Cyclothymia - The Moody Blues

- A chronic, fluctuating mood disturbance considered a milder form of bipolar disorder.
- Clinical Criteria (DSM-5):
- Numerous periods with hypomanic and depressive symptoms for at least 2 years in adults (1 year in children/adolescents).
- Symptoms do not meet the full criteria for a hypomanic or major depressive episode.
- Symptomatic periods are present for at least half the time.
- The patient is not symptom-free for more than 2 months at a time.
⭐ High-Yield: Up to 15-50% of individuals with cyclothymia will eventually be diagnosed with Bipolar I or Bipolar II disorder.
- Management:
- Psychotherapy (CBT, DBT) is the cornerstone of treatment.
- Mood stabilizers (e.g., lithium, valproate) may be considered if there is significant functional impairment.
Diagnosis - The 2-Year Rule
- Core Duration (The "2s"): For ≥ 2 years (adults) or ≥ 1 year (children/adolescents), patient experiences numerous periods of mood disturbance.
- Symptom Persistence:
- Hypomanic & depressive symptoms are present for at least half the time during this period.
- Any symptom-free intervals last no longer than 2 consecutive months.
- Sub-threshold Nature: The symptoms cause clinically significant distress or impairment but have never met the full criteria for a major depressive, manic, or hypomanic episode.
⭐ High-Yield: A significant portion (15-50%) of patients with cyclothymia will eventually progress to a full Bipolar I or Bipolar II disorder diagnosis. Early recognition is key.
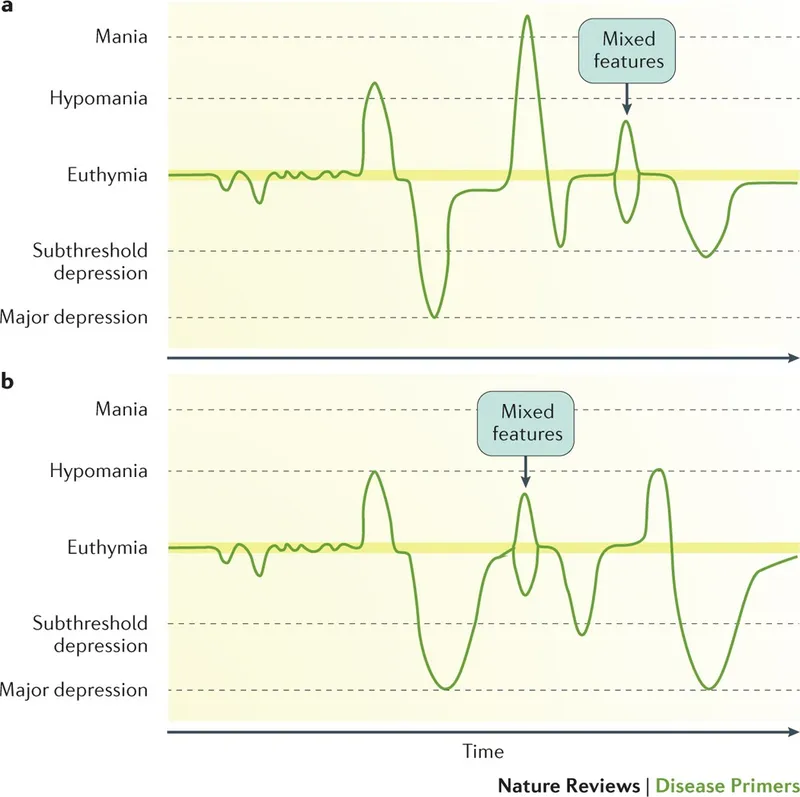
Differential Dx - The Lineup
- Bipolar I & II: Defined by at least one full manic (BPI) or hypomanic/major depressive (BPII) episode. Cyclothymia's highs and lows are less severe.
- Borderline Personality Disorder (BPD): Mood shifts are typically more rapid and reactive to interpersonal stressors, part of a pervasive pattern of instability.
⭐ In cyclothymia, symptoms are chronic but sub-threshold. They must be present for at least 2 years (1 year in children/adolescents), with symptoms present for at least half the time and never absent for more than 2 months at a time.
Management - Taming the Swings
- Psychotherapy is the cornerstone of treatment, focusing on education and coping skills.
- Cognitive Behavioral Therapy (CBT) helps identify and modify thought patterns.
- Psychoeducation and establishing regular routines (sleep, diet) are crucial.
- Pharmacotherapy is considered if functional impairment is severe or psychotherapy is insufficient.
⭐ Antidepressant monotherapy is generally avoided due to the risk of inducing hypomania or rapid cycling. If necessary, they should be used cautiously with a primary mood stabilizer.
High‑Yield Points - ⚡ Biggest Takeaways
- A chronic, fluctuating mood disturbance for at least 2 years (1 year in children/adolescents).
- Numerous periods with hypomanic symptoms and periods with depressive symptoms that do not meet full criteria for an episode.
- The patient is not symptom-free for more than 2 months at a time.
- Considered a milder form of bipolar disorder; high risk of progressing to Bipolar I or II.
- Must cause clinically significant distress or impairment.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

