RAAS Dysregulation - The Vicious Cycle
In states like heart failure or cirrhosis, RAAS activation becomes maladaptive, creating a harmful feedback loop.
- Heart Failure: ↓ Cardiac output triggers RAAS, but resulting ↑ afterload/preload further strains the failing heart.
- Cirrhosis & Nephrotic Syndrome: ↓ Effective circulating volume activates RAAS, leading to volume overload (ascites, edema) that worsens the condition.
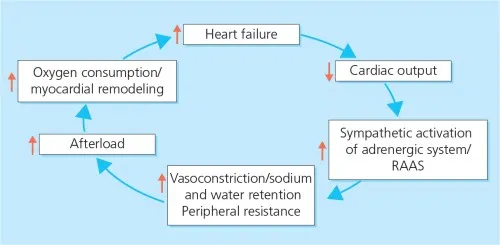
⭐ Angiotensin II directly promotes maladaptive cardiac remodeling (fibrosis, hypertrophy), a key factor in the progression of heart failure. This is a primary target of ACE inhibitors and ARBs.
Heart Failure - The Failing Pump's Cry
- Trigger: ↓ Cardiac Output (CO) from a failing heart leads to ↓ renal perfusion pressure.
- RAAS Activation: Kidneys release renin, activating the RAAS cascade.
- Vicious Cycle:
- Angiotensin II → potent vasoconstriction (↑ afterload).
- Aldosterone → Na⁺ & water retention (↑ preload).
- Both actions increase the workload on an already strained heart, worsening failure.
⭐ Maladaptive Remodeling: Initially compensatory, chronic RAAS activation is detrimental. It promotes myocardial fibrosis and hypertrophy, contributing to the progressive decline of cardiac function.
Hypertension & Renal Artery Stenosis - The Pressure Cooker
-
Pathophysiology: Stenosis → ↓ renal blood flow → affected kidney perceives systemic hypotension.
- RAAS Activation: Juxtaglomerular apparatus (JGA) hyper-secretes renin → ↑ Angiotensin II & ↑ Aldosterone.
- Consequences: Systemic vasoconstriction, plus Na⁺ and H₂O retention, leads to severe secondary hypertension.
-
Key Etiologies:
- Atherosclerosis: Most common cause, typically in older males at the renal artery ostium.
- Fibromuscular Dysplasia (FMD): Affects younger women; classic "string of beads" appearance on angiography.
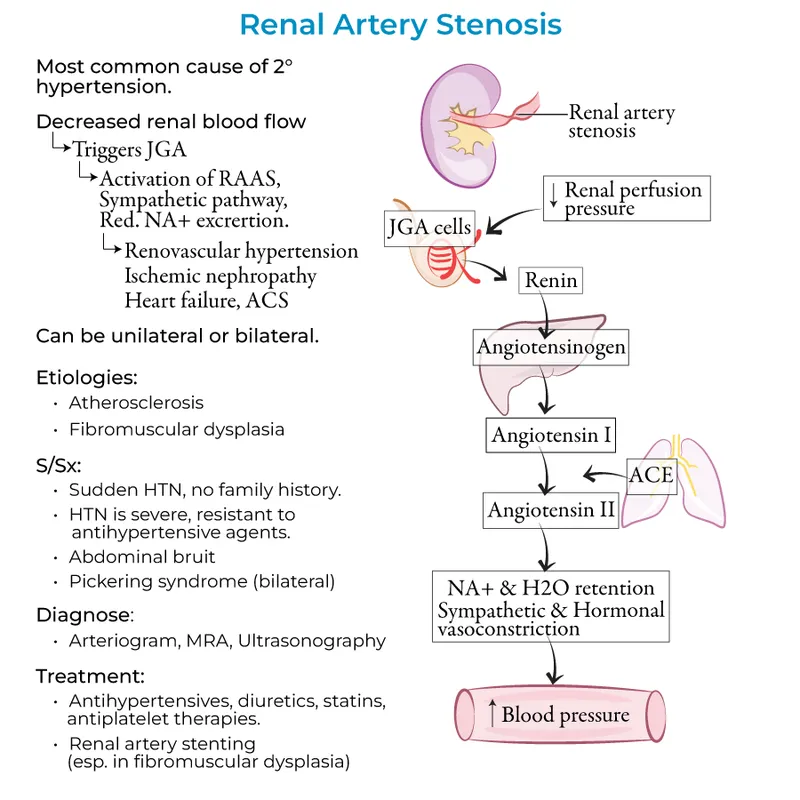
⭐ In unilateral RAS, the contralateral (unaffected) kidney undergoes pressure natriuresis, which helps to limit volume expansion. This compensatory mechanism is absent in bilateral stenosis.
RAAS Pharmacology - Taming the Beast
-
Goal: Disrupt the RAAS cascade to ↓ blood pressure & ↓ aldosterone effects.
-
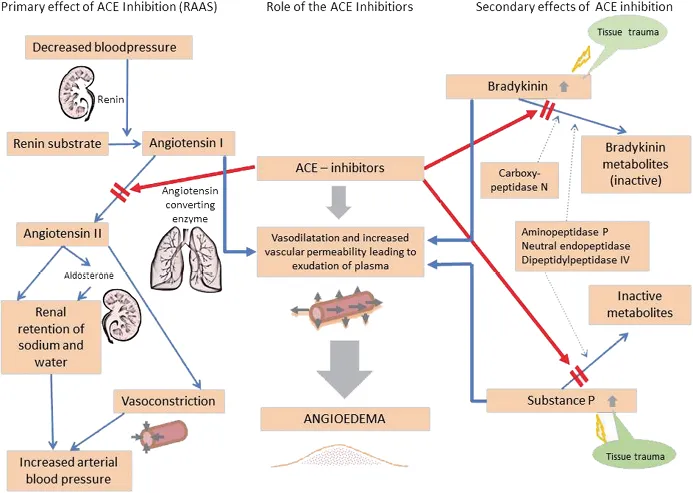
ACE Inhibitors (-prils): Inhibit ACE → ↓ Ang II & ↑ Bradykinin.
- Side Effects: Dry cough, angioedema (due to bradykinin), hyperkalemia.
-
ARBs (-sartans): Selectively block AT1 receptors.
- Side Effects: Hyperkalemia. No cough/angioedema vs. ACEi.
-
Aldosterone Antagonists (MRAs): Block aldosterone receptors in the collecting duct.
- Side Effects: Hyperkalemia. Spironolactone can cause gynecomastia.
⭐ Triple Whammy Effect: Concurrent use of an ACEi/ARB + Diuretic + NSAID significantly increases the risk of acute kidney injury (AKI). NSAIDs constrict the afferent arteriole, reducing GFR in a kidney already compromised by RAAS inhibition and volume depletion.
⚠️ All RAAS inhibitors are teratogenic.
High‑Yield Points - ⚡ Biggest Takeaways
- In heart failure, ↓ cardiac output activates RAAS, leading to deleterious fluid retention and vasoconstriction.
- Renal artery stenosis causes profound RAAS activation, leading to secondary hyperaldosteronism and treatment-resistant hypertension.
- ACE inhibitors and ARBs are crucial in these states; they counter-regulate maladaptive RAAS effects.
- Primary hyperaldosteronism (Conn's syndrome) is a state of high aldosterone but low renin.
- Chronic RAAS activation contributes to end-organ damage like cardiac remodeling and renal fibrosis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

