🌬️ The Pre-Op Puff Check
- Smoking: Major risk for Postoperative Pulmonary Complications (PPCs). Advise cessation ≥4-8 weeks pre-op to ↓ risk.
- COPD/Asthma: Assess severity (e.g., FEV1/FVC < 0.7). Optimize with pre-op bronchodilators and/or steroids.
- Obstructive Sleep Apnea (OSA): Screen with 📌 STOP-BANG questionnaire. High risk for post-op hypoxemia and respiratory failure.
- Recent URI: Postpone elective surgery for 4-6 weeks to ↓ risk of laryngospasm/bronchospasm.
⭐ Smoking cessation >8 weeks pre-op significantly ↓ PPCs. Cessation <4 weeks may paradoxically ↑ airway reactivity and sputum.

🫁 Pathophysiology - Lungs Under Lockdown
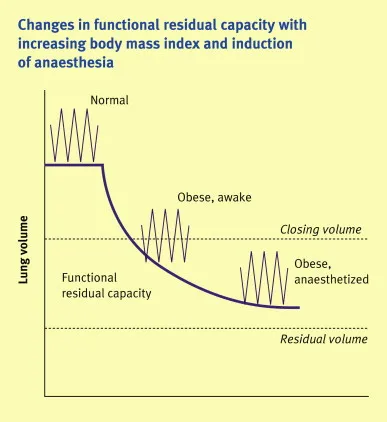
- ↓ Functional Residual Capacity (FRC): The central event under general anesthesia (GA).
- Supine position & neuromuscular blockade cause cephalad diaphragm shift.
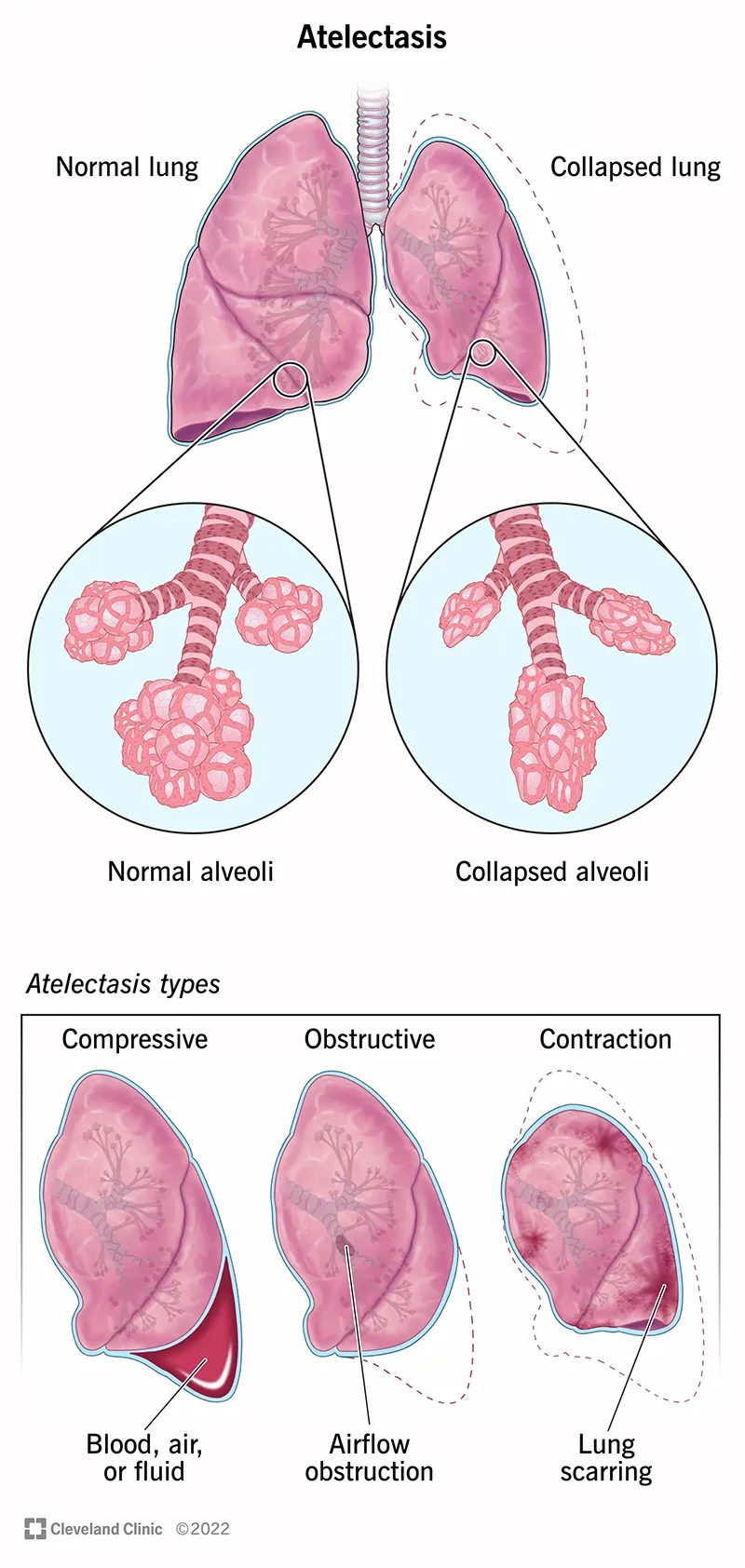
- Results in compression atelectasis, primarily in dependent lung zones.
- ↑ V/Q Mismatch:
- Atelectasis creates an intrapulmonary shunt ($V/Q \approx 0$), causing hypoxemia.
- Volatile anesthetics impair Hypoxic Pulmonary Vasoconstriction (HPV), worsening the shunt.
- ↓ Respiratory Control & Clearance:
- Opioids & anesthetics blunt central chemoreceptor response to ↑ $CO_2$ and ↓ $O_2$.
- ↓ Mucociliary clearance promotes secretion retention.
⭐ FRC can decrease by 15-20% within minutes of anesthesia induction, moving tidal breathing below closing capacity and predisposing to rapid desaturation.
🌬️ Management - Keeping Airways Awesome
-
Pre-operative Strategy:
- Risk Assessment: Use STOP-BANG for OSA; note smoking history.
- Optimization: Mandate smoking cessation >4-8 weeks pre-op. Treat active infections. Optimize asthma/COPD with bronchodilators.
-
Intra-operative Tactics:
- Lung Protective Ventilation: Use low tidal volumes ($V_T$ = 6-8 mL/kg ideal body weight), apply PEEP (5-10 cmH₂O), and perform recruitment maneuvers.
- Avoid high FiO₂ to prevent absorption atelectasis.
-
Post-operative Care:
- 📌 I COUGH: Incentive spirometry, Cough/deep breathing, Oral care, Understanding (patient education), Get moving (early mobilization), Head of bed elevation.
- Prioritize regional analgesia over systemic opioids to facilitate effective breathing.
⭐ Postoperative pulmonary complications (PPCs), especially atelectasis, peak within the first 24-48 hours. They are a leading cause of morbidity after major non-cardiac surgery.
🌬️ Complications - When Breaths Go Bad
- Atelectasis (POD 1-2): Most common. Small airway collapse from ↓ lung volumes.
- Presents with fever, tachypnea, ↓ breath sounds at bases.
- Prevention/Tx: Incentive spirometry, deep breathing, early mobilization.
- Aspiration: Gastric contents enter lungs.
- Pneumonitis: Immediate chemical injury.
- Pneumonia: Bacterial infection, develops over days.
- Pneumonia (POD 3-5): Nosocomial infection (e.g., Pseudomonas, S. aureus).
- Presents with fever, productive cough, consolidation on CXR.
- Pulmonary Embolism (PE): Sudden onset dyspnea, pleuritic chest pain, tachycardia.
- ARDS: Diffuse alveolar damage from sepsis, trauma. Hypoxemia refractory to O₂, bilateral infiltrates ("white-out").
- Laryngospasm/Bronchospasm: Airway hyperreactivity causing stridor or wheezing, often post-extubation.
⭐ Atelectasis is the most common cause of fever in the first 48 hours post-op. Often resolves with incentive spirometry and mobilization.
⚡ Biggest Takeaways
- Smoking cessation >4-8 weeks pre-op is crucial to ↓ postoperative pulmonary complications.
- General anesthesia consistently decreases functional residual capacity (FRC), leading to basilar atelectasis.
- Atelectasis is the most common cause of fever in the first 48 hours post-op; prevent with incentive spirometry.
- Aspiration pneumonitis risk is managed with strict NPO guidelines; high risk in obesity and emergency cases.
- Pulmonary embolism (PE) is a major preventable cause of postoperative mortality; prophylaxis is key.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

