Formation & Structure - The Yellow Body
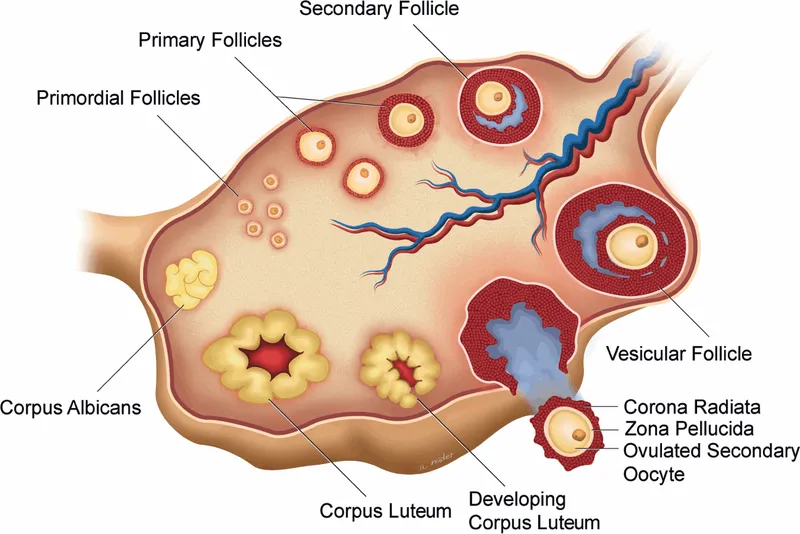
- Post-ovulation transformation: The remnants of the ovarian follicle form the corpus luteum (CL).
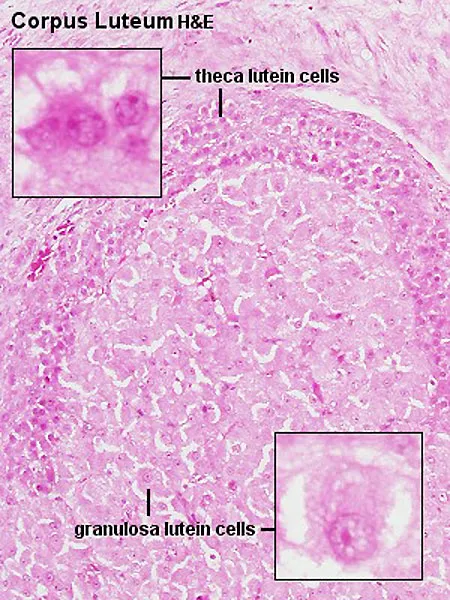
- Luteinization: Triggered by the LH surge, granulosa and theca interna cells hypertrophy, accumulating a yellow pigment (lutein), giving it its name-"yellow body."
- Granulosa lutein cells: Produce progesterone.
- Theca lutein cells: Produce androgens & progesterone.
- Highly vascularized: Essential for hormone transport.
⭐ The LH surge is the critical trigger for both ovulation and the subsequent luteinization of follicular cells into the corpus luteum.
Hormonal Hub - Progesterone Power
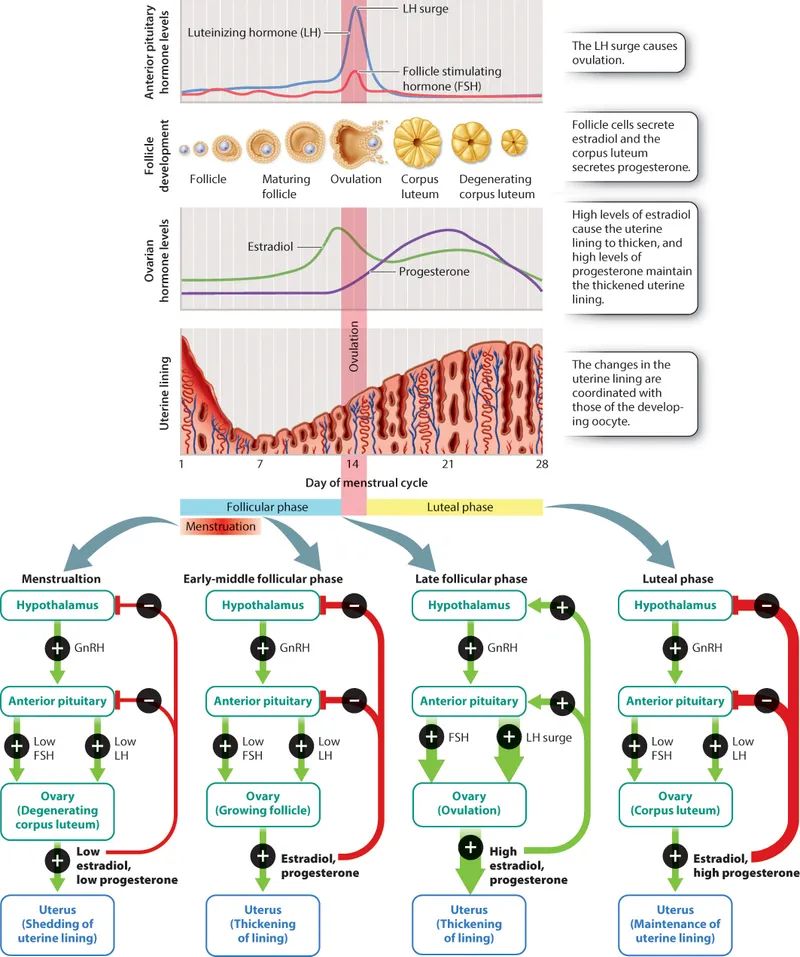
- Primary Role: Luteal phase engine, primarily producing progesterone. Also secretes inhibin A and some estrogen.
- Progesterone's Core Functions:
- Uterine Preparation: Converts endometrium to a secretory state, ready for implantation. ↑ glycogen, ↑ spiral artery growth.
- Pregnancy Maintenance: Relaxes myometrium (prevents contractions) and thickens cervical mucus (forms a protective plug).
- HPA Axis Suppression: Provides negative feedback to the hypothalamus and pituitary, ↓ GnRH, FSH, and LH. This prevents new follicle development.
⭐ The Luteal-Placental Shift: The corpus luteum is critical for maintaining pregnancy for the first 8-10 weeks by producing progesterone. After this period, the placenta becomes the primary source. Failure of this shift can result in miscarriage.
Fate of the Luteum - Live or Let Die
- The corpus luteum has two potential fates, determined by the presence or absence of fertilization.
1. No Fertilization (Luteolysis)
- If no fertilization occurs, the corpus luteum has a fixed lifespan of ~14 days.
- It degenerates into a fibrous scar tissue called the corpus albicans.
- This leads to a sharp ↓ in progesterone and estrogen, triggering endometrial breakdown and menstruation.
2. Fertilization Occurs (Luteal Rescue)
- The syncytiotrophoblast of the implanting blastocyst secretes human chorionic gonadotropin (hCG).
- hCG, an analog of LH, "rescues" the corpus luteum, which becomes the corpus luteum of pregnancy.
⭐ The corpus luteum is critical for progesterone production until the 8-10th week of gestation, when the placenta takes over this function (luteal-placental shift).
Clinical Correlations - Luteal Phase Lows
- Luteal Phase Defect (LPD):
- Corpus luteum produces insufficient progesterone (↓ P4).
- Results in a shortened luteal phase (< 12 days).
- Causes inadequate endometrial maturation for implantation.
- Clinically presents as infertility or recurrent early pregnancy loss.
- Premenstrual Syndrome (PMS) / PMDD:
- Symptoms arise in the luteal phase due to hormonal shifts.
- Not caused by abnormal hormone levels, but rather an abnormal response to normal levels.
- PMDD is a severe form causing significant distress.
⭐ Luteal phase support with progesterone is a common intervention in assisted reproductive technology (ART) cycles to ensure endometrial receptivity.
High‑Yield Points - ⚡ Biggest Takeaways
- The corpus luteum forms from remnant granulosa and theca cells post-ovulation.
- Its primary role is secreting progesterone, which maintains the secretory endometrium for implantation.
- If fertilization occurs, hCG "rescues" the corpus luteum, sustaining progesterone output.
- Without pregnancy, it degenerates into the corpus albicans in 10-14 days.
- This subsequent progesterone withdrawal triggers menstruation.
- The placenta assumes progesterone production by weeks 8-10 of gestation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

