Overview & Epidemiology - The Monthly Storm
- A severe, disabling form of premenstrual syndrome (PMS) marked by prominent affective symptoms: irritability, depression, and anxiety.
- Symptoms cyclically appear during the late luteal phase of the menstrual cycle and remit within a few days of menses onset.
- Prevalence is estimated at 1.8-5.8% of menstruating women, leading to significant distress and functional impairment.
⭐ Prospective daily symptom charting over at least 2 menstrual cycles is required for diagnosis.
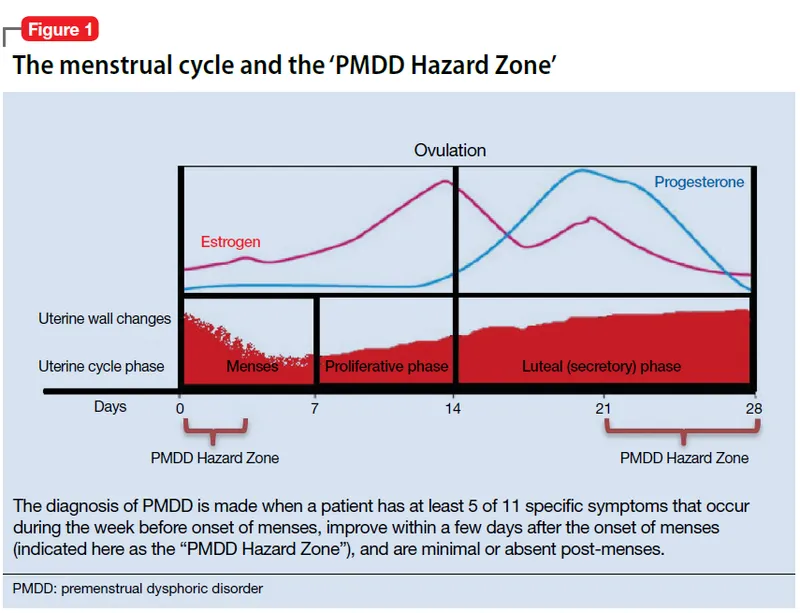
Pathophysiology - Hormone Havoc
- Central Defect: Not abnormal hormone levels, but an abnormal CNS response to normal luteal phase changes in estrogen and progesterone.
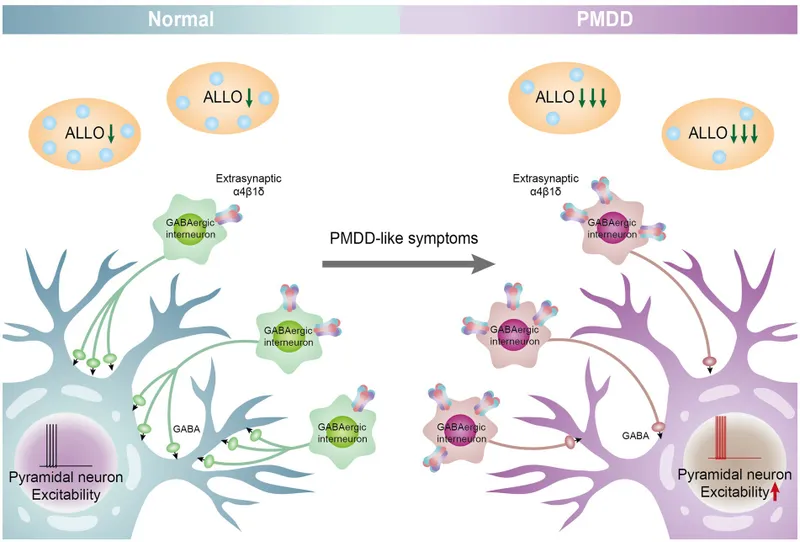
- Neurotransmitter Dysregulation: These hormonal shifts disrupt serotonin (5-HT) and GABAergic systems.
- Key Culprit: Allopregnanolone (a progesterone metabolite) interaction with GABA-A receptors is critical.
⭐ Paradoxical Reaction: In susceptible women, allopregnanolone triggers anxiety and irritability instead of its usual calming, anxiolytic effect.
Clinical Presentation & Diagnosis - Charting the Cycle
- DSM-5 Criteria: Requires ≥5 symptoms in the final week before menses (luteal phase), improving after onset, and minimal post-menses.
- ≥1 Core Mood Symptom:
- Affective lability (mood swings)
- Irritability or ↑ interpersonal conflicts
- Depressed mood, hopelessness
- Anxiety, tension, feeling "on edge"
- ≥1 Additional Symptom: Anhedonia, ↓ concentration, lethargy, appetite changes, sleep changes, feeling overwhelmed, or physical symptoms (e.g., breast tenderness, bloating).
- ≥1 Core Mood Symptom:
⭐ Exam Favourite: The diagnosis cannot be made retrospectively. It requires prospective daily charting for at least 2 consecutive menstrual cycles to confirm the cyclical nature of symptoms and functional impairment.
Differential Diagnosis - More Than Just PMS
- Premenstrual Syndrome (PMS): Milder, less numerous symptoms without the significant distress or functional impairment seen in PMDD.
- Major Depressive Disorder (MDD) & Dysthymia: Symptoms are persistent and not confined to the luteal phase.
- Bipolar Disorder: Characterized by manic or hypomanic episodes that are not cyclically tied to menses.
- Anxiety Disorders: Chronic anxiety symptoms, not just premenstrual.
⭐ A pre-existing disorder (e.g., MDD) may show premenstrual exacerbation, but PMDD requires symptom-free intervals post-menses.
Management & Treatment - Taming the Tide
- First-Line: SSRIs are the cornerstone.
- Options: Continuous daily dosing OR luteal phase-only dosing (start on cycle day 14, stop at menses).
- Agents: Fluoxetine, Sertraline, Citalopram.
- Second-Line:
- Switch to a different SSRI or SNRI (Venlafaxine).
- Oral Contraceptives (OCPs), especially those containing drospirenone (a progestin with anti-androgenic & anti-mineralocorticoid effects).
- Refractory Cases:
- GnRH agonists (e.g., Leuprolide) → induce a temporary, reversible menopause.
- Requires add-back therapy (estrogen/progestin) to mitigate hypoestrogenic side effects.
⭐ Exam Favorite: Unlike in major depression, SSRIs often provide rapid symptom relief within days to 1-2 cycles for PMDD, suggesting a non-serotonergic, possibly allopregnanolone-related mechanism.
High‑Yield Points - ⚡ Biggest Takeaways
- Core feature is the timing: symptoms arise in the late luteal phase and remit with menses.
- Requires prospective daily ratings over ≥2 symptomatic menstrual cycles for diagnosis.
- Characterized by marked affective lability, irritability, depression, or anxiety.
- Differentiated from PMS by severity and significant distress or functional impairment.
- First-line treatment is SSRIs (e.g., fluoxetine, sertraline), which can be dosed continuously or cyclically.
- OCPs are a second-line option.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

