Diagnosis & Epidemiology - Worry Wart Central
- DSM-5 Criteria: Excessive, uncontrollable worry about various topics, occurring more days than not for ≥6 months.
- Requires ≥3 of the following symptoms (only 1 for children):
- Restlessness or feeling on edge
- Easily fatigued
- Difficulty concentrating
- Irritability
- Muscle tension
- Sleep disturbance
- Epidemiology: Lifetime prevalence ~9%. More common in women (2:1 ratio).
⭐ High-Yield: GAD has a very high comorbidity with other psychiatric disorders, especially Major Depressive Disorder.

Pathophysiology - Brain on Overdrive
- Core Dysregulation: Overactive "anxiety circuit" involving key brain regions.
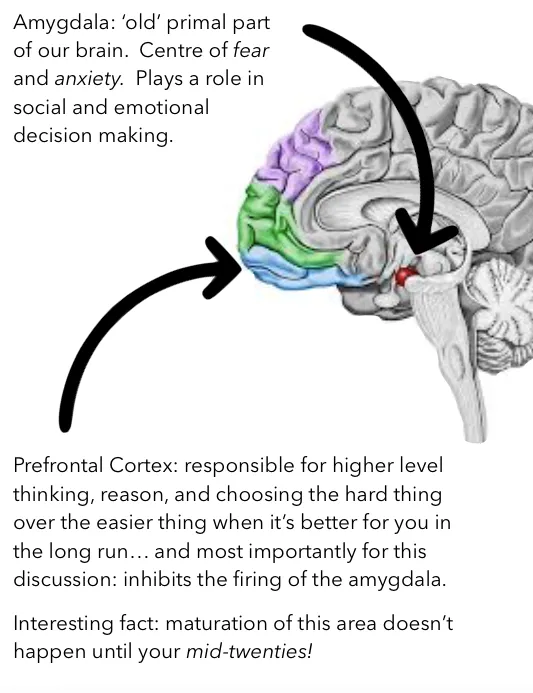
- ↑ Amygdala Activity: The brain's "fear center" is hyper-responsive to perceived threats, driving fear.
- ↓ Prefrontal Cortex (PFC) Control: Ineffective top-down inhibition of the amygdala, leading to uncontrollable worry.
- Neurotransmitter Imbalance:
- Serotonin & GABA: Dysregulation, particularly ↓ inhibitory GABAergic tone.
- Norepinephrine: ↑ levels contribute to autonomic symptoms like palpitations and restlessness.
⭐ The bed nucleus of the stria terminalis (BNST) mediates the sustained, anticipatory anxiety of GAD, distinct from the amygdala's role in acute fear.
Clinical Presentation & Workup - The Daily Grind
- Hallmark: Pervasive, difficult-to-control anxiety and worry about multiple domains (e.g., work, health), lasting ≥6 months.
- Associated with ≥3 of the following symptoms:
- Restlessness or feeling "on edge"
- Easy fatigability
- Difficulty concentrating
- Irritability
- Muscle tension
- Sleep disturbance
- Workup:
- Primarily a clinical diagnosis.
- Rule out organic causes (hyperthyroidism, substance use) with TSH & urine toxicology.
- GAD-7 scale helps quantify severity.
⭐ High comorbidity with Major Depressive Disorder is the rule, not the exception; always screen for depression and suicidality.
Differential Diagnosis - Is It Just Worry?
- Medical Conditions: Always rule out organic causes.
- Hyperthyroidism (check TSH), pheochromocytoma, hypoglycemia, arrhythmias.
- Substance-Induced:
- Intoxication: Caffeine, stimulants (amphetamines, cocaine).
- Withdrawal: Alcohol, benzodiazepines, barbiturates.
- Other Psychiatric Disorders:
- Panic Disorder: Worry is focused on future panic attacks.
- Social Anxiety Disorder: Worry is specific to social situations.
- MDD: Overlapping worry/rumination; assess for core depressive sx.
⭐ GAD involves excessive worry about real-life circumstances (finances, health), whereas OCD features ego-dystonic obsessions that are often bizarre or irrational.
Management - Taming the Worry Dragon
- First-Line: SSRIs (e.g., Sertraline) or SNRIs (e.g., Venlafaxine) are initial pharmacotherapy. Cognitive Behavioral Therapy (CBT) is equally first-line.
- Allow 4-6 weeks for antidepressant efficacy.
- Benzodiazepines can bridge severe, acute symptoms (⚠️ high dependence risk).
- Second-Line: Switch to a different SSRI/SNRI, or augment with buspirone.
⭐ Cognitive Behavioral Therapy (CBT) demonstrates efficacy comparable to pharmacotherapy and provides durable, long-lasting skills, making it a cornerstone of GAD management.
High-Yield Points - ⚡ Biggest Takeaways
- Chronic, excessive worry about multiple life domains, occurring more days than not for at least 6 months.
- Must have ≥3 associated symptoms: restlessness, fatigue, difficulty concentrating, irritability, muscle tension, or sleep disturbance.
- First-line treatment includes SSRIs (e.g., sertraline) or SNRIs (e.g., venlafaxine), often combined with psychotherapy.
- Cognitive Behavioral Therapy (CBT) is the most effective non-pharmacologic treatment.
- High comorbidity with major depressive disorder.
- Always rule out underlying medical causes (e.g., hyperthyroidism) and substance use.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

