Insomnia Disorder - The Wide-Awake Club
- Difficulty initiating or maintaining sleep, or nonrestorative sleep, leading to daytime impairment.
- Diagnostic criteria: Symptoms ≥3 nights/week for ≥3 months, despite adequate opportunity for sleep.
- Management focuses on identifying and treating underlying causes.

⭐ Cognitive Behavioral Therapy for Insomnia (CBT-I) is the first-line treatment and is more effective long-term than medication.
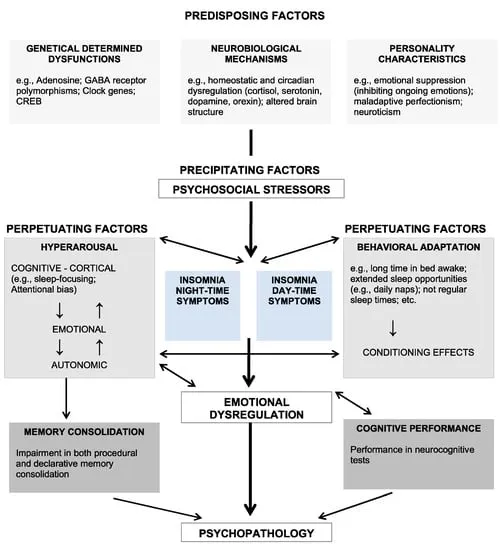
Pathophysiology - The 3P Hyperarousal Model
-
Core Concept: Insomnia results from a state of hyperarousal, where predisposing traits are triggered by a precipitating event, and the resulting sleep disturbance is maintained by perpetuating factors.
-
The 3 Ps:
- Predisposing: Baseline vulnerability (e.g., genetics, anxiety traits).
- Precipitating: Acute triggers (e.g., life stressor, illness).
- Perpetuating: Factors that maintain insomnia (e.g., poor sleep hygiene, catastrophic thoughts about sleep).
⭐ First-line treatment, Cognitive Behavioral Therapy for Insomnia (CBT-I), directly targets the perpetuating factors (maladaptive behaviors and cognitive distortions) that maintain chronic insomnia.
Diagnosis & Workup - The Sleep Detective
- Clinical Interview is Primary: Detailed history of sleep patterns (bedtime, latency, awakenings), daytime dysfunction, and psychiatric/medical history.
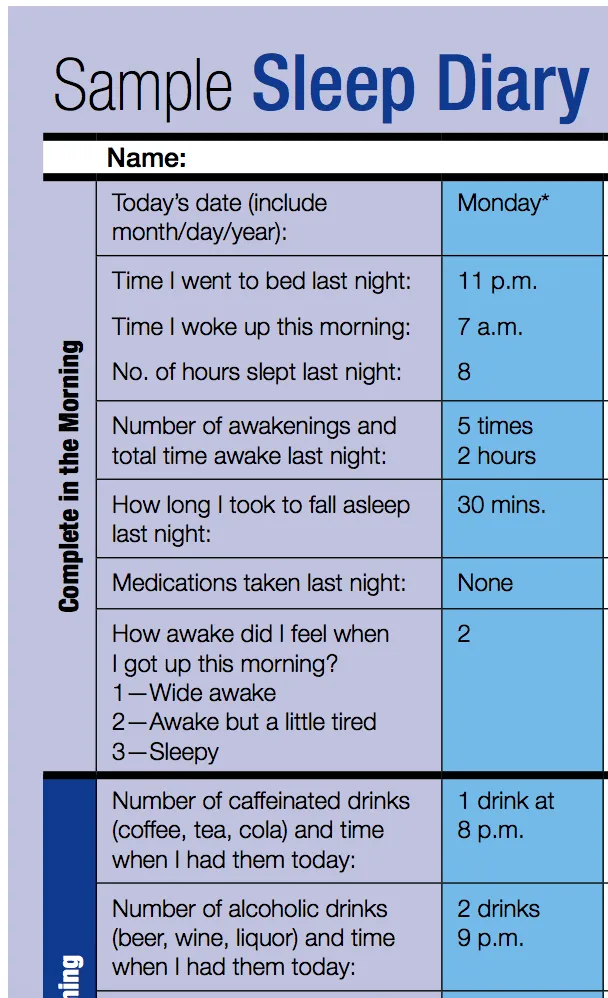
- Sleep Diary/Log: Patient tracks sleep for 1-2 weeks to identify patterns. The cornerstone of behavioral assessment.
- Actigraphy: Wrist-worn device provides objective data on sleep-wake cycles; useful when subjective reports are unclear.
- Polysomnography (PSG): Not routinely indicated. Reserved for suspected comorbid sleep disorders (e.g., sleep apnea, periodic limb movement disorder).
⭐ Exam Favorite: Insomnia is a major risk factor for and is frequently comorbid with Major Depressive Disorder (MDD). Always screen for mood symptoms.
📌 Mnemonic "3-3-3": Difficulty initiating/maintaining sleep for ≥3 nights/week for ≥3 months, causing significant distress/impairment.
Management - CBT-I Before Pills
-
First-Line Therapy: CBT-I is the preferred initial treatment for chronic insomnia, recommended over pharmacotherapy due to its durable effects and lack of medication-related side effects.
-
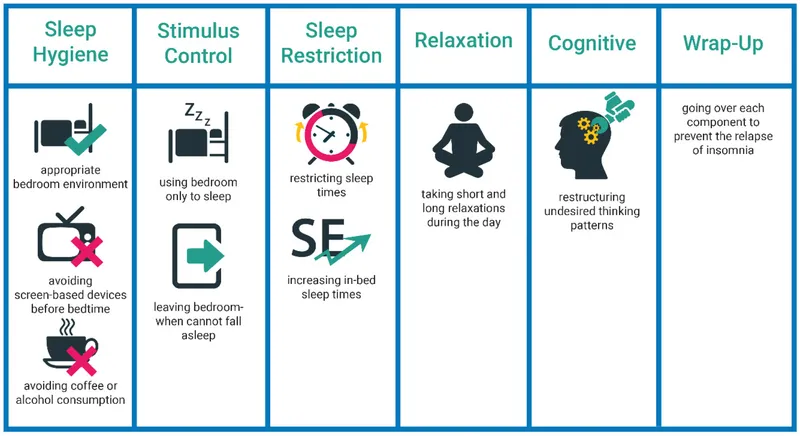
Core Components:
- Stimulus Control: Re-associate the bedroom with sleep. If not asleep in 20 min, leave the room. Use bed only for sleep/intimacy.
- Sleep Restriction: Limit time in bed to the actual time spent sleeping to improve sleep efficiency.
- Cognitive Therapy: Challenge dysfunctional beliefs about sleep (e.g., "I need 8 hours to function").
- Relaxation Training: Diaphragmatic breathing, progressive muscle relaxation.
- Sleep Hygiene: Foundational but insufficient alone.
⭐ Exam Favorite: The therapeutic effects of CBT-I are more sustained over time compared to sedative-hypnotic medications, which often have waning efficacy and risk of dependence.
High‑Yield Points - ⚡ Biggest Takeaways
- Insomnia disorder is defined by difficulty initiating or maintaining sleep, occurring at least 3 nights per week for ≥3 months, causing significant functional impairment.
- Cognitive Behavioral Therapy for Insomnia (CBT-I) is the undisputed first-line treatment and is more effective long-term than pharmacotherapy.
- If medication is needed, use short-term; non-benzodiazepines (e.g., zolpidem, eszopiclone) are preferred over benzodiazepines.
- Always rule out comorbid medical or psychiatric conditions, substance use, and poor sleep hygiene.
- Associated with increased risk of depression, anxiety, and accidents.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

