Overview - Kiddie Blues Basics
- Presentation varies from adults; chronic irritability can be a core symptom instead of overt sadness.
- Core neurovegetative symptoms (sleep, appetite, energy) are key, but look for school failure & social withdrawal.
- High comorbidity: Anxiety, ADHD, ODD/Conduct Disorder.
⭐ A first major depressive episode in childhood/adolescence is a major risk factor for future suicide attempts and developing Bipolar I Disorder.
Major Depressive Disorder (MDD) - Grumpy Kid Syndrome
Hallmark pediatric symptom is persistent irritability instead of sadness. Diagnosis requires ≥5 symptoms over ≥2 weeks, significantly impairing function.
📌 Pediatric SIGECAPS:
- Irritability / Anhedonia (at least one required)
- Sleep disturbance
- Guilt or worthlessness
- Energy loss
- Concentration difficulty
- Appetite change or failure to make expected weight gains
- Psychomotor agitation/retardation
- Suicidal ideation

⭐ A first episode of MDD in childhood or adolescence is a significant predictor for developing Bipolar I Disorder.
Bipolar & Related Disorders - Pediatric Mood Swings
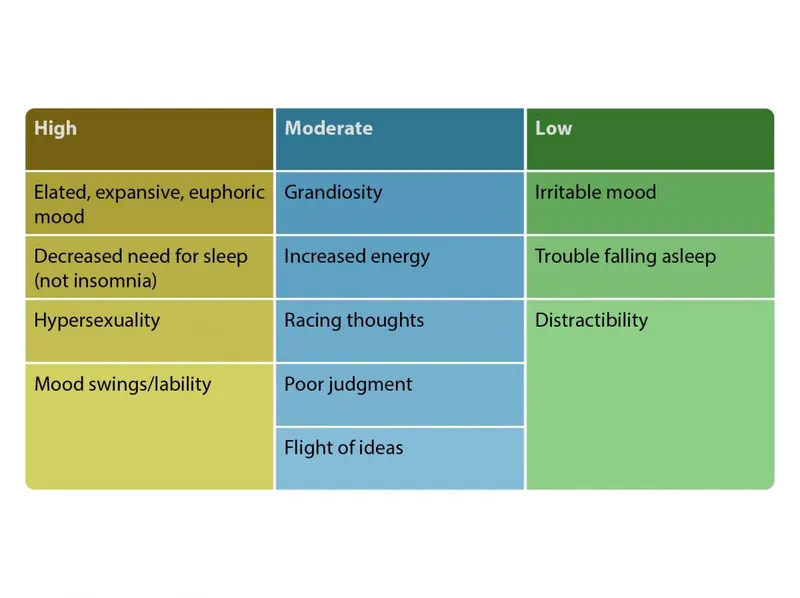
- Core Presentation: Unlike adult euphoria, pediatric cases often show severe, non-episodic irritability, temper tantrums, and aggressive outbursts. Mood is labile and reactive.
- Key Differentiators:
- vs. ADHD: Look for distinct mood episodes (mania/hypomania, depression). ADHD has a more pervasive pattern of hyperactivity/inattention without clear mood cycles.
- vs. DMDD: DMDD features chronic irritability without the discrete manic/hypomanic episodes required for a bipolar diagnosis.
⭐ A family history of bipolar disorder in a first-degree relative is the strongest risk factor.
Disruptive Mood Dysregulation Disorder (DMDD) - Temper Tantrum Turmoil
- Core: Severe recurrent temper outbursts (verbal/behavioral) grossly out of proportion to the situation, occurring ≥3 times/week.
- Mood Baseline: Persistently irritable or angry nearly every day between outbursts.
- Diagnostic Window: Symptom onset must be before age 10.
⭐ Key function is to reduce the overdiagnosis of pediatric bipolar disorder by distinguishing chronic irritability from the episodic mania seen in bipolar disorder.
Treatment Principles - Fixing the Feels
Initial treatment for Major Depressive Disorder (MDD) combines psychotherapy and pharmacotherapy. Bipolar disorder requires mood stabilization.
- Bipolar Disorder:
- Mood Stabilizers: Lithium, Valproate, Lamotrigine.
- Atypical Antipsychotics: Risperidone, Aripiprazole, Olanzapine.
⭐ ⚠️ FDA Black Box Warning: Antidepressants may increase the risk of suicidal thinking and behavior in children, adolescents, and young adults up to age 24.
- Irritability and anger are more common presentations of depression in children than classic sadness.
- Frequent, non-specific somatic complaints (e.g., headaches, stomachaches) are a key sign of depression in youth.
- Disruptive Mood Dysregulation Disorder (DMDD) involves severe, recurrent temper outbursts (≥3x/week) with a persistently irritable mood between episodes.
- Pediatric bipolar disorder often presents with mixed features, rapid cycling, and episodic mood shifts.
- SSRIs carry a black box warning for a potential increase in suicidal ideation in adolescents.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

