🔬 Indications for Biopsy
- Palpable Mass: Any new, dominant, firm, or persistent solid mass.
- Nipple/Areolar Changes:
- Unilateral, spontaneous, bloody, or serosanguinous discharge.
- Persistent eczema/ulceration (suspect Paget's disease).
- Skin Changes: Peau d'orange, dimpling, retraction, erythema.
- Imaging Findings: Based on Breast Imaging Reporting and Data System (BI-RADS).
⭐ A new palpable mass in a woman >30 years old, or any solid mass in a postmenopausal woman, requires tissue diagnosis, regardless of mammogram findings.
🔬 Radiology - The Biopsy Toolkit
The goal is histopathologic diagnosis of suspicious breast lesions. The choice of technique depends on the lesion type and imaging visibility.
-
Fine-Needle Aspiration (FNA):
- Uses a small (22-27 gauge) needle for cytology (cells).
- Main use: Draining simple cysts, sampling axillary nodes.
- ⚠️ Cannot distinguish invasive from in-situ disease.
-
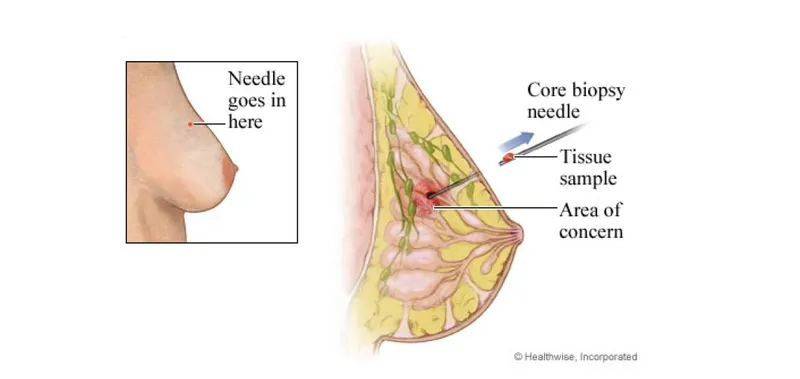
Core Needle Biopsy (CNB):
- Gold standard for initial diagnosis.
- Uses a larger (14-gauge) needle for histology (tissue architecture).
- Vacuum-assisted biopsy (VAB) is a type of CNB that obtains larger, contiguous samples, ideal for calcifications.
-
Surgical (Excisional) Biopsy:
- Removes the entire lesion.
- Used when percutaneous biopsy is discordant, non-diagnostic, or for specific high-risk lesions.
⭐ Always correlate biopsy results with imaging findings. A "benign" pathology report for a highly suspicious (BI-RADS 5) lesion is considered discordant and requires surgical excision.
🔬 Management - Choosing the Right Tool
- Fine Needle Aspiration (FNA):
- Best for simple cysts (diagnostic & therapeutic).
- Provides cytology only; cannot distinguish DCIS from invasive cancer.
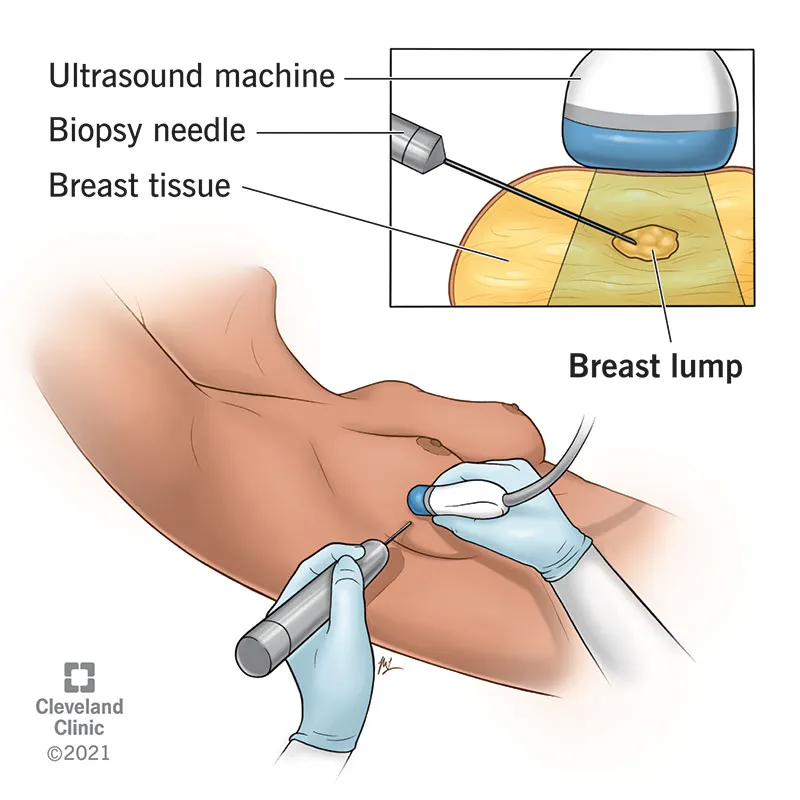
- Core Needle Biopsy (CNB):
- Initial standard for solid masses & suspicious calcifications.
- Provides histology (tissue architecture).
- Guided by US (masses), stereotaxis (calcifications), or MRI.
- Surgical (Excisional) Biopsy:
- Used when CNB is inconclusive, discordant with imaging, or for high-risk lesions (e.g., ADH) due to upgrade risk.
⭐ Core needle biopsy (CNB) is preferred over Fine Needle Aspiration (FNA) for solid masses because it provides tissue architecture, allowing differentiation between in-situ and invasive carcinoma.
🩹 Complications - Post-Poke Problems
- Hematoma/Bleeding: Most common; manage with direct pressure.
- Infection (Cellulitis): Rare; presents with erythema, warmth, pain.
- Pain & Bruising: Expected, self-limited.
- Pneumothorax: ⚠️ Very rare; risk with deep lesions near the chest wall.
- Vasovagal Syncope: Fainting during the procedure.
- False Negative: Risk varies by technique (↑FNA, ↓Excisional).
⭐ Post-biopsy hematomas can obscure or mimic malignancy on follow-up mammograms, complicating interpretation.
⚡ Biggest Takeaways
- Fine Needle Aspiration (FNA) provides cytology only; it cannot differentiate in-situ from invasive disease.
- Core Needle Biopsy (CNB) is the initial standard of care for most breast lesions, providing crucial histology.
- Use ultrasound-guided CNB for suspicious masses and stereotactic CNB for non-palpable microcalcifications.
- Excisional biopsy removes the entire lesion; indicated for discordant CNB results or certain high-risk lesions.
- Sentinel Lymph Node Biopsy (SLNB) is a staging procedure for invasive cancer, not a primary diagnostic biopsy.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

