Physiology - The Body's Rebound
- Trigger: Transitioning to an upright posture (e.g., standing).
- Initial Effect: Gravitational pooling of ~500-700 mL of blood in lower extremity veins.
- Cascade: This ↓ venous return (preload), leading to ↓ cardiac output and a transient ↓ in mean arterial pressure ($MAP$).
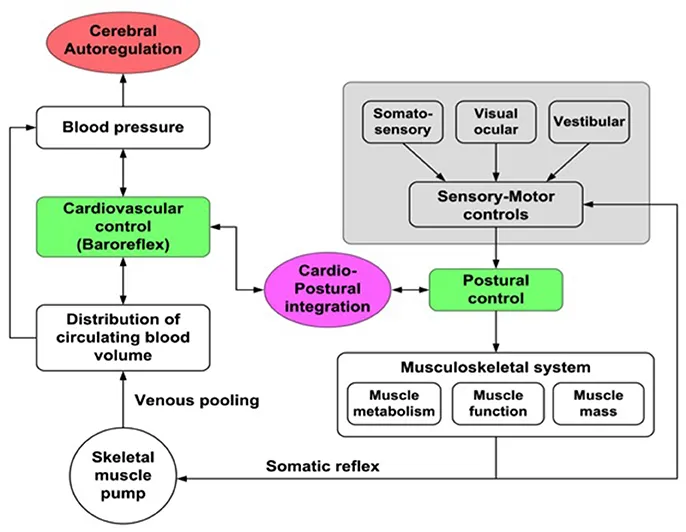
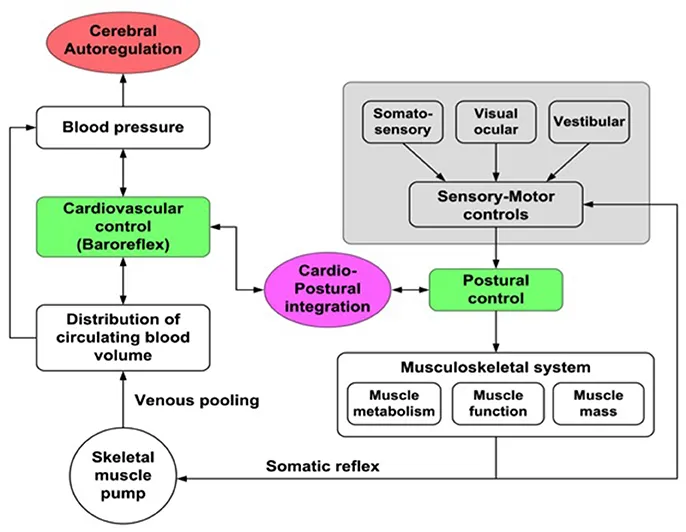
- Response (Baroreflex): Aortic and carotid baroreceptors detect the ↓ $MAP$, triggering a rapid autonomic response:
- ↑ Sympathetic outflow & ↓ parasympathetic outflow.
- Leads to ↑ heart rate, ↑ contractility, and systemic vasoconstriction (↑ TPR).
- This compensates for the initial drop, restoring blood pressure and cerebral perfusion.
⭐ Orthostatic Hypotension: Defined as a sustained reduction in systolic blood pressure of at least 20 mmHg or a reduction in diastolic blood pressure of 10 mmHg within 3 minutes of standing.
Pathophysiology - When Gravity Wins
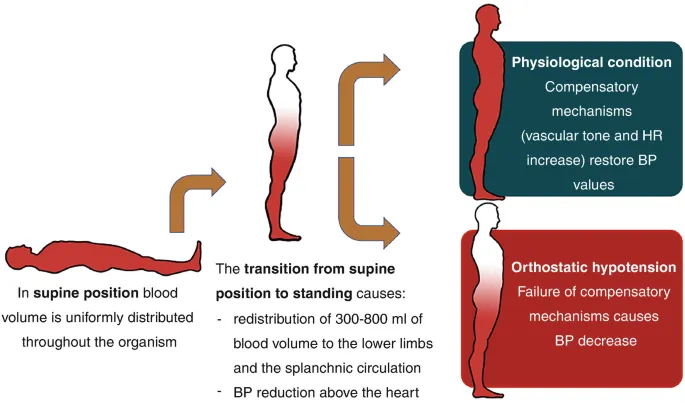
- Upon standing, gravity pulls ~500-1000 mL of blood into the compliant lower-body venous system.
- This ↓ venous return to the heart, leading to a transient drop in cardiac output (CO) and mean arterial pressure (MAP).
- The primary compensatory response is the baroreceptor reflex.
⭐ Orthostatic hypotension occurs when this reflex fails, defined by a sustained reduction in systolic blood pressure of at least 20 mmHg or a reduction in diastolic blood pressure of 10 mmHg within three minutes of standing.
Diagnosis - Spotting the Drop
- Core Criteria: Diagnosis confirmed with a bedside orthostatic vitals test.
- Measure blood pressure and heart rate in the supine position after 5 minutes of rest.
- Have the patient stand up.
- Repeat measurements at 1 and 3 minutes.
- Positive Test: Within 3 minutes of standing:
- Systolic BP drop ≥ 20 mmHg
- Diastolic BP drop ≥ 10 mmHg
- Symptoms of cerebral hypoperfusion (e.g., lightheadedness, dizziness).
⭐ A key diagnostic clue is the heart rate response. An insufficient heart rate increase (<15 bpm) despite hypotension suggests a neurogenic cause (autonomic failure).
Management - Staying Upright
-
Non-Pharmacologic (First-line):
- Physical counter-maneuvers (e.g., leg crossing, squatting, muscle tensing).
- Increase salt and water intake.
- Wear compression stockings or abdominal binders.
- Elevate head of bed.
-
Pharmacologic Options:
- Fludrocortisone (expands plasma volume).
- Midodrine or Droxidopa (vasoconstrictors).
⭐ Midodrine, an α1-agonist, carries a risk of supine hypertension. Counsel patients to take it while upright and avoid doses near bedtime.
High‑Yield Points - ⚡ Biggest Takeaways
- On standing, gravity pools blood in the lower body, causing a transient drop in venous return.
- This leads to decreased cardiac output and a fall in blood pressure.
- The baroreceptor reflex is the immediate compensatory response.
- It triggers increased sympathetic outflow, causing vasoconstriction and increased heart rate.
- Orthostatic hypotension results from a failure of this reflex.
- It's defined as a SBP drop of >20 mmHg or DBP drop of >10 mmHg within 3 minutes of standing.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

