Pathophysiology - Gut Under Attack
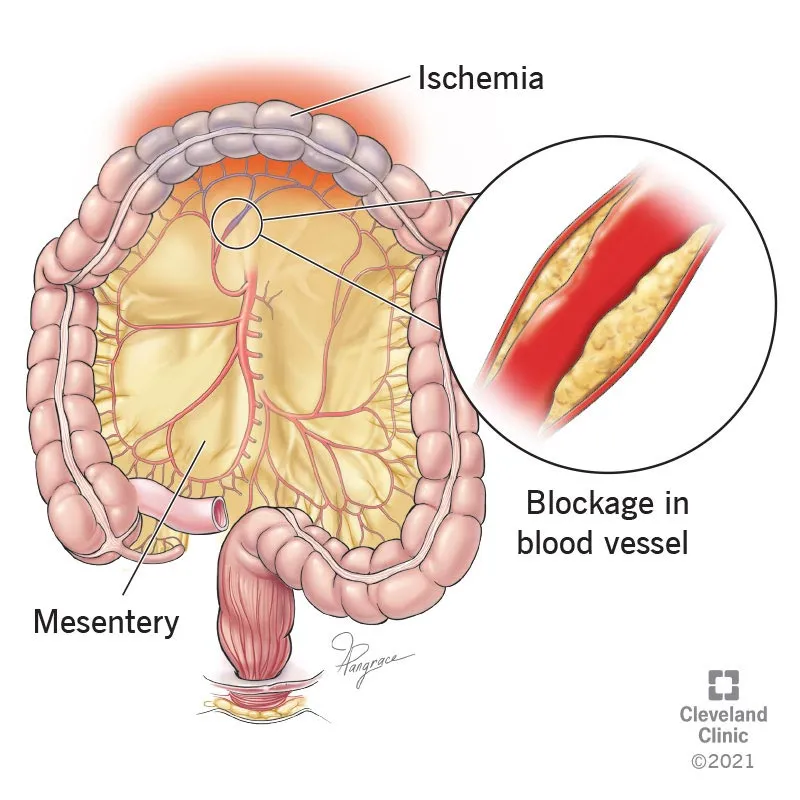
- Primary Insult: Acute reduction in gut blood flow, creating an oxygen supply/demand mismatch.
- Cellular Cascade: Ischemia forces anaerobic metabolism (↑ lactic acidosis). The mucosal barrier, highly sensitive to hypoxia, breaks down within 3 hours, permitting bacterial translocation.
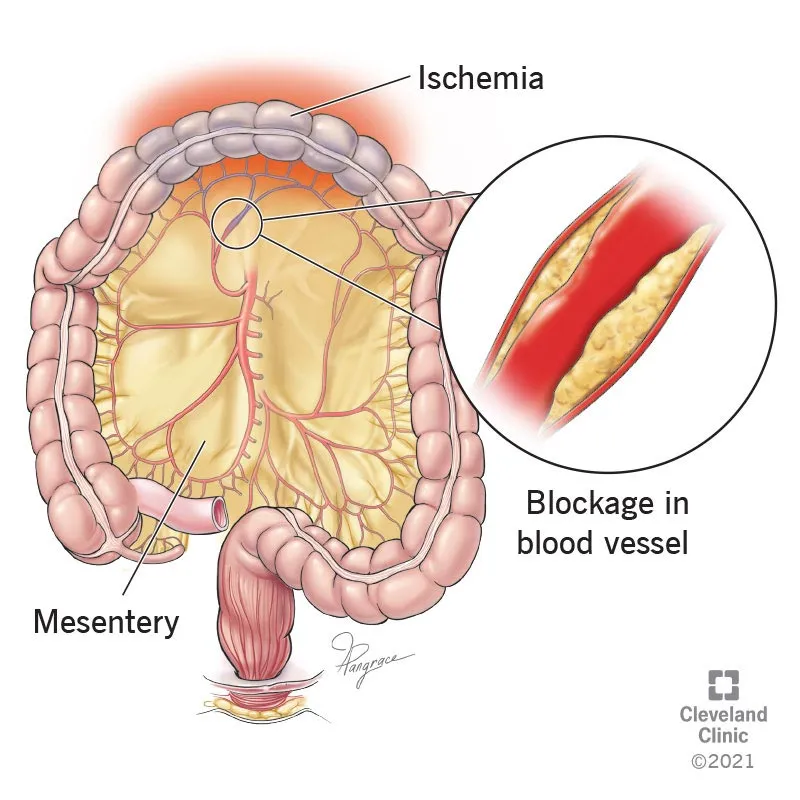
⭐ Pain out of proportion to physical exam is the hallmark sign, stemming from visceral ischemia before transmural infarction causes peritoneal signs.
Etiology & Types - The Four Horsemen
- Acute Arterial Occlusive Disease (~75%): The most common cause.
- Embolism (~50%): Sudden onset. Typically from atrial fibrillation, lodging in the Superior Mesenteric Artery (SMA).
- Thrombosis (~25%): Gradual onset. Due to severe atherosclerosis at the SMA origin.
- Non-Occlusive Mesenteric Ischemia (NOMI) (~20%): Splanchnic vasoconstriction from low-flow states (e.g., shock, heart failure, high-dose vasopressors).
- Mesenteric Venous Thrombosis (MVT) (<10%): Clot in mesenteric veins, linked to hypercoagulable states.
⭐ The SMA is the most commonly affected vessel in acute mesenteric ischemia, particularly from an embolic source.
Clinical Features - Pain Out of Proportion
- Hallmark: Acute, severe, diffuse abdominal pain with a strikingly benign physical exam.
- Pain is often sudden, periumbilical, and poorly localized.
- Early stages lack peritoneal signs like guarding or rebound tenderness.
- Associated features: nausea, vomiting, and initial forceful bowel evacuation.
- 📌 Pain out of proportion, AFIB/atherosclerosis, Increased lactate, No peritonitis (early) -> PAIN.
⭐ Late findings (>12 hrs) indicate bowel infarction: peritoneal signs, hematochezia, and shock. Survival rates drop dramatically once peritonitis develops.
Diagnosis - Racing the Clock
- Labs: ↑ Lactate (a late, ominous sign), leukocytosis, metabolic acidosis.
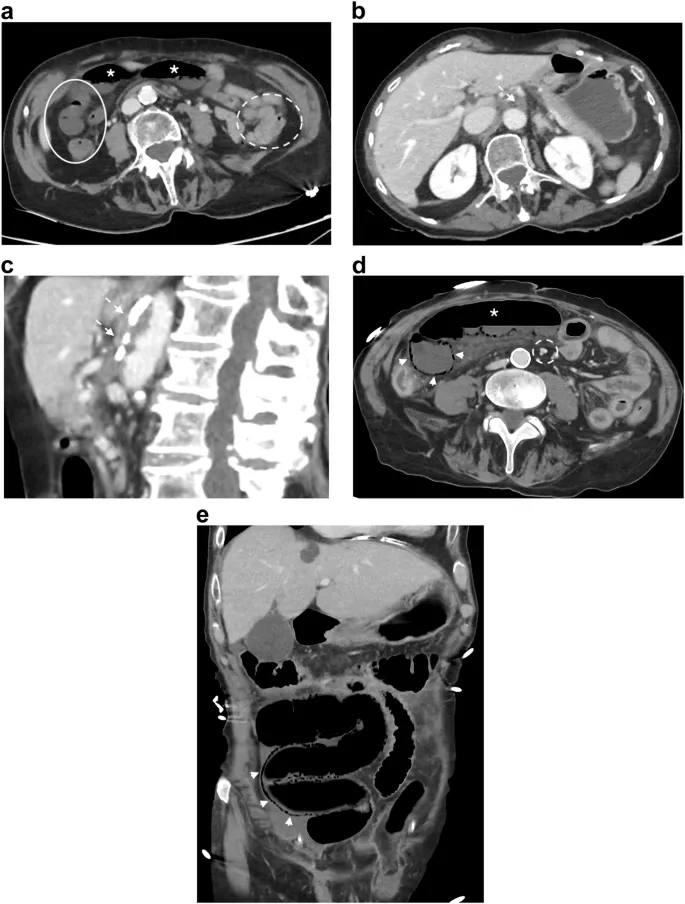
- Imaging Gold Standard: CT Angiography (CTA) of the abdomen and pelvis is the primary diagnostic tool.
- Identifies vessel occlusion (embolus/thrombus), bowel wall thickening, pneumatosis intestinalis (air in bowel wall), and portal venous gas.
- Conventional Angiography: Invasive, but allows for simultaneous diagnosis and therapeutic intervention (e.g., vasodilator infusion for NOMI).
⭐ The classic presentation is "pain out of proportion to the physical exam." High suspicion is critical in patients with risk factors like atrial fibrillation or peripheral vascular disease.
Management - Code Gut
- Immediate Resuscitation: High-flow O₂, aggressive IV fluids, broad-spectrum antibiotics, and correction of metabolic acidosis.
- Anticoagulation: Start systemic anticoagulation with an IV heparin drip immediately upon suspicion, even before definitive diagnosis.
- Definitive Therapy: Guided by clinical stability and presence of peritonitis.
⭐ A planned "second-look" laparotomy in 24-48 hours is often required to re-evaluate bowel viability after initial resection and revascularization.
High‑Yield Points - ⚡ Biggest Takeaways
- Acute mesenteric ischemia (AMI) presents with severe abdominal pain "out of proportion" to the physical exam, often linked to atrial fibrillation.
- The Superior Mesenteric Artery (SMA) is most commonly affected by an embolic event.
- Chronic mesenteric ischemia causes "intestinal angina": crampy postprandial pain that leads to food fear and weight loss.
- CT angiography (CTA) is the gold standard for diagnosis.
- Metabolic acidosis with an elevated serum lactate is a late and ominous sign.
- Treatment is emergent revascularization and possible bowel resection.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

