airway.
⭐ RPE risk is highest with rapid evacuation of a large (>30%) pneumothorax present for >3 days.
⚡ Biggest Takeaways
- Tension pneumothorax is a clinical diagnosis requiring immediate needle decompression (2nd ICS MCL or 5th ICS AAL), followed by chest tube thoracostomy.
- Small, stable primary spontaneous pneumothorax (PSP) (<3 cm) is managed with observation and supplemental O₂.
- Large or symptomatic PSP requires aspiration or a chest tube.
- Secondary spontaneous pneumothorax (SSP) almost always requires a chest tube and admission.
- Recurrence prevention involves pleurodesis or VATS with blebectomy.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

