Etiology & Pathophysiology - Getting All Tied Up
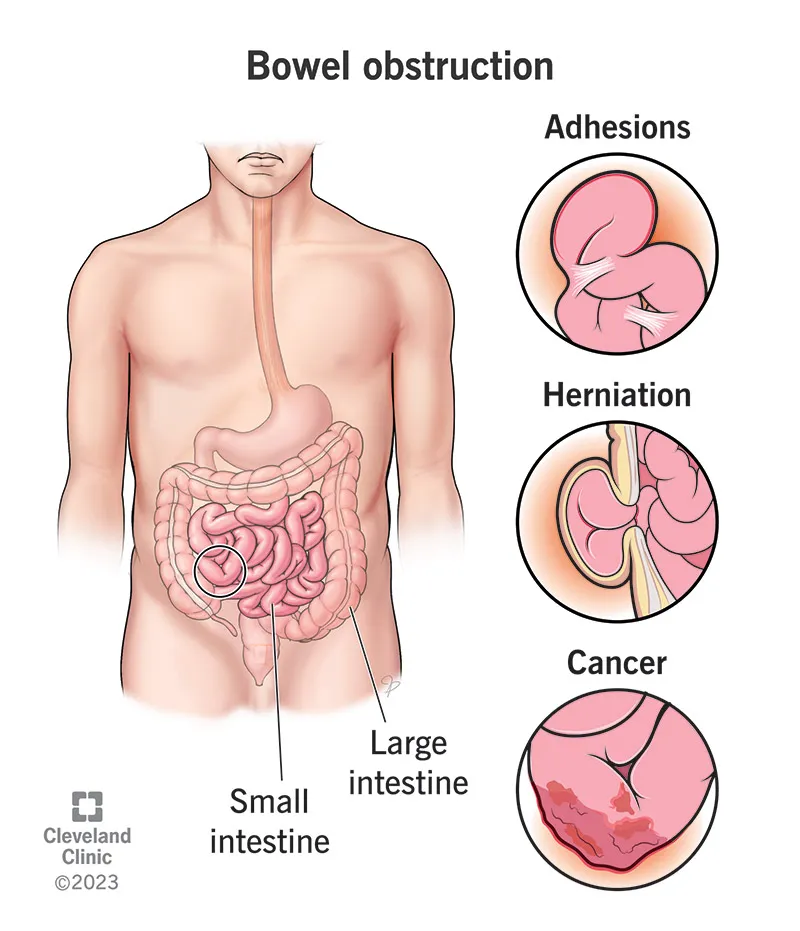
- Most Common Causes (📌 ABC):
- Adhesions (post-operative, ~75%)
- Bulge (incarcerated hernias)
- Cancer (tumors, intrinsic or extrinsic)
- Pathophysiology Cascade:
- Obstruction → Proximal bowel dilation (gas/fluid) → ↑ Intraluminal pressure.
- Bowel wall edema & third-spacing → Hypovolemia & electrolyte shifts.
- Venous & arterial compromise → Ischemia, necrosis, perforation.
⭐ Strangulation is a surgical emergency, marked by fever, tachycardia, leukocytosis, and localized pain. It implies compromised blood flow requiring immediate intervention to prevent bowel necrosis.
Clinical Presentation - The Gut's Cry for Help
- Cardinal Symptoms (📌 CAVO):
- Colicky abdominal pain: Initially periumbilical & crampy; becomes constant & severe with strangulation.
- Abdominal distension: More pronounced in distal SBO.
- Vomiting: Early, bilious (proximal SBO) vs. late, feculent (distal SBO).
- Obstipation: Failure to pass stool or flatus; a late finding indicating complete obstruction.
- Physical Exam Findings:
- Bowel sounds: Early high-pitched "tinkles" → Late hypoactive/absent sounds.
- ⚠️ Peritoneal signs (e.g., rebound tenderness, guarding) suggest strangulation or perforation.
⭐ A patient with partial SBO may still pass flatus or have diarrhea.
Diagnosis - Peeking Inside the Pipes
- Labs: CBC, BMP, lactate, and type & screen. Look for leukocytosis, electrolyte abnormalities, and signs of ischemia (↑ lactate).
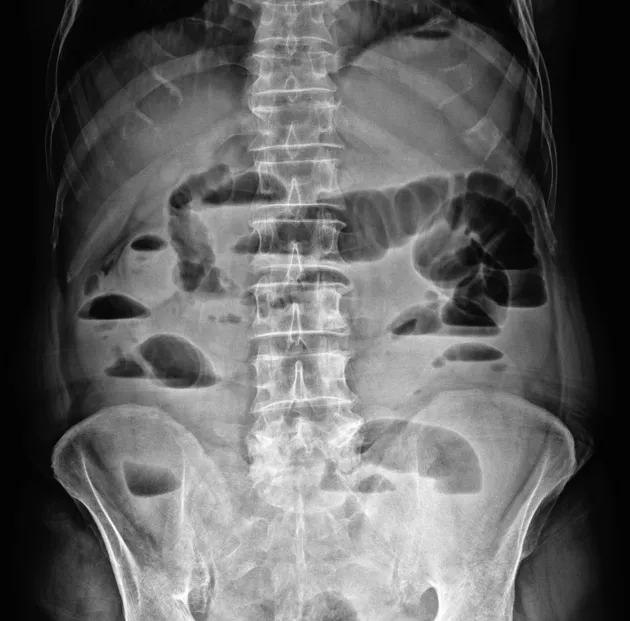
- Abdominal X-ray (AXR): Initial imaging.
- Dilated small bowel loops (>3 cm).
- Multiple air-fluid levels on upright film.
- Paucity of gas in the colon.
- CT Scan (Abdomen/Pelvis with IV contrast): Gold standard for diagnosis.
- Confirms diagnosis, identifies location, severity, and etiology (e.g., hernia, mass).
- Determines presence of complications (ischemia, perforation).
⭐ Exam Favorite: The most important finding on CT is the transition point-a discrete location where the bowel caliber changes from dilated proximal loops to collapsed distal loops, pinpointing the obstruction site.
Management - Untangling the Knot
-
Initial Stabilization (Conservative): The cornerstone for all SBO patients.
- NPO (Nil Per Os): Bowel rest is critical.
- IV Fluids: Aggressive resuscitation with isotonic crystalloids (Lactated Ringer's or Normal Saline) to correct dehydration.
- Nasogastric (NG) Tube: Decompresses the stomach and proximal bowel, reducing distention and vomiting.
- Monitor urine output (goal > 0.5 mL/kg/hr) and electrolytes.
-
Definitive Management: The decision to operate hinges on the presence of complications.
⭐ In a "virgin" abdomen (no prior surgery), a hernia is the most likely cause of SBO. Always perform a thorough physical exam to check for incarcerated hernias, as this is a surgical emergency.
High‑Yield Points - ⚡ Biggest Takeaways
- Adhesions from prior surgery are the #1 cause of SBO.
- Cardinal features are colicky abdominal pain, vomiting, abdominal distension, and obstipation.
- Exam reveals high-pitched, tinkling bowel sounds early on, which later become hypoactive.
- Abdominal X-ray shows dilated small bowel loops (>'''3 cm''') with air-fluid levels.
- CT scan is the diagnostic standard, confirming the diagnosis and identifying the transition point.
- Initial management is conservative: NPO, IV fluids, and NG tube decompression.
- Peritoneal signs, acidosis, or failure to resolve indicate strangulation and require urgent surgery.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

