Benzos & Z-Drugs - The GABA Boosters
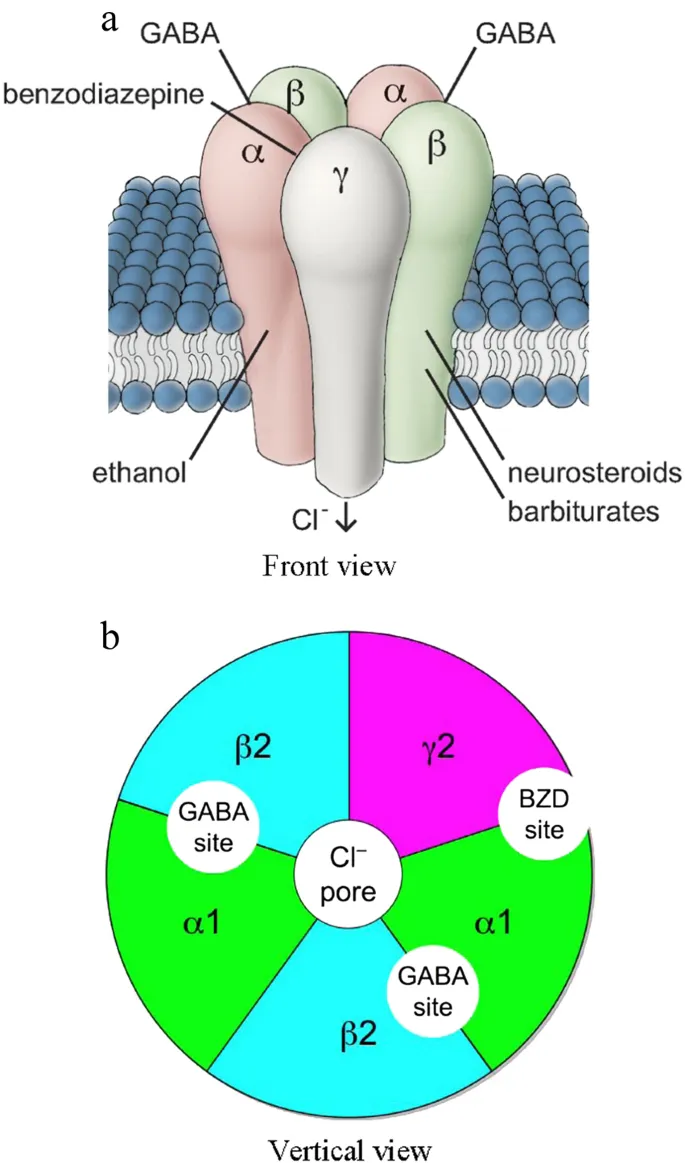
- MoA: Potentiate GABA-A receptors, ↑ frequency of Cl⁻ channel opening → hyperpolarization & CNS depression.
- Agents:
- Benzodiazepines: Temazepam, Triazolam. Less selective (also anxiolytic, myorelaxant).
- Z-Drugs: Zolpidem, Zaleplon, Eszopiclone. More selective for α1-subunit; primarily hypnotic.
- Use: Short-term insomnia management (sleep onset & maintenance).
- Adverse Effects:
- Tolerance, dependence, withdrawal.
- Rebound insomnia.
- Anterograde amnesia, daytime sedation.
- ↑ Fall risk in the elderly.
- ⚠️ Complex sleep behaviors (e.g., sleep-driving), esp. with Z-drugs.
⭐ Z-drugs (e.g., Zolpidem) have less effect on sleep architecture than benzodiazepines but still carry significant risks of dependence and complex sleep-related behaviors.
Orexin & Melatonin Agents - The Switch Flippers
- Suvorexant, Lemborexant
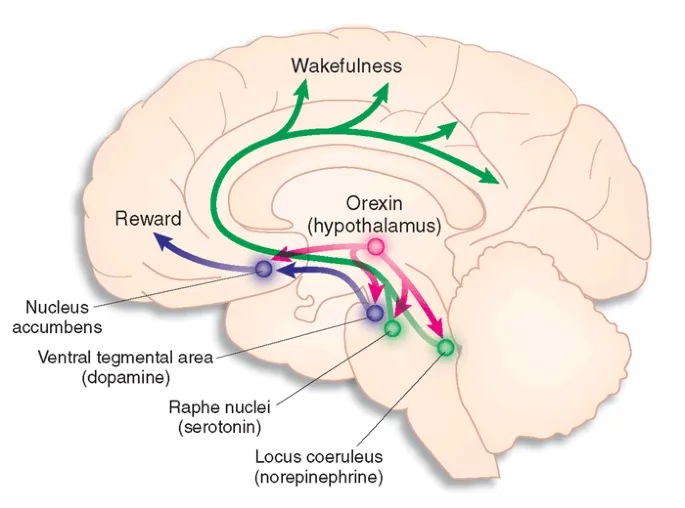
- Mechanism: Dual Orexin Receptor Antagonists (DORAs). Block orexin-A & B from binding to OX1R & OX2R.
- Physiology: Orexin system promotes wakefulness. DORAs inhibit this, acting as a "switch" to turn off arousal systems.
- Use: Insomnia (sleep onset & maintenance).
- Side Effects: Next-day somnolence, sleep paralysis, complex sleep behaviors.
- Ramelteon, Tasimelteon
- Mechanism: Selective agonists for MT1 & MT2 melatonin receptors in the suprachiasmatic nucleus (SCN).
- Ramelteon: For sleep-onset insomnia.
- Tasimelteon: For non-24-hour sleep-wake disorder (e.g., in blind individuals).
⭐ Unlike benzodiazepines, melatonin agonists do not disrupt sleep architecture and have no risk of dependence, rebound insomnia, or withdrawal.
Narcolepsy Meds - The Wake-Up Crew
Primary goals: ↑ daytime wakefulness & ↓ cataplexy.
-
Wakefulness-Promoting Agents (1st Line for EDS):
- Modafinil & Armodafinil: Atypical stimulants with low abuse potential. Primary choice.
- Solriamfetol: A dopamine-norepinephrine reuptake inhibitor (DNRI).
- Pitolisant: A histamine H3-receptor antagonist/inverse agonist.
-
For Cataplexy & EDS:
- Sodium Oxybate (GHB): GABA-B agonist. Excellent for cataplexy, fragmented sleep, and EDS.
- Antidepressants: TCAs, SSRIs, and venlafaxine are effective for cataplexy by suppressing REM sleep.
⭐ Sodium Oxybate carries a black box warning for CNS depression and abuse/misuse. Co-administration with alcohol or other sedatives is contraindicated due to severe respiratory depression risk.
Antidepressants & Others - The Off-Label Allies
- Trazodone
- Low-dose antidepressant for insomnia; mechanism: H1 & 5-HT2A antagonism.
- ⚠️ Risk of priapism.
- Doxepin (TCA)
- Ultra-low-dose for sleep maintenance via potent H1 blockade.
- Mirtazapine
- Sedating; useful for insomnia with depression or low appetite.
- Side effects: ↑ appetite, weight gain.
- Ramelteon
- Melatonin receptor agonist (MT1/MT2) for sleep-onset difficulty.
- Not a controlled substance.
- Suvorexant
⭐ Dual Orexin Receptor Antagonist (DORA). It promotes sleep by blocking the wake-promoting signals of orexin neuropeptides.
High‑Yield Points - ⚡ Biggest Takeaways
- Benzodiazepines & Z-drugs (e.g., zolpidem) potentiate GABA-A receptors; carry risks of tolerance, dependence, and rebound insomnia.
- Ramelteon, a melatonin receptor agonist, is safe for sleep-onset insomnia, especially in elderly or substance abuse history.
- Suvorexant, an orexin receptor antagonist, is effective for both sleep onset and maintenance difficulties.
- Low-dose trazodone is frequently used for insomnia in depression; be aware of the rare risk of priapism.
- Modafinil is first-line therapy for the excessive daytime sleepiness of narcolepsy.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

