Autoregulation - The Kidney's Balancing Act
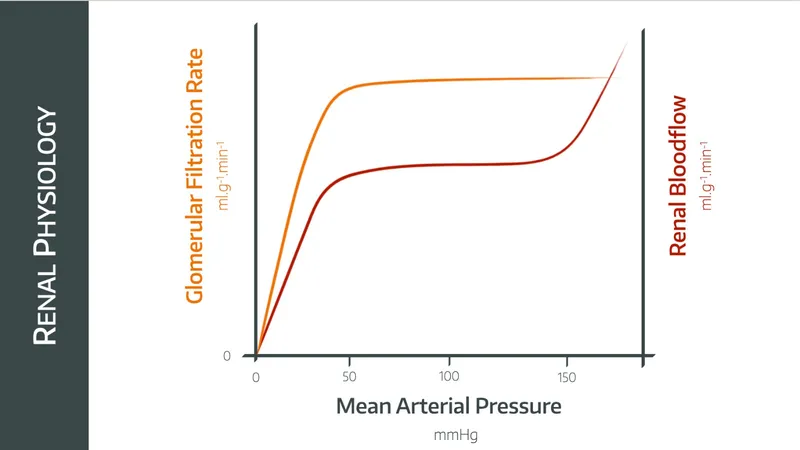
Maintains near-constant Glomerular Filtration Rate (GFR) and Renal Blood Flow (RBF) despite fluctuations in mean arterial pressure (MAP) between 80-180 mmHg.
- Myogenic Mechanism (Intrinsic):
- ↑ Systemic BP stretches afferent arterioles.
- Triggers smooth muscle contraction (vasoconstriction).
- Normalizes downstream blood flow and GFR.
- Tubuloglomerular Feedback (TGF):
- Macula densa cells sense ↑ NaCl delivery (proxy for ↑ GFR).
- Release of vasoactive substances (e.g., adenosine, ATP).
- Causes afferent arteriole constriction, reducing GFR.
⭐ NSAIDs inhibit prostaglandins (which dilate afferent arterioles), leading to vasoconstriction. This can precipitate acute renal failure by impairing the kidney's ability to maintain RBF.
Myogenic Mechanism - The Stretch Reflex
- An intrinsic property of vascular smooth muscle; it provides a rapid, localized response to changes in arterial pressure, independent of nerves or hormones.
- Primary Goal: To maintain a constant renal blood flow (RBF) and glomerular filtration rate (GFR) despite fluctuations in systemic blood pressure.
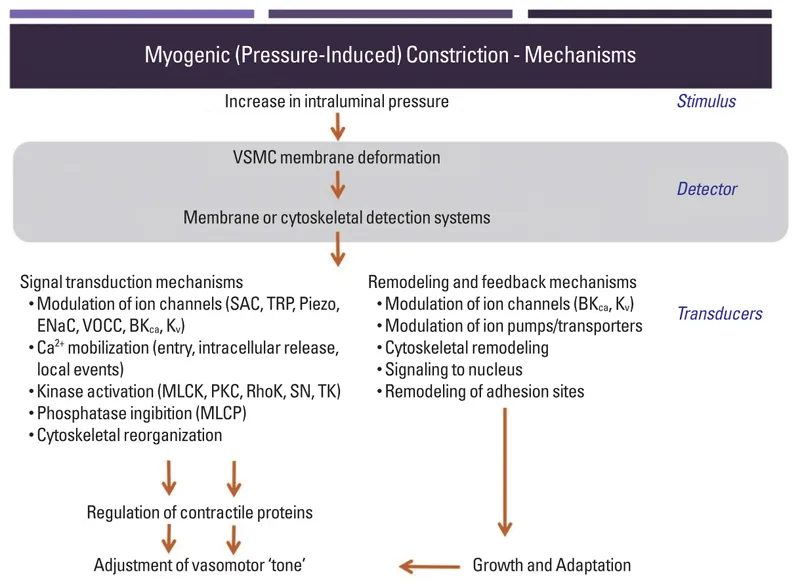
⭐ This mechanism is the first line of defense against hypertensive damage to the glomeruli, reacting within seconds to pressure changes. It is most effective within a mean arterial pressure range of 80-180 mmHg.
Tubuloglomerular Feedback - Macula Densa's Message
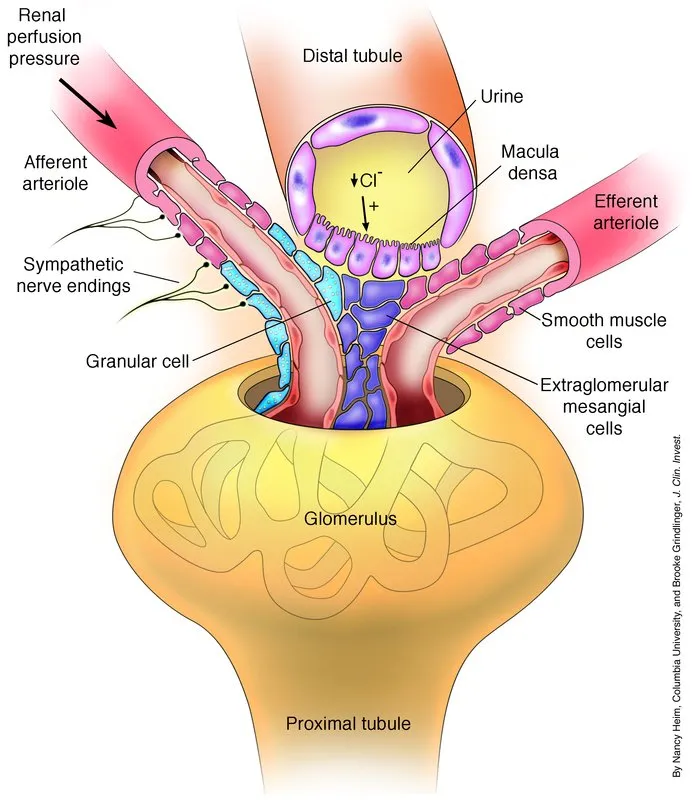
- A key intrinsic mechanism for renal autoregulation, centered on the Juxtaglomerular Apparatus (JGA).
- Sensor: Macula Densa cells in the Distal Convoluted Tubule (DCT) detect changes in tubular fluid flow and NaCl concentration.
Mechanism:
- Trigger: ↑ GFR → ↑ fluid & NaCl delivery to the macula densa.
- Response: Macula densa cells release vasoactive substances (ATP, adenosine).
- Action: These paracrine signals cause vasoconstriction of the afferent arteriole.
- Result: ↓ renal blood flow → ↓ GFR, returning it to normal.
⭐ The macula densa acts as a "smart sensor," linking distal tubule flow directly to glomerular hemodynamics. This feedback is crucial for protecting the glomerulus from pressure-induced damage.
Extrinsic Control - When Hormones Hijack
- Sympathetic Nervous System (Norepinephrine):
- Activated by major stress (e.g., hemorrhage, fight-or-flight).
- Constricts both afferent & efferent arterioles → ↓↓ RBF & ↓ GFR.
- Renin-Angiotensin II System (AT-II):
- Low levels: Preferentially constricts efferent arteriole → ↑ GFR to preserve filtration.
- High levels (e.g., severe volume depletion): Constricts both afferent & efferent arterioles → ↓ RBF & ↓ GFR.
⭐ Prostaglandins vasodilate the afferent arteriole. NSAIDs block prostaglandin synthesis, causing afferent constriction and ↓ GFR, risking acute kidney injury in vulnerable patients.
High‑Yield Points - ⚡ Biggest Takeaways
- Myogenic mechanism: Afferent arteriole intrinsically constricts when stretched by high systemic pressure.
- Tubuloglomerular feedback (TGF): Macula densa senses ↑ NaCl delivery, releasing adenosine to constrict the afferent arteriole.
- Autoregulation maintains a stable GFR and RBF over a mean arterial pressure range of 80-180 mmHg.
- Angiotensin II preferentially constricts the efferent arteriole, helping to preserve GFR during hypoperfusion.
- Prostaglandins dilate the afferent arteriole; NSAIDs block this, causing constriction and ↓ GFR.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

