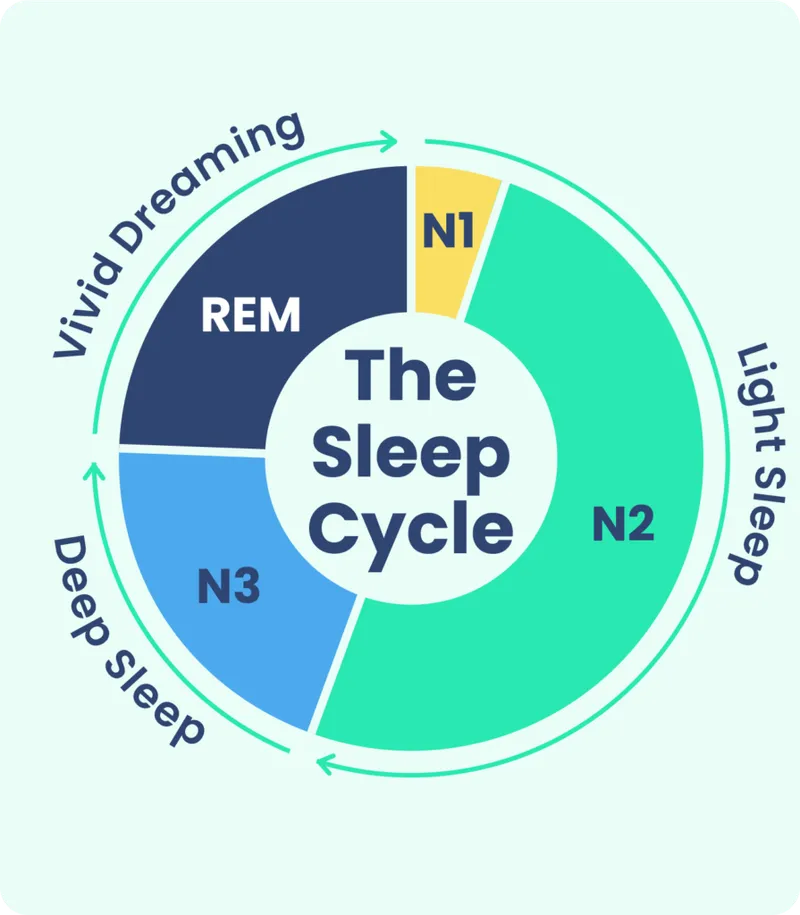
Parasomnias - Unwanted Night Guests
- NREM Arousal Disorders (Slow-wave N3 sleep; first half of night)
- Sleepwalking (Somnambulism): Complex motor behaviors. Amnesia for event.
- Sleep Terrors: Abrupt terror, screaming, autonomic arousal (↑HR, ↑RR). Inconsolable, amnesia.
- REM-Related Parasomnias (Second half of night; dream recall)
- Nightmare Disorder: Recurrent frightening dreams. Recalls details.
- REM Sleep Behavior Disorder (RBD): Dream-enacting behaviors, often violent. Lack of normal muscle atonia.
⭐ RBD is a strong predictor of future neurodegeneration (e.g., Parkinson disease, Lewy body dementia).
NREM Disorders - Sleepwalking & Screaming
- Pathophysiology: Disorders of arousal from non-rapid eye movement (NREM) sleep, specifically stage N3 (slow-wave). Occur in the first ⅓ of the night.
- Core Features: Incomplete awakenings, unresponsiveness to comfort, and anterograde amnesia for the event. Eyes may be open.
- Sleepwalking (Somnambulism):
- Complex motor behaviors (e.g., walking, eating, leaving the house).
- Primary concern is risk of injury.
- Sleep Terrors (Pavor Nocturnus):
- Sudden, terrifying screams with significant autonomic arousal (tachycardia, tachypnea, diaphoresis).
- Child appears terrified and is inconsolable.
- Management:
- Primary: Reassurance and safety measures (lock doors/windows, remove hazards).
- Pharmacotherapy (if severe/injurious): Low-dose benzodiazepines.
⭐ Key Distinction: Unlike nightmares (REM sleep), patients have no recall of sleep terror or sleepwalking episodes and typically occur earlier in the night.
REM Disorders - Acting Out Dreams
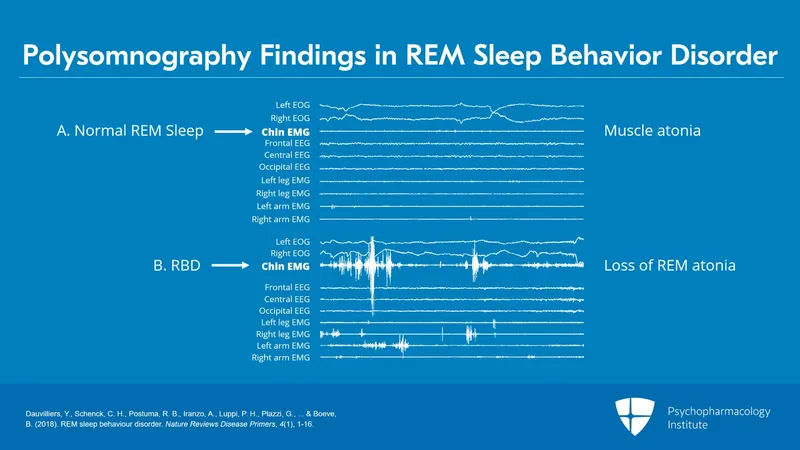
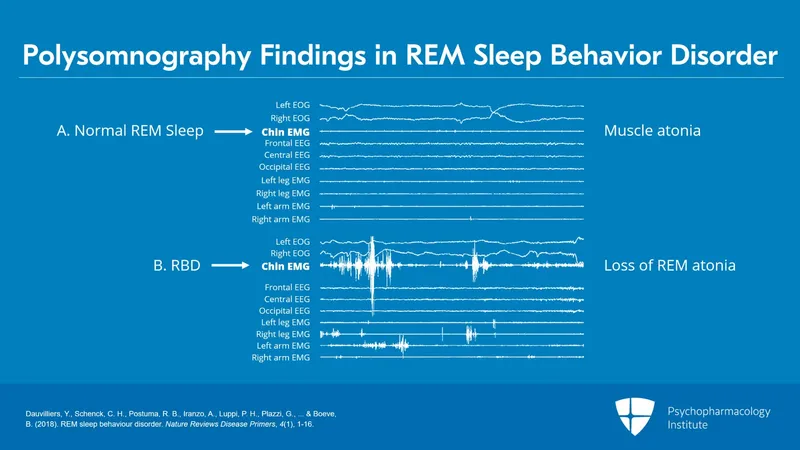
- Pathophysiology: Characterized by the loss of normal muscle atonia during REM sleep, leading to dream-enacting behaviors.
- Clinical Picture: Patients physically and often violently act out vivid dreams. They can be awakened easily and will recall the dream. Common in men > 50 years old.
- Diagnosis: Polysomnography (PSG) demonstrates REM sleep without atonia.
- Treatment:
- Ensure environmental safety (remove weapons/dangerous objects from bedroom).
- Clonazepam (low-dose) is first-line.
- Melatonin is an alternative.
⭐ High-Yield: RBD is a major prodromal symptom for neurodegenerative diseases. Up to 80% of patients will develop an α-synucleinopathy, such as Parkinson disease or Lewy Body Dementia, often within a decade.
📌 Rapid Eye Movements become Real Enacted Movements.
Workup & Treatment - Taming the Night
-
Workup
- Begin with a detailed sleep history from the patient and bed partner.
- Rule out secondary causes: medications, substances, other sleep disorders (e.g., OSA).
- Polysomnography (PSG): Gold standard to confirm diagnosis, especially differentiating NREM disorders from nocturnal seizures and identifying REM sleep without atonia in RBD.
-
Treatment
- Foundation: Reassurance and strict safety precautions (e.g., removing dangerous objects, securing windows).
- NREM Parasomnias: If severe/injurious, consider low-dose benzodiazepines (e.g., Clonazepam 0.5-2 mg).
- REM Sleep Behavior Disorder (RBD): Clonazepam is first-line; Melatonin is a common alternative.
⭐ REM Sleep Behavior Disorder (RBD) is a powerful predictor for future development of an α-synucleinopathy, such as Parkinson's disease or Lewy body dementia.
- NREM parasomnias (sleepwalking, sleep terrors) occur in the first half of the night during N3 sleep, with no memory of the event.
- REM sleep behavior disorder (RBD) involves acting out dreams in the second half of the night and strongly predicts future α-synucleinopathies (e.g., Parkinson's).
- Nightmare disorder also occurs during REM sleep but features distressing dreams without motor activity and with full recall upon awakening.
- Management for all parasomnias prioritizes safety measures and reassurance.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

