Glomerular Filtration - The Kidney's Sieve
- Function: Ultrafiltration of blood to produce a protein-free filtrate. Normal GFR ≈ 125 mL/min or 180 L/day.
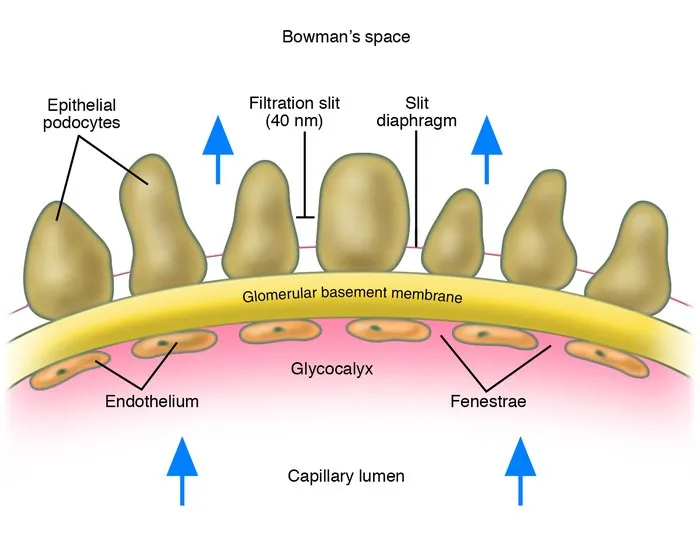
- Filtration Barrier (Size & Charge Selectivity):
- Fenestrated Capillary Endothelium: Blocks cells.
- Glomerular Basement Membrane (GBM): Fused basal laminae with negative charge (heparan sulfate) repels albumin.
- Podocyte Foot Processes: Slit diaphragms form the final barrier.
- Starling Forces: GFR is governed by hydrostatic and oncotic pressure gradients. $P_{GC}$ (Glomerular Capillary Hydrostatic Pressure) is the main driver.
⭐ Loss of the GBM's negative charge (e.g., Minimal Change Disease) causes selective albuminuria, even without major structural changes on light microscopy.
Proximal Tubule - The Bulk Reabsorber
- Workhorse of the nephron; reabsorbs ~65-80% of filtered solutes and water.
- Fluid leaving is isotonic to plasma (~300 mOsm/L).
Key Functions:
- Reabsorption: All glucose & amino acids; most $Na^+$, $Cl^-$, $K^+$, $H_2O$, and $HCO_3^-$.
- $HCO_3^-$ reabsorption depends on carbonic anhydrase.
- Secretion: $H^+$, $NH_4^+$, organic acids (PAH, urate), and bases (creatinine).
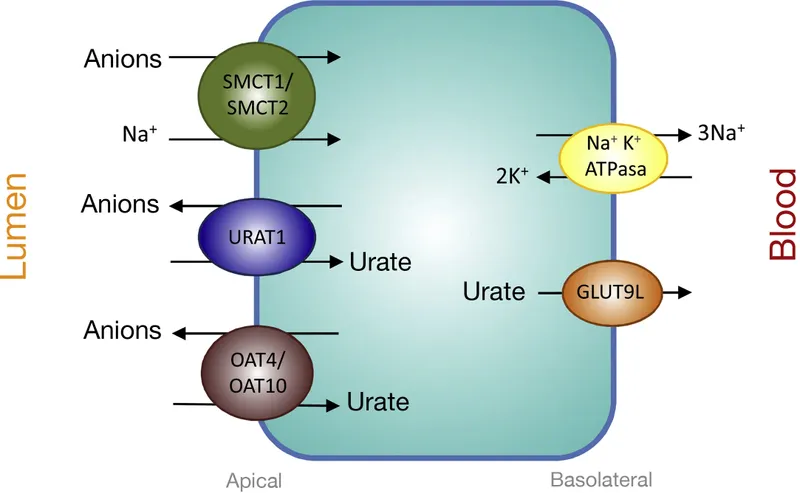
⭐ High-Yield: Parathyroid hormone (PTH) inhibits the $Na^+/PO_4^{3-}$ cotransporter, causing phosphate excretion (phosphaturia). Carbonic anhydrase inhibitors (e.g., acetazolamide) act here, causing $HCO_3^-$ wasting.
Loop of Henle - Salty Medulla Maker
- Primary Function: Establishes a hypertonic medullary interstitium via countercurrent multiplication, crucial for concentrating urine.
- Descending Limb:
- Highly permeable to H₂O, impermeable to NaCl.
- H₂O passively flows out into the salty medulla.
- Tubular fluid osmolarity ↑.
- Ascending Limb:
- Impermeable to H₂O.
- Thin Ascending: Passive NaCl reabsorption.
- Thick Ascending Limb (TAL): Actively reabsorbs NaCl via the Na-K-2Cl (NKCC) cotransporter. This is the engine of the system.
- Tubular fluid becomes dilute (hypotonic).
- Vasa Recta: Countercurrent exchange prevents washout of the medullary gradient.
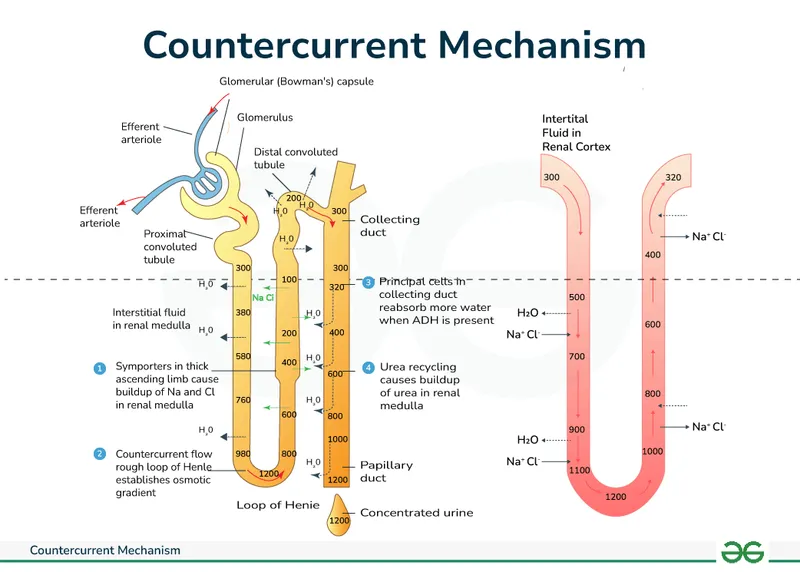
⭐ The Thick Ascending Limb's Na-K-2Cl (NKCC) cotransporter is the target for loop diuretics (e.g., Furosemide). Inhibition leads to potent diuresis by disrupting the medullary gradient.
Distal Nephron - Hormonal Fine-Tuning
The final, precise regulation of urine composition, primarily influenced by aldosterone and ADH to manage electrolyte and water balance.
-
Principal Cells: Major site of Na⁺/K⁺/H₂O regulation.
- Aldosterone: Binds mineralocorticoid receptor → upregulates basolateral Na⁺/K⁺-ATPase and apical channels (ENaC, ROMK) → ↑Na⁺ reabsorption, ↑K⁺ secretion.
- ADH (Vasopressin): Binds V2 receptor (Gs) → ↑cAMP → PKA activation → insertion of AQP2 channels into apical membrane → ↑H₂O reabsorption.
-
Intercalated Cells: Manage acid-base balance.
- α-cells: Secrete H⁺ via H⁺-ATPase.
- β-cells: Secrete HCO₃⁻.
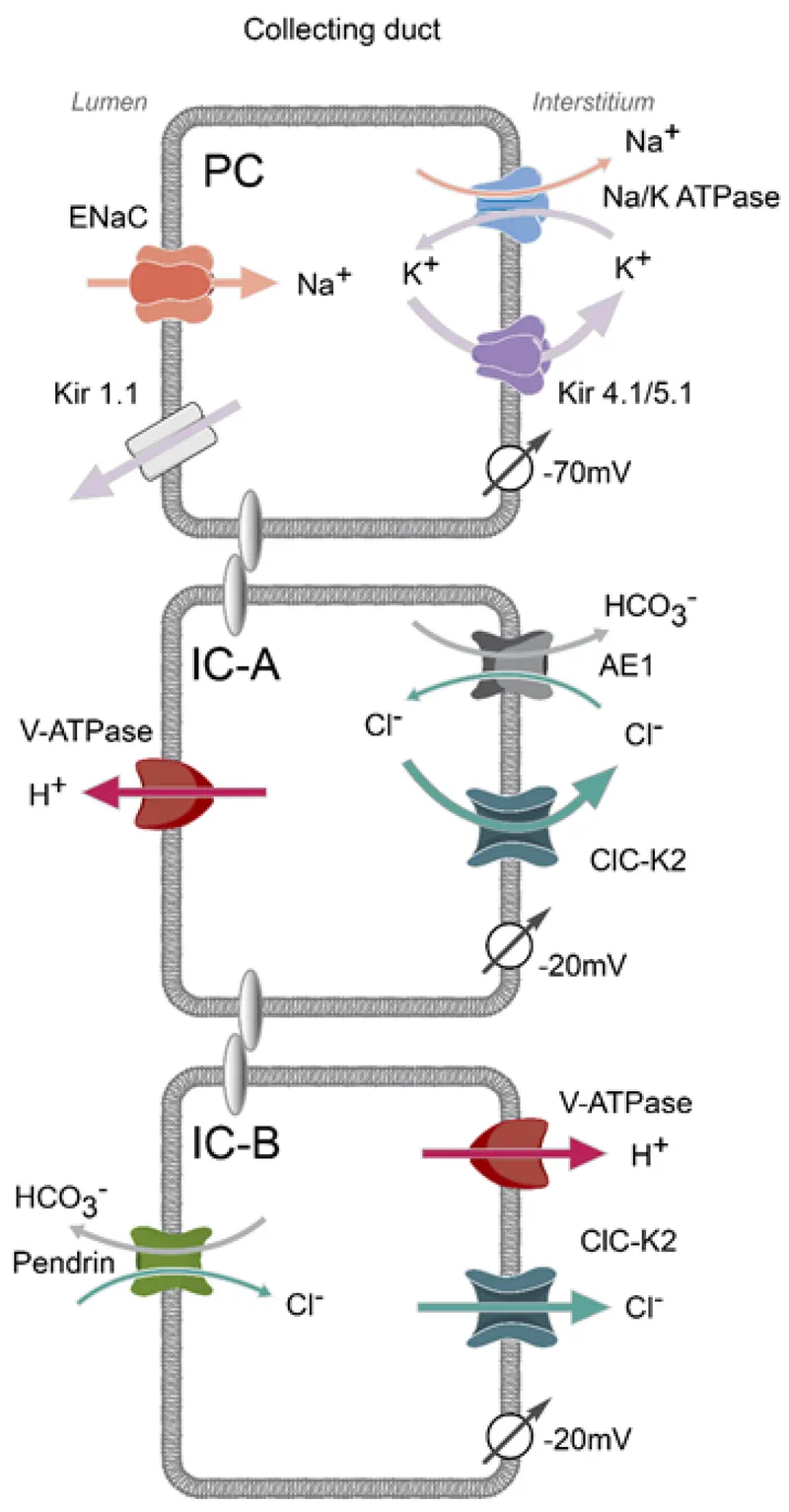
⭐ K⁺-Sparing Diuretics: Amiloride and triamterene directly block the ENaC channel. Spironolactone and eplerenone are competitive aldosterone antagonists, preventing its nuclear action. Both mechanisms reduce Na⁺ reabsorption and K⁺ secretion.
High‑Yield Points - ⚡ Biggest Takeaways
- Aldosterone (acting on the DCT/CD) and ADH (acting on the CD) are the principal regulators of volume and osmolarity.
- The PCT is the bulk reabsorber: nearly all glucose/amino acids and ~65% of Na+ and H₂O.
- The Loop of Henle generates the medullary gradient via countercurrent multiplication, essential for concentrating urine.
- The DCT fine-tunes electrolytes: Aldosterone reabsorbs Na+, while PTH reabsorbs Ca²⁺.
- The Collecting Duct controls final urine concentration via ADH-regulated aquaporins.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

