🦠 Pathophysiology - Pus in the Pleura
Empyema develops from an initial parapneumonic effusion through three progressive stages. The key is bacterial invasion and subsequent inflammatory response within the pleural space, leading to pus accumulation.
⭐ In the fibrinopurulent stage, pleural fluid analysis is critical: pH < 7.2, Glucose < 60 mg/dL, and LDH > 1000 IU/L strongly suggest empyema and the need for drainage.
🧪 Diagnosis - Finding the Foul Fluid
- Imaging:
- Chest X-ray (CXR): Initial test; shows blunting of costophrenic angles, meniscus sign. Lateral decubitus films confirm free-flowing fluid.
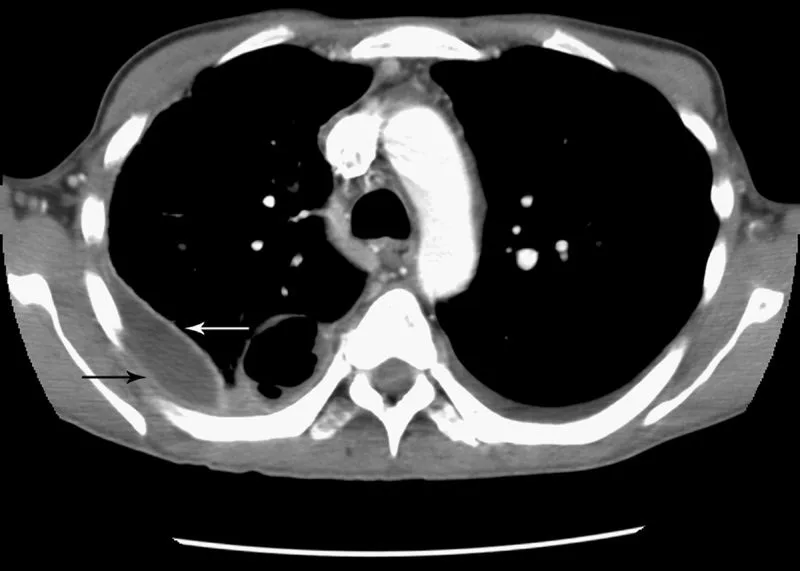
- Chest CT with contrast: Best test to confirm empyema, identify loculations, and guide drainage. May show the "split pleura" sign.
- Thoracentesis (Ultrasound-guided):
- Definitive diagnostic procedure to sample pleural fluid.
- Pleural Fluid Analysis (Complicated Effusion/Empyema):
- Grossly purulent fluid (frank empyema)
- Positive Gram stain or culture
- pH < 7.2
- Glucose < 60 mg/dL
- LDH > 1000 IU/L
⭐ A pleural fluid pH < 7.2 is the single most important indicator for requiring chest tube drainage in a parapneumonic effusion.
💧 Management - Draining the Swamp
Goals: Drain infected fluid, treat infection with broad-spectrum antibiotics (then tailored), and achieve full lung re-expansion. Management follows a stepwise escalation based on clinical response and imaging.
- Fibrinolytics: Intrapleural tPA (tissue plasminogen activator) and DNase (dornase alfa) lyse fibrin loculations and viscous pus, improving chest tube output.
- Surgery (Decortication): Indicated for failed medical therapy or organized empyema causing a "trapped lung."
- VATS is the preferred, less invasive approach with lower morbidity than open thoracotomy.
⭐ The MIST2 trial established that combined intrapleural tPA-DNase therapy improves fluid drainage, reduces hospital stay, and decreases the need for surgery in patients with pleural infection compared to placebo or either agent alone.

🌪️ Complications - When Things Go Wrong
- Fibrothorax: "Trapped lung" from a thick, inelastic pleural peel, restricting lung expansion. May require decortication.
- Bronchopleural Fistula (BPF): Communication between bronchus and pleural space. Presents with persistent air leak.
- Empyema Necessitatis: Infection dissects through the chest wall, forming a subcutaneous abscess.
- Sepsis/Septic Shock: Systemic inflammatory response.
⭐ A bronchopleural fistula (BPF) is a feared complication, often presenting post-pneumonectomy with a new air-fluid level on CXR.
⚡ Biggest Takeaways
- Empyema is pus in the pleural space, most often a complication of pneumonia (parapneumonic effusion).
- Progression follows three stages: Exudative (simple) → Fibrinopurulent (complicated, loculated) → Organizing (fibrous peel).
- Thoracentesis is diagnostic; complicated effusions show pH <7.2, glucose <60 mg/dL, and positive Gram stain/culture.
- Initial management is IV antibiotics and tube thoracostomy (chest tube) for drainage.
- For loculations or failed drainage, escalate to VATS ± fibrinolytics (tPA/DNase).
- Open decortication is reserved for chronic empyema with a trapped lung.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

