Waveform Morphology - The Heart's Signature
- Anacrotic Limb (Systolic Upstroke): Rapid pressure ↑ from ventricular ejection. Its slope reflects myocardial contractility (inotropy).
- Systolic Peak: The highest pressure point, representing the peak force of left ventricular contraction.
- Dicrotic Notch: A small dip marking the closure of the aortic valve. It signals the end of systole.
- Diastolic Runoff: The gradual pressure decline as blood flows to the periphery. The slope is determined by Systemic Vascular Resistance (SVR).
⭐ The dicrotic notch is blunted or disappears in significant aortic regurgitation and in low-pressure states (e.g., septic shock).
Key Pressure Points - Numbers Game
- Systolic Pressure (SP): Peak pressure during cardiac contraction.
- Normal: <120 mmHg.
- Diastolic Pressure (DP): Lowest arterial pressure during cardiac relaxation.
- Normal: <80 mmHg.
- Pulse Pressure (PP): The difference between SP and DP; reflects stroke volume.
- Formula: $PP = SP - DP$
- Normal: ~40 mmHg.
- Widened in aortic regurgitation; narrowed in aortic stenosis.
- Mean Arterial Pressure (MAP): Average pressure driving tissue perfusion.
- Formula: $MAP \approx DP + \frac{1}{3}(PP)$
- Must be >60-65 mmHg for adequate organ perfusion.
⭐ The MAP formula weights diastole more heavily because at a normal heart rate, the diastolic phase lasts about twice as long as the systolic phase.
Physiological Factors - What Shapes the Wave
- Systolic Pressure (SP): Peak pressure during ventricular ejection. Primarily reflects the interplay between stroke volume and aortic compliance.
- ↑ Stroke Volume (SV) → ↑ SP
- ↓ Aortic Compliance → ↑ SP
- Diastolic Pressure (DP): Lowest pressure during ventricular relaxation. Primarily set by systemic vascular resistance (SVR).
- ↑ SVR → ↑ DP (less peripheral runoff)
- ↑ Heart Rate → ↑ DP (less diastolic time)
- Pulse Pressure (PP): The difference, $PP = SP - DP$.
- Proportional to SV; inversely proportional to compliance.
- Mean Arterial Pressure (MAP): Average pressure over a cardiac cycle.
- $MAP \approx DP + \frac{1}{3}PP$
⭐ In arteriosclerosis, decreased aortic compliance is the main driver of isolated systolic hypertension (↑ SP, normal DP), causing a widened pulse pressure. This is a key hemodynamic change in the elderly.
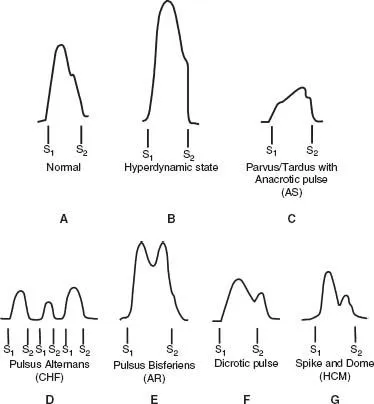
Pathological Waveforms - When Waves Go Wrong
- Aortic Stenosis: Pulsus parvus et tardus (weak and delayed upstroke). Results in a narrow pulse pressure (↓).
- Aortic Regurgitation: Pulsus bisferiens (biphasic pulse) and water-hammer pulse. Creates a wide pulse pressure (↑).
- Hypertrophic Cardiomyopathy (HOCM): Spike-and-dome pattern (bifid pulse) due to LV outflow tract obstruction.
⭐ Pulsus Paradoxus: An exaggerated drop (>10 mmHg) in systolic blood pressure during inspiration. It is a classic sign of cardiac tamponade.
High‑Yield Points - ⚡ Biggest Takeaways
- The arterial pressure waveform graphically represents pressure changes in an artery throughout the cardiac cycle.
- The systolic peak corresponds to maximum pressure during left ventricular ejection.
- The dicrotic notch (incisura) marks the closure of the aortic valve.
- Pulse pressure (Systolic − Diastolic) is directly proportional to stroke volume.
- Mean Arterial Pressure (MAP) is approximately Diastolic P + ⅓(Pulse P), critical for ensuring adequate tissue perfusion.
- A dampened, delayed upstroke (pulsus parvus et tardus) is a classic sign of aortic stenosis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

