V/Q Fundamentals - The Lung's Air-Blood Duet
- Ventilation (V): The volume of gas reaching the alveoli per minute.
- Normal alveolar ventilation ≈ 4 L/min.
- Perfusion (Q): The volume of blood flowing through pulmonary capillaries per minute.
- Normal pulmonary blood flow ≈ 5 L/min.
- V/Q Ratio: The ratio of alveolar ventilation to pulmonary blood flow, ideally matched for optimal gas exchange.
- Normal overall V/Q ratio is $4/5$ = 0.8.
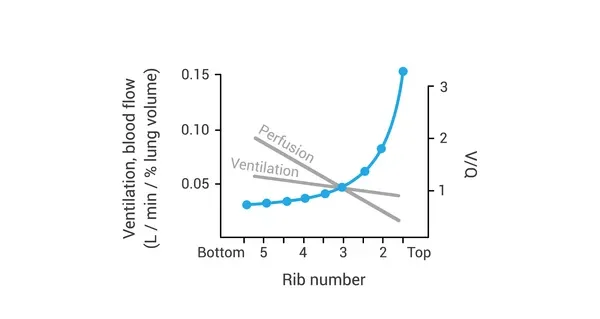
⭐ Both ventilation and perfusion are highest at the lung bases (due to gravity), but perfusion's increase is more pronounced than ventilation's. This variation creates a physiological V/Q gradient from apex to base.
Normal V/Q Gradient - Gravity's Influence
In an upright lung, gravity pulls both air (ventilation) and blood (perfusion) downwards, but its effect on blood is far greater. This creates a physiological gradient from the apex to the base.
- Apex (Top of Lung):
- Ventilation (V) is lower.
- Perfusion (Q) is much lower.
- Result: High V/Q ratio (e.g., >3.0), creating physiologic dead space.
- Base (Bottom of Lung):
- Ventilation (V) is higher.
- Perfusion (Q) is much higher.
- Result: Low V/Q ratio (e.g., 0.6), creating a physiologic shunt.
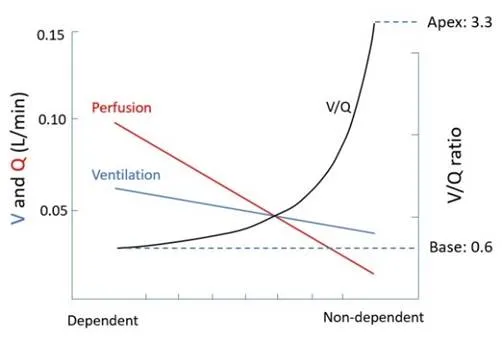
⭐ Both ventilation and perfusion are lowest at the apex and highest at the base. The key is that the gradient for perfusion is much steeper than for ventilation.
- The average V/Q for the entire lung is ~0.8.
Gas Exchange Effects - The Apex-to-Base Shift
-
Apex (High V/Q > 1): "Wasted Ventilation"
- Ventilation exceeds perfusion, creating physiologic dead space.
- Alveolar gas has high $O_2$ and low $CO_2$.
- Blood leaving the apex has ↑ $PaO_2$ (
130 mmHg) & ↓ $PaCO_2$ (28 mmHg).
-
Base (Low V/Q < 1): "Physiologic Shunt"
- Perfusion exceeds ventilation.
- Alveolar gas has lower $O_2$ and higher $CO_2$.
- Blood leaving the base has ↓ $PaO_2$ (
90 mmHg) & ↑ $PaCO_2$ (42 mmHg).
-
Net Result:
- Mixing of blood from all lung zones results in systemic arterial values of $PaO_2$ ≈ 100 mmHg and $PaCO_2$ ≈ 40 mmHg.
⭐ Because blood flow is much higher at the base, the overall composition of systemic arterial blood more closely resembles that of the blood leaving the base.
High‑Yield Points - ⚡ Biggest Takeaways
- Both ventilation (V) and perfusion (Q) are gravity-dependent, increasing from the apex to the base of the lung.
- The change in perfusion is more dramatic than the change in ventilation down the lung.
- The apex has a high V/Q ratio (e.g., >3), creating physiologic dead space with high PAO₂.
- The base has a low V/Q ratio (e.g., <0.6), creating a physiologic shunt with low PAO₂.
- The average V/Q ratio for the entire lung is approximately 0.8.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

