Etiology & Pathophysiology - The Breach
-
Common Causes:
- Peptic Ulcer Disease (PUD): Most frequent, esp. anterior duodenal ulcers.
- Diverticulitis: Particularly sigmoid colon.
- Appendicitis: Rupture leading to peritonitis.
- Malignancy: Gastric or colorectal tumors eroding the wall.
- Trauma: Blunt or penetrating injuries.
- Iatrogenic: Post-procedural (e.g., colonoscopy, ERCP) or surgical.
- Bowel Obstruction: Ischemic necrosis or cecal blowout.
- Inflammatory Bowel Disease (IBD): Crohn's (transmural), toxic megacolon (UC).
-
Pathophysiology Cascade:
- Breach of GI wall → Leakage of luminal contents (air, bacteria, enzymes, feces).
- Chemical peritonitis → Bacterial peritonitis → Systemic inflammation (SIRS).
- Fluid shift to peritoneum ("third spacing") → Hypovolemia & septic shock.

⭐ The most common cause of pneumoperitoneum is a perforated duodenal ulcer. Free air under the diaphragm on an upright chest X-ray is the classic sign.
Clinical Presentation & Diagnosis - The Alarm Bells
- History & Symptoms:
- Sudden, severe, diffuse abdominal pain (“thunderclap” onset).
- Syncope can occur due to profound vagal response.
- Referred shoulder pain (Kehr's sign) from diaphragmatic irritation.
- Physical Exam Findings:
- Signs of peritonitis: guarding, rigidity, rebound tenderness.
- Classic "board-like" abdomen is pathognomonic.
- Systemic signs: Tachycardia, hypotension, fever (SIRS).
⭐ On exam, diminished liver dullness to percussion can be an early clue to pneumoperitoneum before imaging is even done.

Management - The Fix-It Crew
Immediate resuscitation is key. The approach follows a structured algorithm, often leading to surgical intervention.
-
Initial Stabilization (The ABCs):
- NPO (Nil Per Os) & Nasogastric (NG) tube for gastric decompression.
- Aggressive IV fluid resuscitation (crystalloids).
- Broad-spectrum IV antibiotics (e.g., Piperacillin-Tazobactam) to cover gram-negatives and anaerobes.
- Insert a Foley catheter to monitor urine output.
-
Definitive Treatment:
- The primary goal is source control (closing the perforation) and peritoneal lavage.
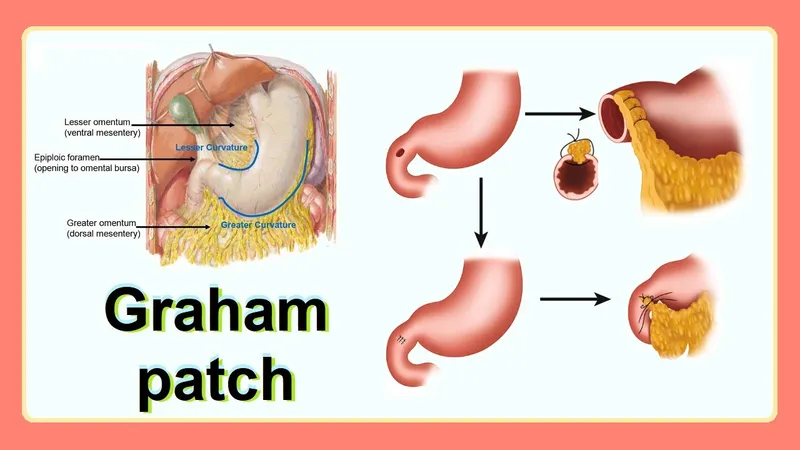
⭐ For a perforated peptic ulcer, an omental patch repair (Graham patch) is a common and effective technique. This involves suturing a piece of the omentum over the perforation to seal it.
High‑Yield Points - ⚡ Biggest Takeaways
- Peptic ulcer disease, particularly duodenal ulcers, is the leading cause of GI perforation.
- The classic presentation is sudden-onset, severe, diffuse abdominal pain followed by a rigid, board-like abdomen from peritonitis.
- An upright chest X-ray is the best initial test to detect pneumoperitoneum (free air under the diaphragm).
- Abdominal CT scan is the most sensitive imaging modality for diagnosis.
- Management is an emergency: IV fluids, broad-spectrum antibiotics, and immediate exploratory laparotomy.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

