Obstructive Sleep Apnea (OSA) - The Airway Blockade
- Pathophysiology: Repetitive collapse of the pharyngeal airway during sleep, leading to apnea (cessation of airflow ≥10s) or hypopnea (↓ airflow by ≥30% with ≥3% O₂ desaturation).
- Risk Factors: Obesity (BMI >30), male gender, age >40, large neck circumference (>17" men, >16" women), alcohol/sedatives, smoking.
- Clinical Presentation: Excessive daytime sleepiness, loud snoring, witnessed apneas, morning headaches, non-restorative sleep.
- 📌 STOP-BANG screening: Snoring, Tiredness, Observed apnea, high blood Pressure, BMI >35, Age >50, Neck >40cm, Gender male.
- Diagnosis:
- Gold standard: In-lab polysomnography (PSG).
- Apnea-Hypopnea Index (AHI):
- Mild: 5-15 events/hour
- Moderate: 15-30 events/hour
- Severe: >30 events/hour
- Management:
- CPAP (Continuous Positive Airway Pressure): First-line therapy.
- Lifestyle: Weight loss, positional therapy (avoid supine), avoid alcohol.
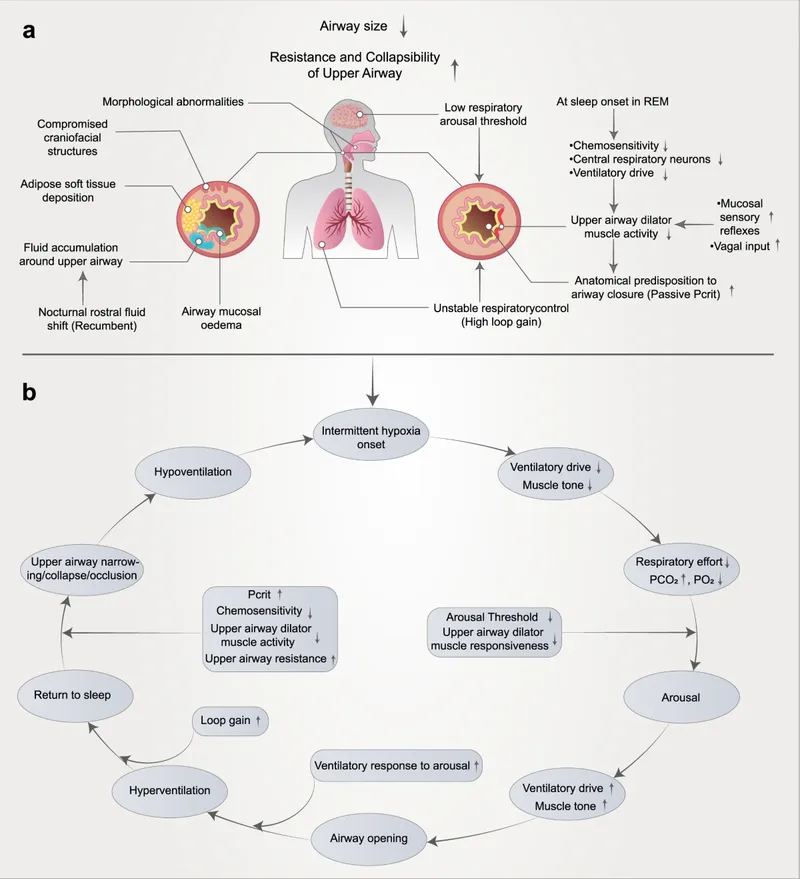
⭐ OSA is a major secondary cause of hypertension and is strongly associated with cardiovascular morbidity (e.g., MI, stroke, atrial fibrillation).
Central Sleep Apnea (CSA) - The Brain's Pause Button
- Pathophysiology: Transient ↓ or cessation of respiratory drive from the CNS, leading to absent respiratory effort.
- Key Differentiator from OSA: No effort to breathe during apneic episodes.
- Etiology:
- Idiopathic: No identifiable cause.
- Cheyne-Stokes Breathing: Crescendo-decrescendo pattern, often seen in heart failure (CHF).
- Meds: Opioids are a major precipitant.
- Neurologic: Stroke, brainstem lesions.
- High Altitude
- Diagnosis: Polysomnography (PSG) shows cessation of both airflow and respiratory effort (thoracic/abdominal movements).
⭐ Cheyne-Stokes breathing, a specific type of CSA with a cyclical crescendo-decrescendo pattern of breathing and apnea, is strongly associated with advanced heart failure.
Diagnosis & Management - Sleuthing & Solving
- Polysomnography (PSG): Gold standard diagnostic test. Measures Apnea-Hypopnea Index (AHI).
- Mild OSA: AHI 5-15
- Moderate OSA: AHI 15-30
- Severe OSA: AHI >30
- Management Strategy:
- Positive Airway Pressure (PAP): First-line therapy.
- CPAP for Obstructive Sleep Apnea (OSA).
- BiPAP/ASV for Central Sleep Apnea (CSA) or CPAP failure.
- Adjunctive: Weight loss, positional therapy, avoiding alcohol before bed.
- Alternatives: Mandibular advancement devices, surgical options (e.g., UPPP).
- Positive Airway Pressure (PAP): First-line therapy.
⭐ Untreated OSA is a significant independent risk factor for developing systemic hypertension and atrial fibrillation.
- Obstructive Sleep Apnea (OSA) results from upper airway collapse, strongly associated with obesity and large neck circumference.
- Diagnosis is confirmed by polysomnography showing an apnea-hypopnea index (AHI) of ≥ 15/hour, or ≥ 5/hour with symptoms.
- CPAP is the first-line treatment; weight loss is a key management component.
- Untreated OSA is a major risk factor for systemic hypertension, arrhythmias, and stroke.
- Central Sleep Apnea (CSA) is characterized by absent respiratory effort, often linked to heart failure or opioid use.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

