🩹 Clinical Manifestations - The Immediate Aftermath
- Hematoma:
- Occurs within 24 hours post-op.
- Presents with pain, swelling, ecchymosis, and ↑ drain output.
- ⚠️ May require urgent surgical evacuation to prevent flap necrosis.
- Seroma:
- Most common complication; collection of serous fluid under skin flaps.
- Typically develops 1-2 weeks post-op.
- Management: observation, aspiration for large/symptomatic collections.
- Infection:
- Presents with erythema, warmth, tenderness, fever.
- Common pathogens: Staphylococcus aureus, Streptococcus pyogenes.
- Skin Flap Necrosis:
- Dusky, violaceous discoloration of the skin edge, may lead to eschar.
- Nerve Injury:
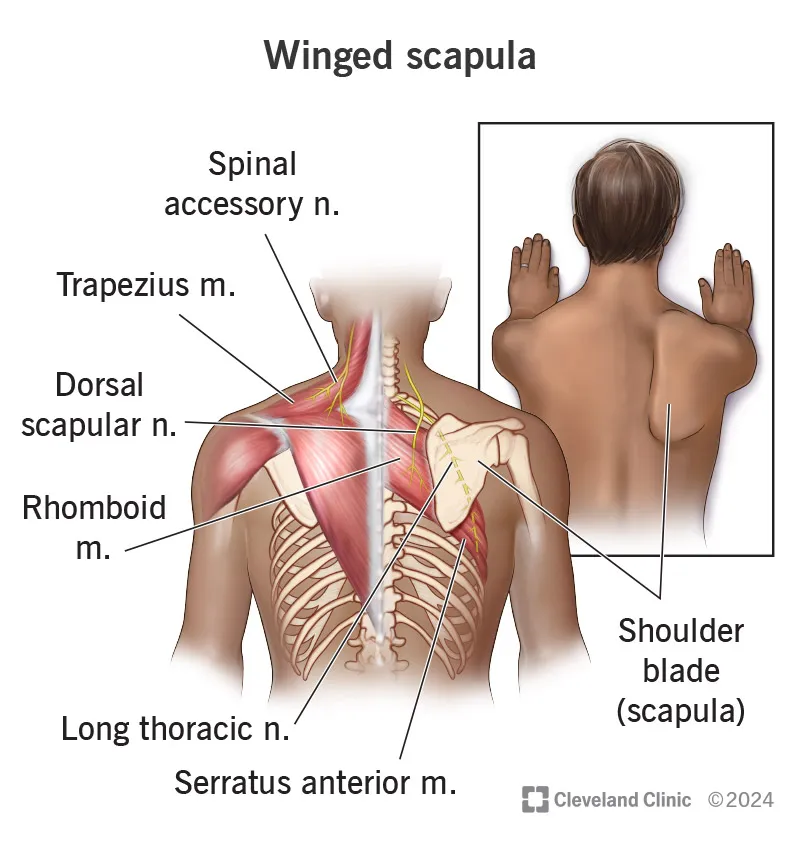
- Long Thoracic n.: "Winged scapula" (Serratus Anterior palsy).
- Thoracodorsal n.: Weak arm adduction/internal rotation (Latissimus Dorsi palsy).
⭐ Injury to the intercostobrachial nerve is the most frequent nerve injury during axillary dissection, causing numbness or paresthesia of the inner upper arm.
⏳ Complications - The Long Haul
-
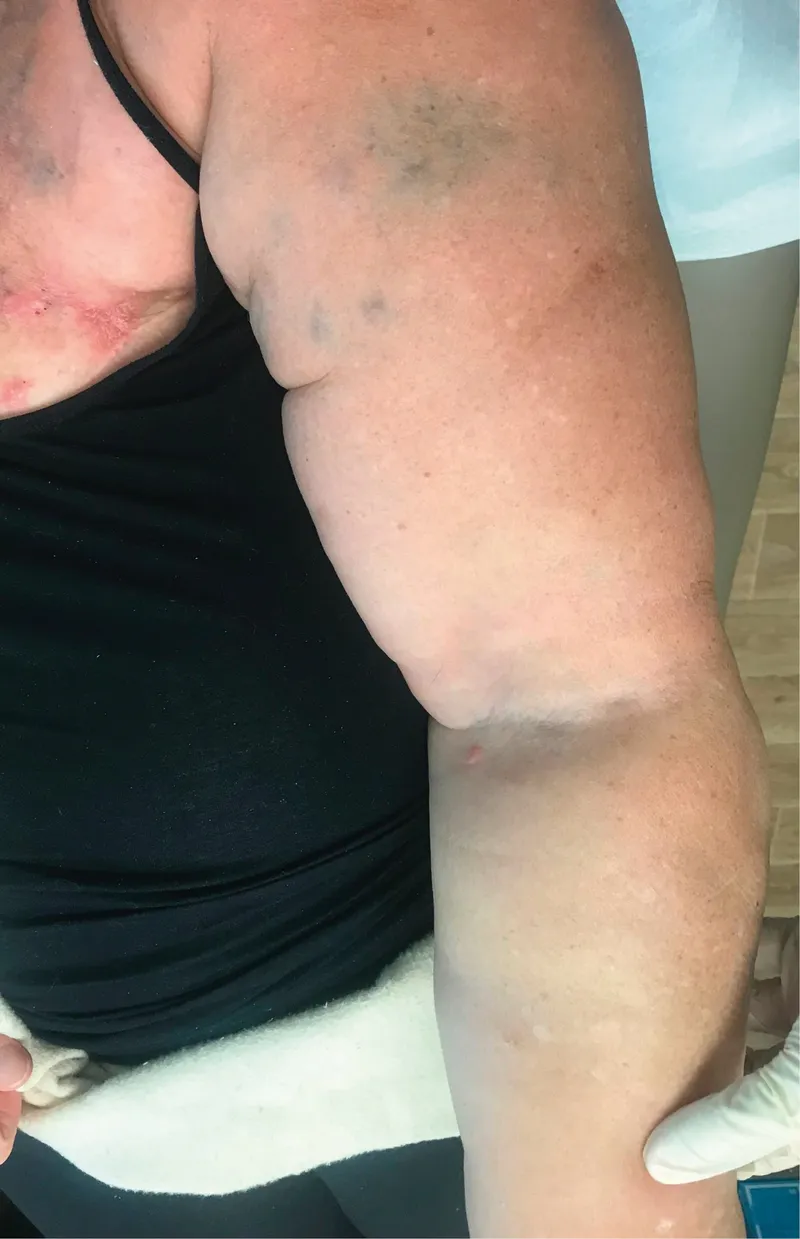
Lymphedema:
- Chronic, progressive swelling of the ipsilateral arm.
- Cause: Disruption of axillary lymphatics, especially after Axillary Lymph Node Dissection (ALND).
- Presentation: Pitting edema, heaviness, ↑ risk of cellulitis/lymphangitis.
- Mgmt: Compression garments, manual lymphatic drainage, physical therapy.
- ⚠️ Avoid BP cuffs, IVs, and phlebotomy on the affected arm.
-
Post-Mastectomy Pain Syndrome (PMPS):
- Chronic neuropathic pain (>3 months) in the axilla, medial arm, or chest wall.
- Cause: Injury to the intercostobrachial nerve during axillary dissection.
-
Shoulder/Arm Dysfunction:
- ↓ Range of motion, weakness, "winged scapula."
- Cause: Injury to long thoracic n. (serratus anterior) or thoracodorsal n. (latissimus dorsi).
⭐ The risk of lymphedema is significantly lower with sentinel lymph node biopsy (SLNB) (
5%) compared to axillary lymph node dissection (ALND) (20-40%).
- Psychosocial: Body image issues, depression, anxiety.
- Phantom Breast Syndrome: Non-painful or painful sensations in the absent breast.
🗺️ Anatomy - Nerve Injury Map
Nerve injury is a key risk during axillary lymph node dissection.
| Nerve | Muscle(s) Innervated | Clinical Deficit & High-Yield Points |
|---|---|---|
| Long Thoracic n. | Serratus Anterior | Winging of the scapula on pushing against a wall. Difficulty with arm abduction > 90°. |
| Thoracodorsal n. | Latissimus Dorsi | Weakness in arm adduction, extension, & internal rotation (e.g., pulling up). Often sacrificed if involved by tumor. |
| Intercostobrachial n. | (Sensory only) | Numbness/paresthesia of medial upper arm & axilla. |
| Medial Pectoral n. | Pectoralis Major & Minor | Weakness in arm adduction & internal rotation; atrophy of pectoral muscles. |
⭐ Most common injury: The intercostobrachial nerve is a sensory nerve most frequently damaged during axillary dissection, leading to posteromedial arm numbness.
🛠️ Management - Tackling Troubles
- Seroma/Hematoma:
- Small: Observe for self-resolution.
- Symptomatic/Large: Sterile needle aspiration.
- Recurrent: Consider drain placement or sclerotherapy.
- Surgical Site Infection (SSI):
- Cellulitis: Antibiotics (cover Staph/Strep).
- Abscess: Incision & Drainage (I&D) + antibiotics.
- Skin Flap Necrosis:
- Limited: Conservative wound care.
- Extensive: Surgical debridement ± grafting.
- Chronic Pain/Neuropathy:
- Gabapentin, pregabalin, TCAs; physical therapy.
⭐ Lymphedema management focuses on control, not cure. Complete Decongestive Therapy (CDT) is the gold standard. ⚠️ Crucially, avoid BP cuffs, IVs, and phlebotomy on the affected arm.
⚡ High-Yield Points - Biggest Takeaways
- Lymphedema: Chronic high-protein swelling from axillary lymph node dissection (ALND). Biggest risk factor for angiosarcoma (Stewart-Treves syndrome).
- Nerve Injury: Long thoracic → winged scapula (serratus anterior). Thoracodorsal → weak arm adduction (latissimus dorsi). Intercostobrachial → upper inner arm numbness.
- Seroma: Most common early complication; a collection of serous fluid under the skin flaps.
- Phantom Breast Syndrome: Sensation in the amputated breast; treat with TCAs or gabapentin.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

