Overview - The Heavy Veil
A severe subtype of Major Depressive Disorder (MDD) characterized by a near-complete loss of pleasure (anhedonia) in almost all activities. It feels like a heavy, oppressive blanket, distinct from normal sadness. This subtype points towards more significant biological underpinnings.
- Pervasive Anhedonia: The central feature; an inability to find pleasure in anything.
- Diurnal Variation: Mood is characteristically worse in the morning.
- Psychomotor Disturbance: Observable retardation or agitation.
- Sleep: Early morning awakening, typically ≥2 hours before usual.
⭐ Patients with melancholic features often show a more robust response to somatic treatments like electroconvulsive therapy (ECT) and pharmacotherapy (especially TCAs & SNRIs) than to psychotherapy alone.
Diagnosis - Spotting the Signs
Applies if these features are present during the most severe period of a Major Depressive Episode (MDE). The patient must first meet full MDE criteria.
-
Gateway Criteria (≥1 Required):
- Pervasive Anhedonia: Loss of pleasure in virtually all activities.
- Lack of Mood Reactivity: Mood does not brighten, even temporarily, to positive stimuli.
-
Additional Criteria (≥3 Required):
- Distinct Quality of Mood: Profound despondency or an "empty" mood.
- Diurnal Variation: Depression is consistently worse in the morning.
- Sleep: Early morning awakening (at least 2 hours before usual).
- Psychomotor: Marked psychomotor agitation or retardation.
- Appetite/Weight: Significant anorexia or weight loss.
- Guilt: Excessive or inappropriate guilt.
⭐ Melancholic features are a strong predictor of a favorable response to somatic therapies, particularly Electroconvulsive Therapy (ECT).
Pathophysiology - The Biology of Blight
- Monoamine Hypothesis: Core deficiency in key neurotransmitters: Serotonin (↓ 5-HT), Norepinephrine (↓ NE), and Dopamine (↓ DA).
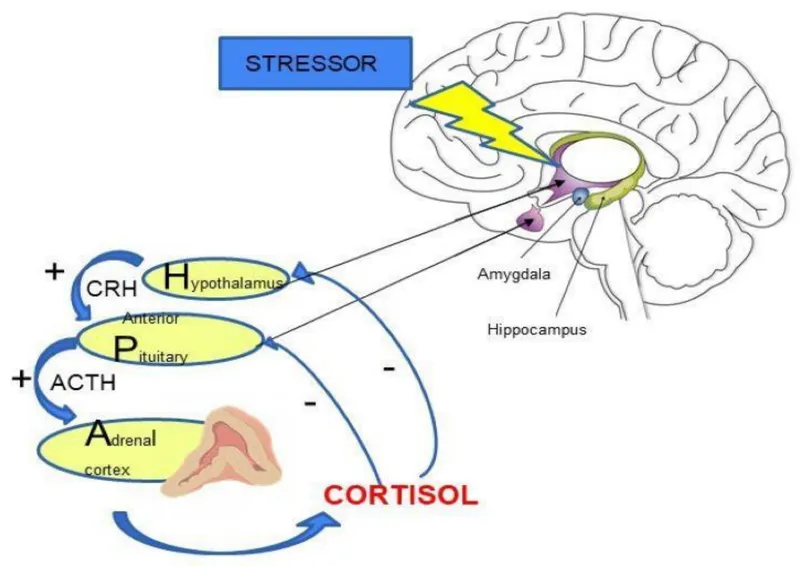
- HPA Axis Dysregulation: Chronic stress leads to hyperactive Hypothalamic-Pituitary-Adrenal axis.
- ↑ CRH & ↑ Cortisol levels.
- Glucocorticoid receptor resistance impairs negative feedback.
- Neuroanatomic Changes:
- ↓ Hippocampal & prefrontal cortex (PFC) volume.
- ↑ Amygdala activity (fear, anhedonia).
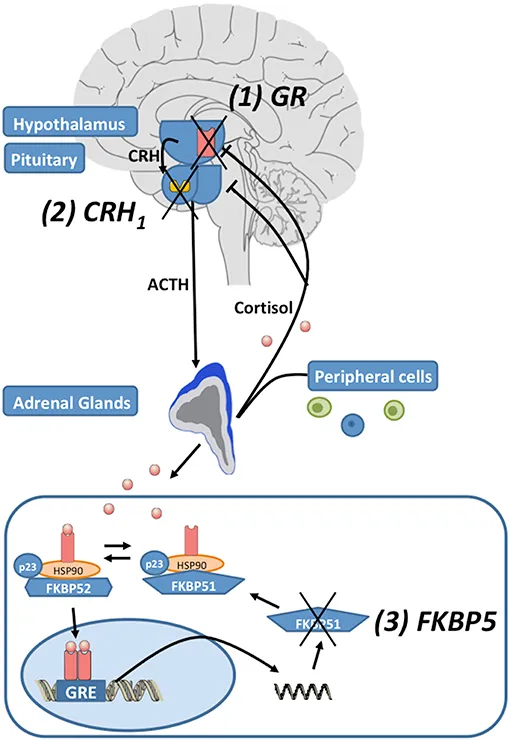
⭐ A hallmark of melancholia is HPA axis hyperactivity, classically demonstrated by the failure to suppress cortisol levels after administering a low dose of dexamethasone (Dexamethasone Suppression Test).
Treatment - Piercing the Gloom
- Pharmacotherapy First: Melancholia often responds better to broader-acting agents.
- Preferred: Tricyclic Antidepressants (TCAs) or SNRIs (Venlafaxine, Duloxetine) over SSRIs alone.
- ⚠️ TCAs: Require careful monitoring (cardiac, anticholinergic effects).
- Somatic Therapies: Highly effective for severe or treatment-refractory cases.
- Electroconvulsive Therapy (ECT): Gold standard for rapid and robust response, especially with psychosis or catatonia.
- TMS: An alternative neuromodulation technique.
- Psychotherapy: Primarily as an adjunct to biological treatments (e.g., CBT, supportive).
⭐ ECT demonstrates the highest remission rates (often >80%) for depression with severe melancholic or psychotic features, surpassing pharmacotherapy.
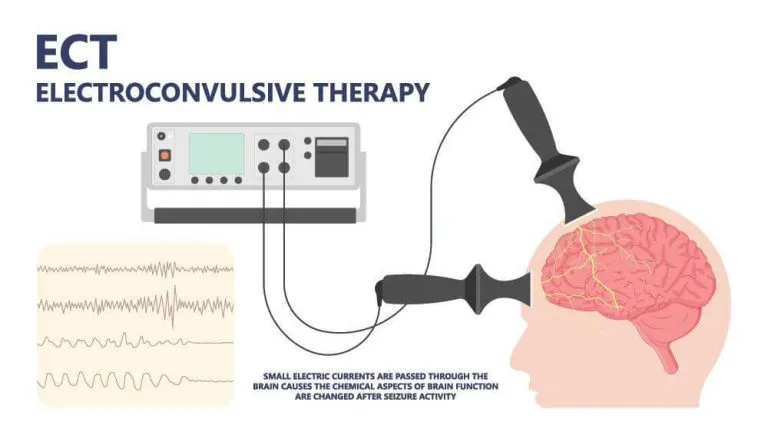 electrode placement)
electrode placement)
High‑Yield Points - ⚡ Biggest Takeaways
- The core feature is pervasive anhedonia, a near-complete loss of pleasure in all activities.
- Symptoms characteristically show diurnal variation, being significantly worse in the morning.
- Expect profound psychomotor retardation or, less commonly, agitation.
- Early morning awakening (at least 2 hours before usual) is a classic sleep disturbance.
- Patients often express excessive or inappropriate guilt over minor matters.
- Significant anorexia or weight loss is a key vegetative sign.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

