Initial Assessment - The Gentle Detective
First, suspect and rule out delirium. A sudden behavioral change is delirium until proven otherwise. Systematically investigate for underlying triggers before labeling a behavior as "dementia-related."
-
Medical Evaluation:
- Pain: Use the PAINAD scale for non-verbal patients.
- Infection: Check for UTI, pneumonia.
- Medications: Review for new or psychoactive drugs (esp. anticholinergics).
- Metabolic: Check electrolytes, glucose.
- Environment: Look for changes in routine, noise, or caregivers.
-
Behavioral Analysis (ABC Model):
- Antecedent: What triggers the behavior?
- Behavior: Describe the specific action.
- Consequence: What is the response to the behavior?
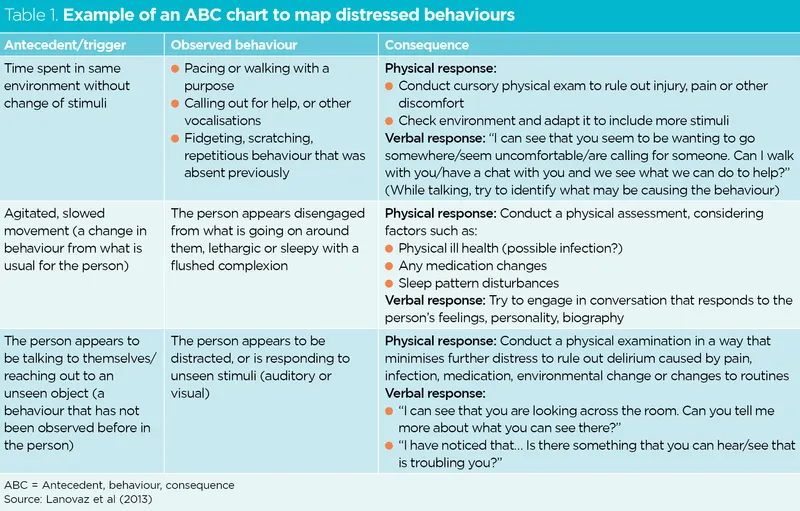
⭐ In a patient with dementia presenting with acute agitation or confusion, the first step is always to screen for delirium by looking for reversible medical causes like infection (UTI), dehydration, or medication side effects.
Non-Pharm Toolkit - No Pills, Just Skills
- First-line approach for Behavioral and Psychological Symptoms of Dementia (BPSD).
- Core Principle: ABC Model
- Antecedent: Identify triggers (e.g., pain, noise, unmet needs like hunger or toileting).
- Behavior: Objectively describe the action (e.g., agitation, shouting).
- Consequence: Observe the response to the behavior.
- Key Strategies (DICE Approach 📌)
- Describe: Chart the ABCs to understand the behavior.
- Investigate: Rule out underlying causes (e.g., delirium, infection, pain).
- Create: Develop a tailored intervention plan.
- Environmental: Simplify surroundings, reduce stimuli, improve lighting. Use safety locks.
- Communication: Use calm, simple, direct language. Avoid arguing. Validate feelings.
- Activities: Structure daily routines. Engage in familiar, pleasant activities (e.g., music, simple chores).
- Evaluate: Monitor effectiveness and adjust the plan as needed.
⭐ Exam Favorite: Always rule out underlying delirium (e.g., from a UTI) or untreated pain before attributing behavioral changes solely to dementia progression.
Pharmacotherapy - The Chemical Calm
- Guiding Principle: Non-pharmacologic interventions are first-line. Medications are reserved for symptoms causing significant distress or risk of harm.
- Antipsychotics (for severe agitation/psychosis):
- Atypicals preferred: Risperidone, Olanzapine, Quetiapine.
- Start with the lowest possible dose and titrate slowly ("start low, go slow").
- ⚠️ BBW: All antipsychotics carry a black box warning for an increased risk of all-cause mortality in elderly patients with dementia-related psychosis.
- Antidepressants:
- SSRIs (e.g., Citalopram, Sertraline) can treat co-morbid depression and anxiety.
- Trazodone is often used for insomnia with agitation due to its sedative effects.
⭐ Citalopram at doses > 20 mg/day in patients > 60 years old is associated with an increased risk of QT prolongation.
High-Yield Points - ⚡ Biggest Takeaways
- Non-pharmacologic interventions are first-line for managing behavioral symptoms in dementia.
- Always investigate for underlying triggers like pain, infection (e.g., UTI), or medication side effects before starting medications.
- Atypical antipsychotics are used for severe agitation but carry a black box warning for increased mortality in elderly patients.
- Avoid benzodiazepines due to the significant risk of worsening confusion, sedation, and falls.
- Caregiver education and support are crucial for effective long-term management.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

