Sleep Stages - A Dreamy Descent
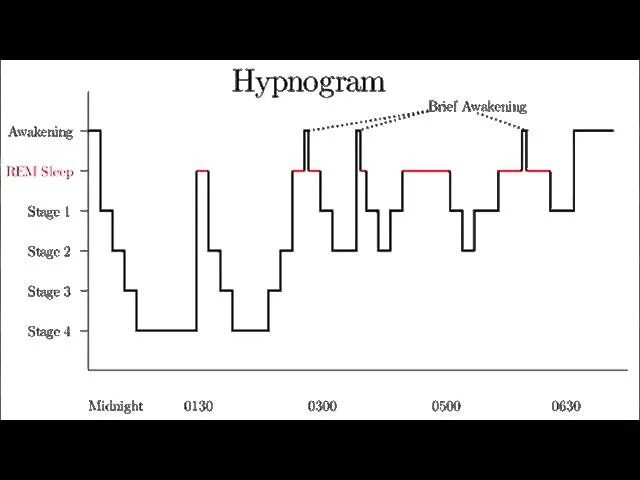
- Sleep Architecture: The predictable cycling between NREM and REM sleep stages, typically 4-5 cycles per night. Visualized on a hypnogram.
- NREM (Non-Rapid Eye Movement) Sleep: Constitutes 75-80% of total sleep.
- N1: Transition to sleep; light sleep.
- N2: Majority of sleep time; features sleep spindles and K-complexes.
- N3: Slow-wave sleep (SWS); deepest, most restorative stage.
- REM (Rapid Eye Movement) Sleep: Makes up 20-25% of sleep; associated with dreaming.
⭐ REM sleep is characterized by muscle atonia, which includes most accessory muscles of respiration, making breathing predominantly diaphragmatic.
Physiological Changes - The Sleeping Lung
Overall, minute ventilation ($V_E = V_t \times RR$) decreases during sleep. The pattern of breathing and chemoreceptor sensitivity varies significantly between NREM and REM stages, impacting gas exchange.
| Parameter | Wakefulness | NREM Sleep | REM Sleep |
|---|---|---|---|
| Minute Ventilation ($V_E$) | Normal | ↓ (stable) | ↓↓ (irregular) |
| Tidal Volume ($V_t$) | Normal | ↓ | ↓↓ |
| Respiratory Rate (RR) | Normal | Regular | Irregular/Variable |
| Hypercapnic Drive | Normal | ↓ | ↓↓ (blunted) |
| Hypoxic Drive | Normal | ↓ | ↓↓ (blunted) |
| Upper Airway Resistance | Normal | ↑ | ↑↑ (variable) |
- Upper airway muscle (e.g., genioglossus) tone ↓, leading to ↑ resistance.
- REM sleep features atonia of intercostal muscles, making breathing diaphragm-dependent.
⭐ The ventilatory response to both hypoxia and hypercapnia is most significantly blunted during REM sleep, increasing the risk of desaturation.
Sleep Apnea - When Breathing Stops
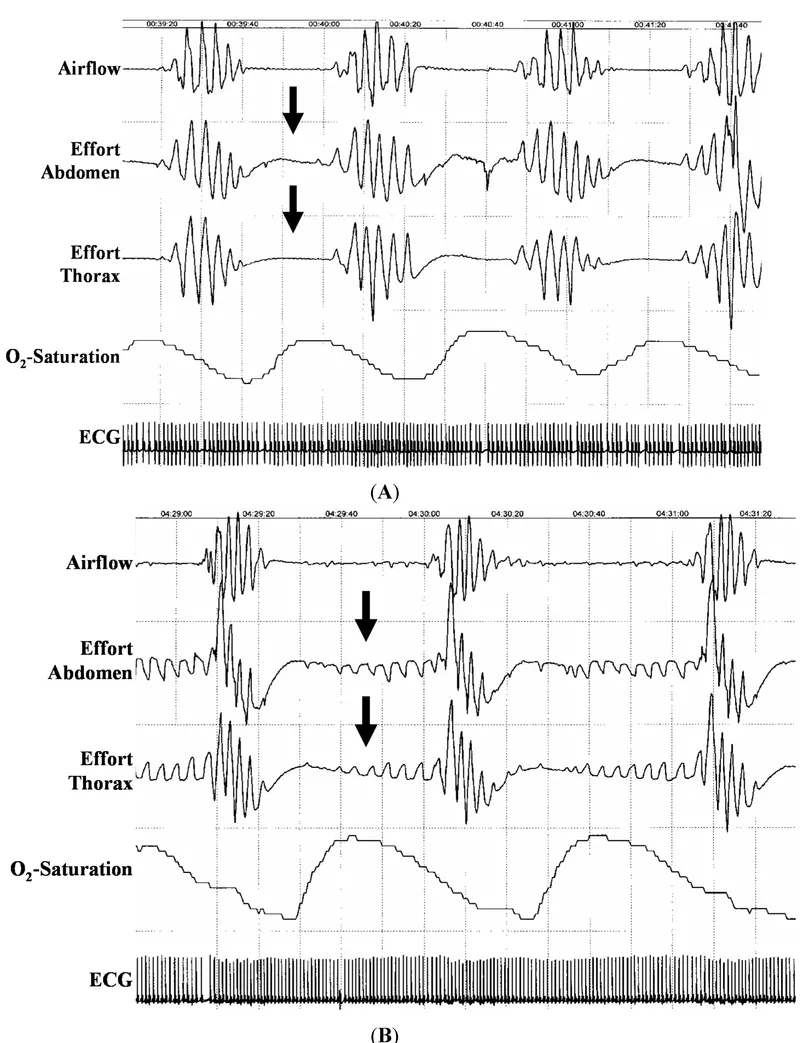
Recurrent episodes of apnea (cessation of airflow) or hypopnea (reduced airflow) during sleep, leading to oxygen desaturation.
- Obstructive Sleep Apnea (OSA): Most common type. Characterized by upper airway collapse despite persistent respiratory effort.
- Central Sleep Apnea (CSA): Defined by the absence of respiratory effort, stemming from reduced central nervous system drive.
- Diagnosis: Polysomnography measures the Apnea-Hypopnea Index (AHI).
- AHI Severity: Mild 5-15, Moderate 15-30, Severe >30 events/hour.
⭐ In OSA, there is continued (often exaggerated) respiratory effort against an obstructed upper airway, whereas in CSA, both airflow and respiratory effort cease.
📌 Mnemonic: For OSA think 'Obstruction': Effort Present, Airflow Absent.
Clinical Correlates - The Zzz-Sleuth
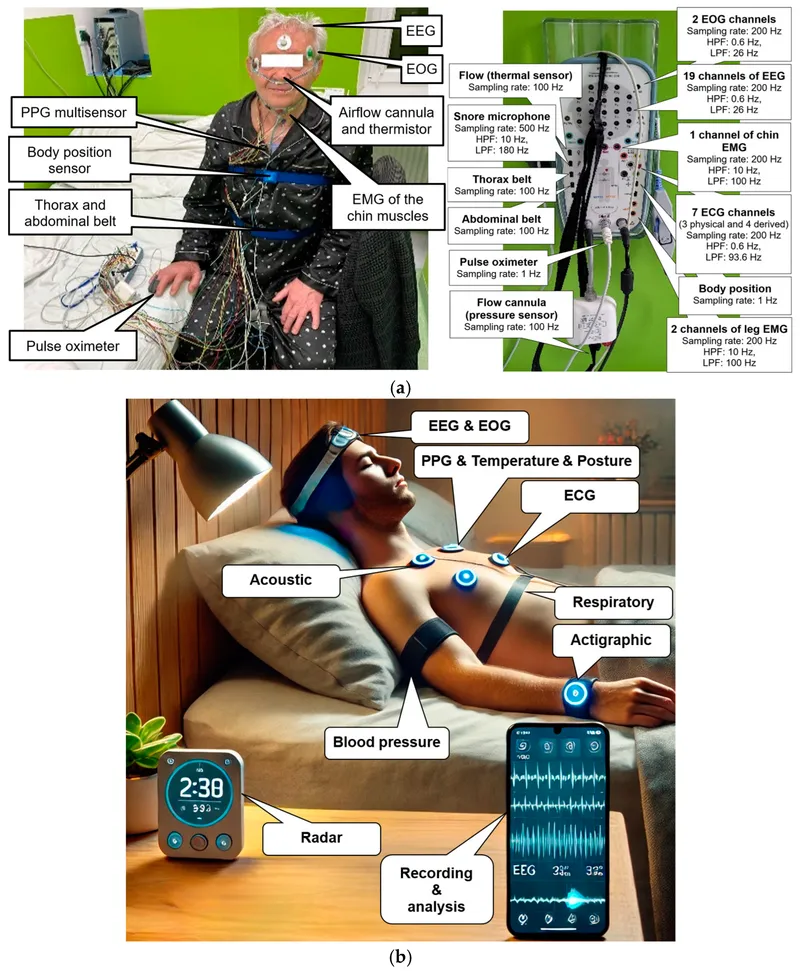
- Polysomnography (PSG): The definitive diagnostic test for sleep-related breathing disorders.
- Integrates multiple measurements:
- Electroencephalogram (EEG): Brain waves (sleep staging).
- Electrooculogram (EOG): Eye movements (REM sleep).
- Electromyogram (EMG): Muscle tone (atonia in REM).
- Respiratory airflow/effort & O₂ saturation.
- Integrates multiple measurements:
- Epworth Sleepiness Scale: A questionnaire to quantify daytime sleepiness; a score >10 is considered sleepy.
- Management:
- CPAP (Continuous Positive Airway Pressure): Provides constant pressure to keep the airway open.
- BiPAP (Bilevel Positive Airway Pressure): Delivers higher pressure on inhalation and lower pressure on exhalation.
⭐ Polysomnography is the gold standard for diagnosing sleep-related breathing disorders, as it simultaneously measures brain waves (sleep stage), eye movements, muscle activity, respiratory airflow/effort, and oxygen saturation.
High-Yield Points - ⚡ Biggest Takeaways
- During NREM sleep, minute ventilation ↓ due to reduced metabolic rate and chemosensitivity.
- REM sleep brings irregular, shallow breathing and profound muscle atonia, especially of the upper airway, increasing collapse risk.
- Ventilatory responses to hypoxia and hypercapnia are significantly blunted, most severely in REM.
- Sleep induces a state of relative hypoventilation, causing a physiological ↑ in PaCO2.
- Upper airway resistance increases during all sleep stages.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

