Initial Assessment - Stabilize to Scrutinize
- Primary Survey (ABCDEs): Airway, Breathing, Circulation, Disability, Exposure. A systematic approach to identify and treat life-threatening conditions immediately.
- Resuscitation: Secure 2 large-bore IV lines, initiate crystalloid fluid bolus (e.g., Lactated Ringer's), draw baseline labs (CBC, CMP, lactate, coags, type & screen).
- Secondary Survey: A detailed head-to-toe examination and focused history (AMPLE: Allergies, Medications, Past medical history, Last meal, Events).
⭐ Serial abdominal exams and lactate measurements are crucial. A rising lactate is a red flag for underlying ischemia or sepsis, even with otherwise stable vital signs.
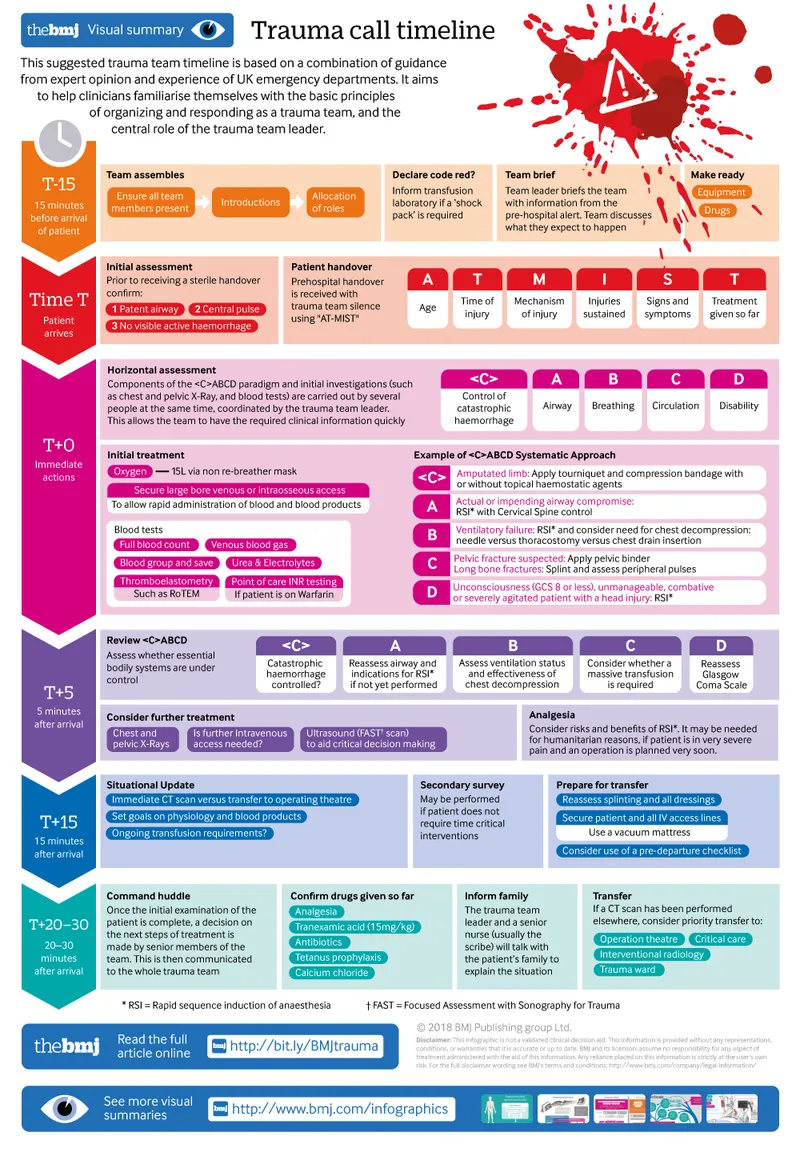
Patient Selection for NOM - Who Skips the Knife?
The decision hinges on two pillars: patient stability and injury characteristics. NOM is reserved for the hemodynamically stable patient without signs of peritonitis (e.g., guarding, rebound tenderness).
- Key Criteria:
- Hemodynamic stability (SBP >90 mmHg, HR <100 bpm)
- No signs of peritonitis
- Reliable clinical examination (GCS 15)
⭐ For select cases of acute diverticulitis (e.g., Hinchey Ia/Ib), NOM with antibiotics is the standard of care, avoiding surgery in over 85% of patients.
Core NOM Strategies - Guts on Rest
- Nil Per Os (NPO): Crucial first step to minimize gut stimulation and inflammation.
- Intravenous Fluids (IVF): Isotonic crystalloids (e.g., Lactated Ringer's) to maintain hemodynamic stability and correct electrolyte imbalances.
- Gastric Decompression: Nasogastric (NG) tube placement for patients with nausea, vomiting, or significant abdominal distention.
- Serial Clinical Assessment: The cornerstone of NOM. Frequent re-evaluation (q4-6h) of:
- Vitals (tachycardia, fever)
- Abdominal exam (tenderness, guarding, peritonitis)
- Urine output (> 0.5 mL/kg/hr)
- Judicious Analgesia: Pain control that doesn't mask peritoneal signs.
⭐ High-Yield: Clinical improvement (↓ pain, ↓ WBC) dictates when to advance the diet, not just the return of bowel sounds or flatus. Early re-feeding may be beneficial in select stable patients.
Monitoring & Failure - Watchful Waiting Woes
- Core Principle: Non-operative management (NOM) is a trial requiring continuous, active monitoring, not passive observation.
- Key Parameters:
- Clinical: Serial abdominal exams (watch for peritonitis), vital signs (SIRS criteria).
- Labs: Rising lactate or WBC count are red flags.
- Imaging: Repeat CT scan if the clinical picture worsens or fails to improve.
⭐ The development of peritonitis or hemodynamic instability despite resuscitation are hard stops for NOM and mandate immediate surgical exploration.
Specific Conditions - No-Scalpel Scenarios
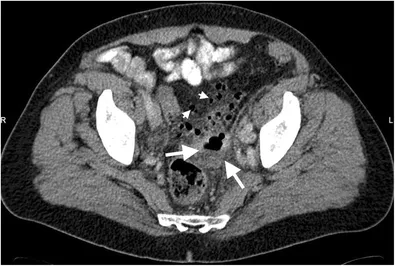
- Acute Diverticulitis:
- Uncomplicated (Hinchey I): Bowel rest, IV antibiotics.
- Abscess (Hinchey II): Percutaneous drainage if >4-5 cm; otherwise, treat with IV antibiotics alone.
- Adhesive Small Bowel Obstruction (SBO):
- Stable/Partial: NPO, NG tube decompression, IV fluids.
- ⚠️ Watch for ischemia (fever, tachycardia, acidosis) → immediate surgery.
⭐ In partial SBO, water-soluble contrast challenge (e.g., Gastrografin) can be both diagnostic and therapeutic, predicting the need for surgery.
High‑Yield Points - ⚡ Biggest Takeaways
- Hemodynamic stability is the primary prerequisite for non-operative management; instability mandates surgery.
- Core principles include bowel rest (NPO), IV fluid resuscitation, and nasogastric (NG) tube decompression.
- Serial abdominal exams and labs are crucial to monitor for clinical deterioration or peritonitis.
- Broad-spectrum antibiotics are key for infectious etiologies like uncomplicated diverticulitis or contained abscesses.
- Failure to improve within 24-48 hours is a strong indication for surgical intervention.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

