⚙️ The Heart's Helpers
Mechanical Circulatory Support (MCS) devices are used for cardiogenic shock or advanced heart failure. They unload the ventricle and improve end-organ perfusion.
- Intra-Aortic Balloon Pump (IABP): Counter-pulsation device. Inflates during diastole to ↑ coronary perfusion; deflates during systole to ↓ afterload.
- Percutaneous VADs (e.g., Impella): Catheter-based axial flow pump placed across the aortic valve. Directly unloads the LV by pumping blood to the aorta.
- Ventricular Assist Device (VAD): Surgically implanted pump. Used as a bridge-to-transplant or as destination therapy.
- VA-ECMO: Provides full cardiopulmonary support, bypassing the heart and lungs.
⭐ Continuous-flow LVADs can cause acquired von Willebrand syndrome due to shear stress on vWF multimers, leading to a high risk of GI bleeding from arteriovenous malformations (AVMs).
💔 Pathophysiology - When the Pump Fails
Cardiogenic shock is profound cardiac pump failure, causing end-organ hypoperfusion despite adequate intravascular volume. The fundamental equation is $CO = HR \times SV$.
- Primary Insult: ↓ Myocardial contractility → ↓ Stroke Volume (SV) & Cardiac Output (CO).
- Maladaptive Compensation:
- Baroreceptor reflex → ↑ Sympathetic tone & ↑ SVR (afterload).
- RAAS activation → ↑ volume (preload).
- Vicious Cycle: ↑ Afterload & ↑ Preload further strain the failing ventricle, increasing myocardial O₂ demand and worsening ischemia.
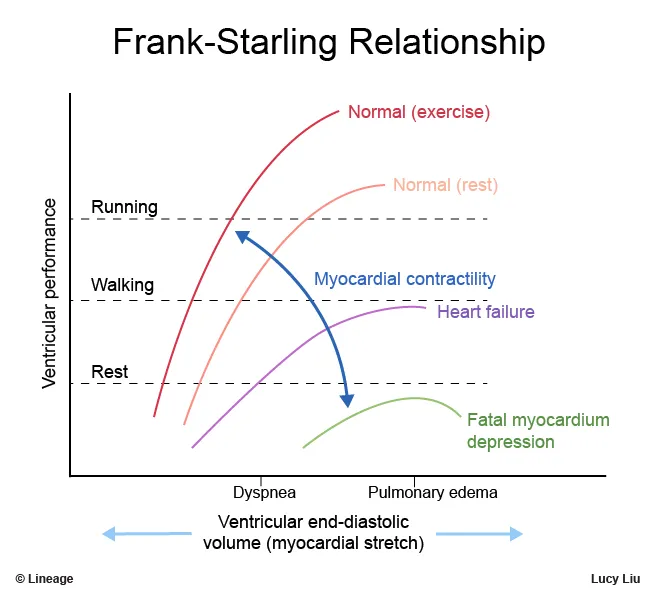
⭐ In cardiogenic shock, the heart operates on the flat/descending part of the Frank-Starling curve; increasing preload (fluids) worsens pulmonary congestion without improving CO.
⚙️ Management: Choosing the Right Device
Selection is multifactorial, guided by:
- Goal of Therapy: Bridge to Recovery (BTR), Transplant (BTT), Candidacy (BTC), or Destination Therapy (DT).
- Required Duration: Short-term (<30 days) vs. Long-term (months-years).
- Hemodynamic Severity: INTERMACS profile (1=crashing, 7=stable).
- Patient Factors: RV function, ambulation potential, end-organ function, anticoagulation tolerance.
⭐ INTERMACS profiles are key. Profile 1 ("Crash and Burn") requires immediate, temporary support (e.g., ECMO). Stable, inotrope-dependent patients (Profile 4, "Resting Symptoms") are prime candidates for durable LVADs as Bridge to Transplant (BTT) or Destination Therapy (DT).
⚠️ Complications - When Good Tech Goes Bad
📌 Mnemonic: BITH-R (Bleeding, Infection, Thrombosis, Hemolysis, Right Heart Failure).
- Bleeding: Most common.
- GI Bleeding: Due to acquired von Willebrand Syndrome (AVWS) from shear stress on vWF multimers & angiodysplasia from non-pulsatile flow.
- Thrombosis:
- Pump Thrombosis: Suspect with ↑ power consumption, hemolysis.
- Stroke/TIA: Embolic events.
- Infection:
- Driveline infection is most frequent; can lead to sepsis.
- Hemolysis: Mechanical RBC destruction.
- Labs: ↑ LDH, ↑ plasma-free Hb, ↓ haptoglobin.
- Right Heart Failure: Common after LVAD placement; RV fails to handle increased preload.
⭐ Continuous-flow LVADs cause loss of pulsatility, leading to arteriovenous malformations (AVMs) in the GI tract, a major cause of recurrent bleeding.
⚡ Biggest Takeaways
- IABP: Inflates in diastole to ↑ coronary perfusion; deflates in systole to ↓ afterload. Contraindicated in aortic regurgitation.
- LVADs: A bridge-to-transplant or destination therapy. High risk of thrombosis, stroke, and GI bleeding (acquired vWD).
- ECMO: V-A for cardiopulmonary support (cardiogenic shock); V-V for isolated respiratory failure (ARDS).
- Impella: Percutaneous pump directly unloads the LV across the aortic valve, reducing myocardial oxygen demand.
- Universal risks: thrombosis, bleeding (anticoagulation-related), infection, and hemolysis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

