❤️ Cardiac Risk Stratification
-
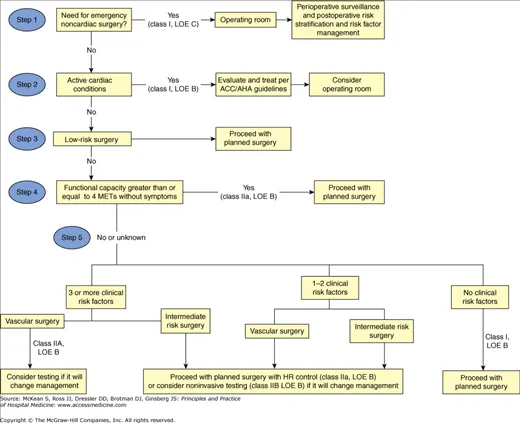
Goal: Predict & mitigate Major Adverse Cardiac Events (MACE) using ACC/AHA guidelines. Integrates surgical risk, patient comorbidities via the Revised Cardiac Risk Index (RCRI), and functional capacity via Metabolic Equivalents (METs).
-
RCRI Components (1 point each):
- High-risk surgery (vascular, intraperitoneal, intrathoracic)
- Ischemic Heart Disease (hx of MI, +stress test)
- Congestive Heart Failure (hx of CHF, pulmonary edema)
- Cerebrovascular Disease (hx of CVA/TIA)
- Insulin-dependent Diabetes
- Creatinine >2.0 mg/dL
- MACE Risk: 0 pts ≈0.4%; 1 pt ≈1%; ≥2 pts ≈>2%.
-
Functional Capacity (METs):
- <4 METs: Poor (can't climb 1 flight of stairs).
- ≥4 METs: Good (can proceed if RCRI is low).
⭐ In patients with good functional capacity (≥4 METs), further cardiac testing is rarely needed, regardless of RCRI score, for most elective surgeries.
💊 Management - Perioperative Drug Patrol
- Beta-blockers: CONTINUE throughout the perioperative period.
- ⚠️ Abrupt withdrawal risks rebound tachycardia, hypertension, and ischemia.
- Statins: CONTINUE indefinitely.
- Pleiotropic effects (plaque stabilization, anti-inflammatory) reduce MACE risk.
- ACE Inhibitors / ARBs: HOLD on the morning of surgery.
- Prevents refractory hypotension during anesthesia induction.
- Restart post-op once hemodynamically stable and euvolemic.
- Antiplatelets (Aspirin/DAPT):
- Aspirin (secondary prevention): CONTINUE unless bleeding risk is very high (e.g., intracranial, spinal surgery).
- P2Y12 Inhibitors (e.g., clopidogrel): Stop 5-7 days before surgery.
⭐ For coronary stents, DAPT discontinuation is high-risk. Delay elective surgery: >1 month post-BMS (Bare Metal Stent), >6 months post-DES (Drug-Eluting Stent).
💔 Complications - The Post-Op Heart Attack
- Perioperative MI: Myocardial infarction occurring during or within 30 days of surgery.
- MINS (Myocardial Injury after Noncardiac Surgery): Prognostically significant myocardial injury due to ischemia, detected by an elevated troponin. Often asymptomatic.
- Two Main Types:
- Type 1 MI: Atherosclerotic plaque rupture & thrombosis. Classic ACS mechanism.
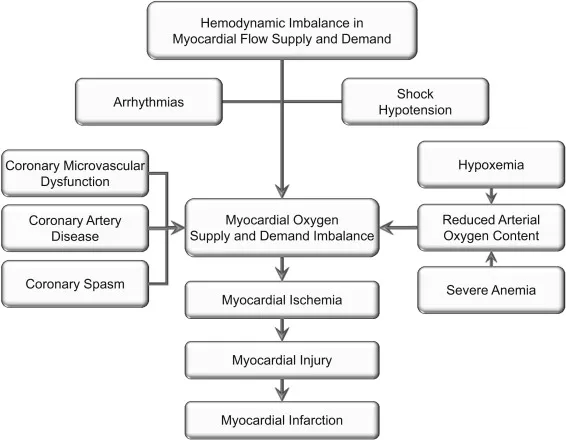
- Type 2 MI: Oxygen supply-demand mismatch. The predominant type post-op.
- ↓ Supply: Hypotension, anemia, hypoxemia.
- ↑ Demand: Tachycardia, hypertension, pain, stress.
- Diagnosis & Surveillance:
- Routine troponin surveillance in high-risk patients (pre-op and post-op days 1-3).
- ECG may show new ischemic changes but is often non-specific or normal.
⭐ Most perioperative MIs are Type 2 and clinically silent (no chest pain). This underscores the importance of routine troponin surveillance in at-risk patients, as MINS is independently associated with increased mortality.
⚡ Biggest Takeaways
- Use the RCRI to stratify risk for major adverse cardiac events (MACE).
- Continue chronic beta-blockers and statins; do not start beta-blockers on surgery day.
- Highest risk for post-op MI is within 48-72 hours, often silent or atypical.
- For coronary stents, consult cardiology on DAPT management to prevent stent thrombosis.
- Severe symptomatic aortic stenosis is a major contraindication for elective non-cardiac surgery.
- Manage new post-op A-fib with rate control first (e.g., metoprolol, diltiazem).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

