Pathophysiology - The Brain's Bad Build-up
FTD results from progressive neuronal loss and focal atrophy in the frontal and temporal lobes. The underlying cause is the accumulation of one of two main abnormal proteins:
-
Tauopathy (~40% of cases)
- Aggregates of hyperphosphorylated tau protein form neurofibrillary tangles.
- The classic finding is the Pick body: a spherical, silver-staining intraneuronal inclusion.
- Associated with mutations in the MAPT gene.
-
TDP-43 Proteinopathy (~50% of cases)
- Cytoplasmic inclusions of TDP-43 protein are the hallmark.

⭐ The C9orf72 gene expansion is the most common genetic cause of both FTD and Amyotrophic Lateral Sclerosis (ALS), creating an FTD-ALS clinical spectrum.
Clinical Presentation - Personality & Language Gone
Presents in two main forms, often before age 65.
-
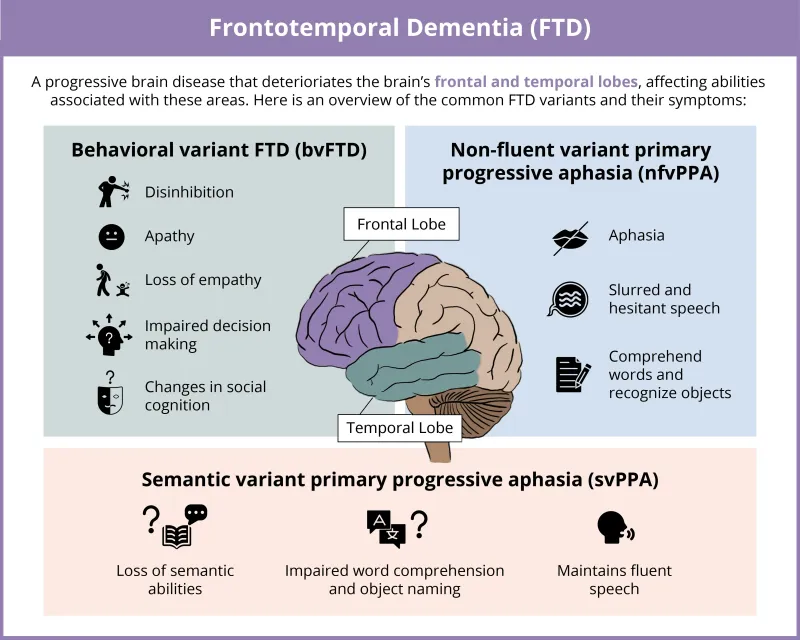
Behavioral Variant (bvFTD): Most common form.
- Personality/Behavioral Changes: Early, prominent signs.
- Disinhibition: Socially inappropriate behavior, impulsivity.
- Apathy: Loss of motivation and interest.
- Loss of Empathy/Sympathy: Emotional blunting.
- Stereotyped/Compulsive Behaviors: Repetitive actions, hoarding.
- Dietary changes: Hyperorality, preference for sweets.
- Personality/Behavioral Changes: Early, prominent signs.
-
Primary Progressive Aphasia (PPA): Language function declines first.
- Semantic Variant (svPPA): "What is a 'fork'?"
- Loss of word/object meaning (anomia).
- Fluent, grammatically correct but empty speech.
- Non-fluent/Agrammatic Variant (nfvPPA): "Fork... eat... food."
- Effortful, halting speech with grammatical errors (agrammatism).
- Apraxia of speech often present.
- Semantic Variant (svPPA): "What is a 'fork'?"
⭐ In early FTD, memory and visuospatial functions are often strikingly preserved, distinguishing it from Alzheimer's disease where memory loss is the initial, dominant feature.
Diagnosis - Finding the Frontal Faults
- Clinical Criteria: Diagnosis relies on international consensus criteria for behavioral variant FTD (bvFTD) or primary progressive aphasia (PPA).
- Neuropsychological Testing: Confirms executive dysfunction (e.g., poor planning, disinhibition) or specific language deficits.
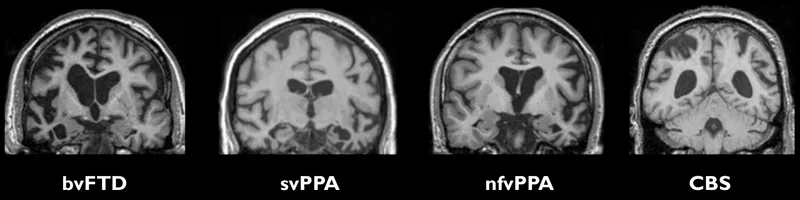
- Neuroimaging: Crucial for diagnosis.
- MRI: Shows characteristic, often asymmetric, atrophy in the frontal and/or temporal lobes.
- PET/SPECT: Reveals ↓ frontotemporal hypometabolism or hypoperfusion, helping differentiate from other dementias.
⭐ Exam Favorite: In contrast to Alzheimer's disease, memory and visuospatial skills are typically well-preserved in the early stages of FTD.
Management - Support, Not Cure
- Core Goal: Primarily symptomatic and supportive, as no disease-modifying therapies currently exist. Focus on safety and quality of life.
- Non-Pharmacologic (First-Line):
- Behavioral redirection, environmental modification.
- Speech, physical, and occupational therapy.
- Pharmacologic (Symptom-Targeted):
- Behavioral: SSRIs (e.g., sertraline) for disinhibition, anxiety, and compulsive behaviors.
- Sleep: Trazodone for insomnia and agitation.
⭐ High-Yield: Unlike Alzheimer's, cholinesterase inhibitors (e.g., donepezil) and memantine are not effective and may worsen agitation in FTD.
High-Yield Points - ⚡ Biggest Takeaways
- Presents at a younger age (<65) than Alzheimer's disease.
- Characterized by early personality and behavior changes (apathy, disinhibition, compulsivity) or language dysfunction.
- Memory and visuospatial skills are relatively preserved in the early stages.
- Two primary variants: behavioral variant (bvFTD) and primary progressive aphasia (PPA).
- Pathology is linked to tau protein (Pick bodies) or TDP-43 proteinopathy.
- Neuroimaging reveals focal atrophy of the frontal and/or temporal lobes.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

