Mechanism of Action - Atypical Balancing Act
- Primary Action: Combined Dopamine $D_2$ receptor and Serotonin $5-HT_{2A}$ receptor antagonism.
- Mesolimbic Pathway: $D_2$ blockade → ↓ positive symptoms (hallucinations, delusions).
- Mesocortical Pathway: $5-HT_{2A}$ blockade > $D_2$ blockade → ↑ dopamine release → alleviates negative & cognitive symptoms.
- Nigrostriatal Pathway: Serotonin blockade counters dopamine blockade → protective against extrapyramidal symptoms (EPS).
- Tuberoinfundibular Pathway: $D_2$ blockade → ↑ prolactin levels (hyperprolactinemia).
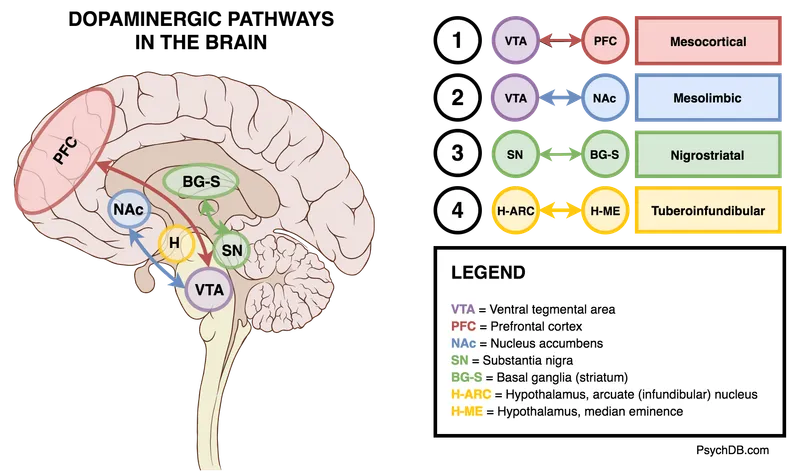
⭐ Exam Favorite: The lower risk of EPS with atypicals is attributed to potent $5-HT_{2A}$ antagonism, which stimulates downstream dopamine release in the nigrostriatal pathway, overriding the $D_2$ blockade.
Key Agents - The Atypical Lineup
- Risperidone (Risperdal): Highest risk of hyperprolactinemia among SGAs due to potent D2 blockade. Available as a long-acting injectable (LAI).
- Olanzapine (Zyprexa): High risk for metabolic syndrome (↑ weight, ↑ lipids, ↑ glucose). 📌 "Olanzapine makes you Obese."
- Quetiapine (Seroquel): Highly sedating (H1 blockade), making it useful for patients with insomnia. Low EPS risk.
- Aripiprazole (Abilify): Unique partial D2 agonist mechanism. Can be activating; common side effect is akathisia.
- Ziprasidone (Geodon): Associated with QTc prolongation. ⚠️ Must be taken with a >500 kcal meal.
- Clozapine (Clozaril): Most effective agent, reserved for treatment-resistant schizophrenia.
⭐ Clozapine is uniquely effective but carries a 1% risk of agranulocytosis, requiring mandatory weekly ANC monitoring for the first 6 months.
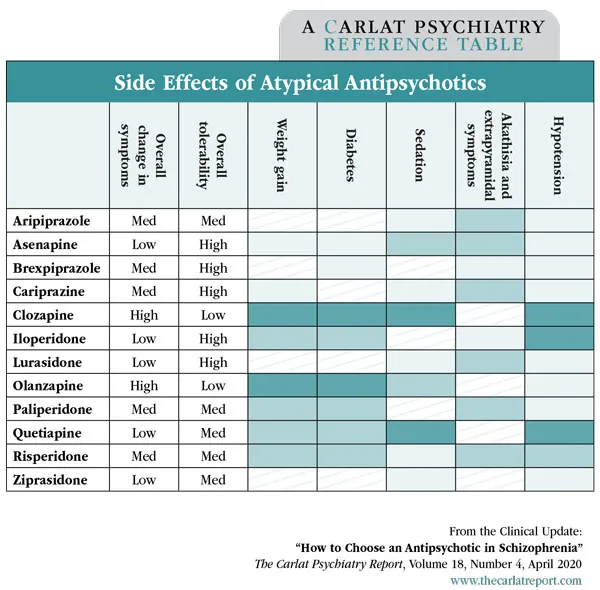
Adverse Effects - Metabolic Mayhem & More
-
Metabolic Syndrome: Major concern, highest risk with clozapine and olanzapine.
- Weight Gain: Significant and common.
- Dyslipidemia: ↑ triglycerides and cholesterol.
- Hyperglycemia: Risk of new-onset Type 2 Diabetes.
-
Monitoring Protocol:
- Other Key Adverse Effects:
- Hyperprolactinemia: Esp. risperidone, paliperidone → gynecomastia, amenorrhea.
- QTc Prolongation: Highest risk with ziprasidone.
- Sedation/Orthostasis: Common with clozapine, quetiapine.
- ⚠️ Agranulocytosis: Clozapine only. Requires strict ANC monitoring.
⭐ Clozapine is reserved for treatment-resistant schizophrenia due to its superior efficacy but carries a ~1% risk of agranulocytosis, requiring absolute neutrophil count (ANC) to be >1500/μL before starting treatment.
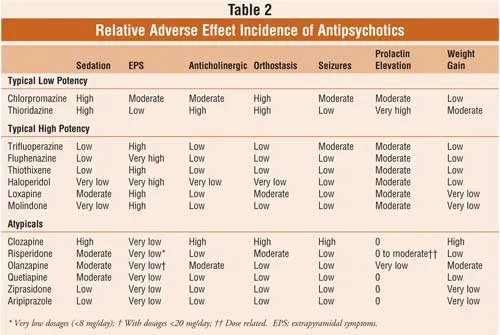
Clinical Choice - The Right Drug, Right Time
- Guiding Principle: Individualize choice based on side-effect profile, patient comorbidities, and prior treatment responses.
- Metabolic Syndrome: For patients with or at high risk for obesity/diabetes, prefer agents with lower metabolic risk like Aripiprazole, Lurasidone, or Ziprasidone.
- Non-Adherence: Consider long-acting injectable (LAI) formulations (e.g., Paliperidone, Aripiprazole) to improve compliance.
⭐ Clozapine is uniquely effective for treatment-resistant schizophrenia (failure of 2 other antipsychotics) but requires regular ANC monitoring due to the risk of agranulocytosis.
High‑Yield Points - ⚡ Biggest Takeaways
- Second-generation antipsychotics (SGAs) block both D2 and 5-HT2A receptors.
- They are effective against both positive and negative symptoms of schizophrenia.
- SGAs have a lower risk of EPS and tardive dyskinesia but a higher risk of metabolic syndrome.
- Clozapine is used for treatment-resistant cases and carries a risk of agranulocytosis.
- Risperidone is most associated with hyperprolactinemia.
- Olanzapine and clozapine carry the highest risk for weight gain and metabolic issues.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

