Secondary Survey - The Grand Tour
-
A systematic head-to-toe evaluation to identify all injuries after the primary survey and resuscitation are complete. It is performed on a stable patient.
-
History (📌 AMPLE):
- Allergies
- Medications (especially anticoagulants, beta-blockers)
- Past medical history / Pregnancy
- Last meal (for anesthesia/surgery timing)
- Events / Environment related to injury
-
Comprehensive Physical Exam:
- Head & Maxillofacial: Check for lacerations, fractures (palpate), and eye/ear/nose/throat injuries.
- Cervical Spine & Neck: Maintain protection; inspect for trauma, hematomas, and tracheal deviation.
- Chest: Palpate for tenderness, crepitus; auscultate heart and lung sounds.
- Abdomen & Pelvis: Inspect, auscultate, palpate. Pelvic stability assessment if no fracture suspected.
- Perineum/Rectal/Vaginal: Assess for bleeding, hematomas, and sphincter tone.
- Musculoskeletal: Examine extremities for fractures, deformities, and compartment syndrome.
- Neurological: Re-evaluate GCS, pupillary response, and check for focal deficits.
⭐ Continuous Re-evaluation: The secondary survey is a dynamic process. Patients must be frequently reassessed to identify missed injuries or deterioration, especially after any intervention.
Head-to-Toe Exam - A Systematic Sweep
- Head & Maxillofacial:
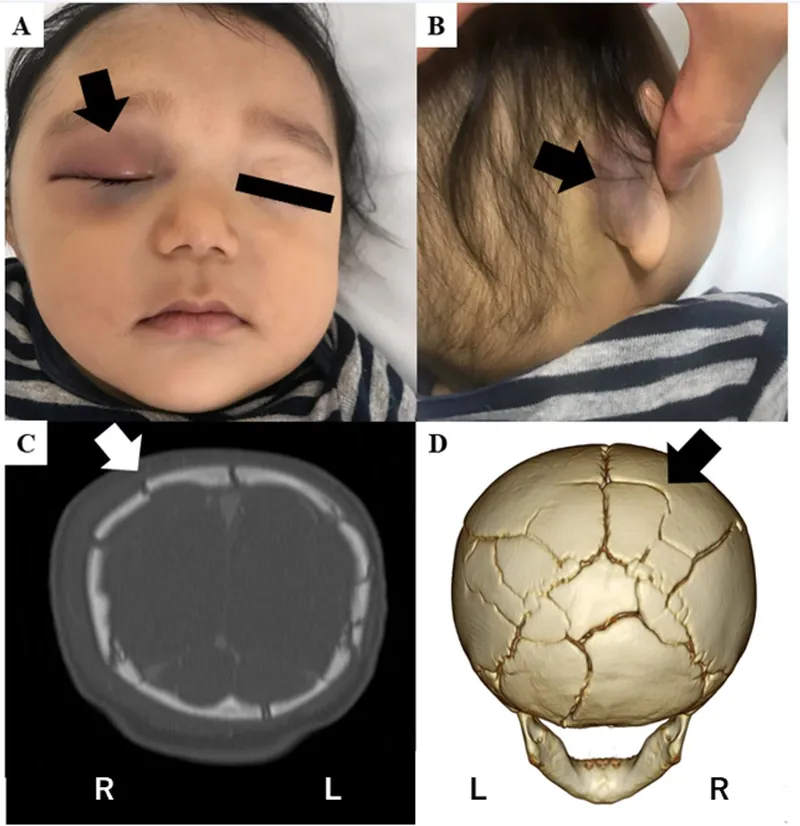
- Inspect & palpate for lacerations, deformities, step-offs (e.g., basilar skull fracture signs: Raccoon eyes, Battle's sign).
- Eyes: PERRLA, EOMI, fundoscopy for hemianopia, papilledema.
- Maxillofacial: Palpate for instability (Le Fort fractures), check for malocclusion.
- Cervical Spine & Neck:
- Maintain C-spine immobilization until cleared.
- Palpate for tenderness, check for JVD, tracheal deviation, subcutaneous emphysema.
- Chest:
- Inspect, Auscultate, Palpate, Percuss (IAPP).
- Identify flail chest, open wounds, crepitus.
- Auscultate heart and lung sounds.
- Abdomen & Pelvis:
- IAPP: Note tenderness, guarding, ecchymosis (Grey Turner's, Cullen's sign).
- Pelvis: Assess stability with gentle pressure. Do not rock the pelvis if fracture is suspected.
- Perineum & Rectal:
- Check for blood at the urethral meatus, scrotal/vulvar hematoma.
- Rectal exam for tone, wall integrity, and prostate position.
⭐ A high-riding prostate on DRE suggests significant pelvic trauma and potential urethral injury. A retrograde urethrogram is indicated before catheterization.
- Musculoskeletal & Back:
- Inspect all extremities for deformity, swelling, open fractures.
- Palpate for tenderness and crepitus. Check distal pulses, motor, and sensation (PMS).
- Log-roll patient to examine the entire spine and back.
Adjuncts & Re-evaluation - Diagnostic Deep Dive
-
Diagnostic Adjuncts: Specialized tests to identify specific injuries.
- FAST (Focused Assessment with Sonography for Trauma): Screens for hemoperitoneum, pericardial effusion.
- eFAST: Adds bilateral thoracic views for pneumothorax.
- DPL (Diagnostic Peritoneal Lavage): Invasive; used if ultrasound is unavailable/equivocal in unstable patients.
- X-rays: Chest (AP), Pelvis (AP), C-spine (lateral).
- CT Scans: For stable patients to detail head, chest, abdominal, and spinal injuries.
-
Monitoring & Tubes:
- Urinary Catheter: Monitors output (goal: >0.5 mL/kg/hr in adults).
- Gastric Tube: Decompresses stomach, reduces aspiration risk.
-
Continuous Re-evaluation:
- Vital signs, GCS, and urine output are monitored serially.
- New findings prompt re-assessment, potentially repeating the primary survey.
⭐ DPL is considered positive in blunt trauma if >10 mL of gross blood is aspirated initially, or RBC count is >100,000/mm³ in the lavage fluid.

High‑Yield Points - ⚡ Biggest Takeaways
- The Secondary Survey is a comprehensive head-to-toe evaluation performed only after the primary survey is complete and the patient is hemodynamically stable.
- It includes a complete history using the AMPLE mnemonic: Allergies, Medications, Past medical history, Last meal, and Events of injury.
- A thorough physical examination is performed, including a complete neurological exam, and examination of all orifices.
- Continuous re-evaluation of vital signs is crucial to detect deterioration.
- Maintain a high index of suspicion for occult injuries.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

