Central Command & Initial Response - The 'Go' Signal
- Origin: A feed-forward signal from the motor cortex and higher brain centers, initiated by the anticipation or start of exercise.
- Mechanism: Directly stimulates medullary cardiovascular centers before receiving feedback from peripheral chemoreceptors or mechanoreceptors in the muscle.
- Immediate Effects:
- Rapid withdrawal of parasympathetic (vagal) tone.
- Increased sympathetic outflow to the heart and vasculature.
- Result: An anticipatory rise in heart rate (HR) and cardiac output (CO).
⭐ The initial, rapid increase in heart rate at the onset of exercise is primarily due to vagal withdrawal, not sympathetic activation.
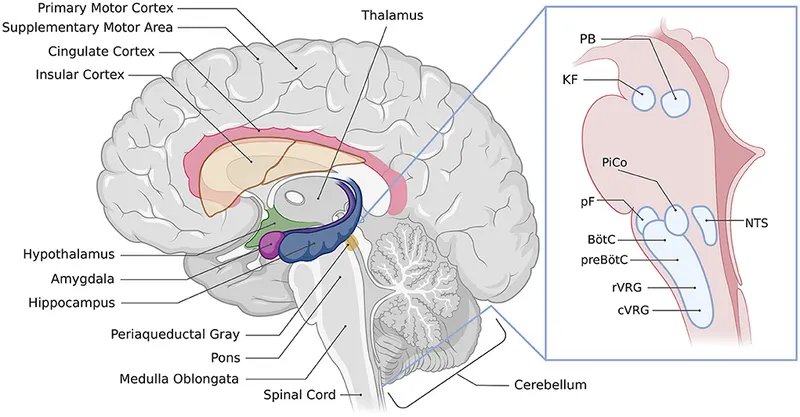
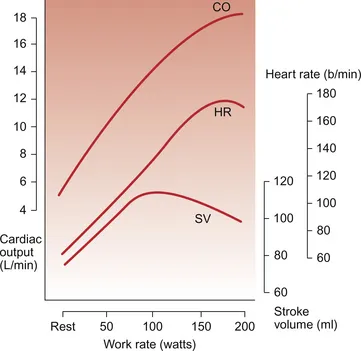
Cardiac Output - The Heart's Hustle
-
Definition: The volume of blood pumped by the heart per minute, crucial for oxygen delivery.
-
Formula: $CO = HR \times SV$
-
Response to Exercise: CO increases linearly with workload to meet the muscles' metabolic demands.
- Resting: ~5 L/min
- Maximal Exercise: Can reach 20-40 L/min.
-
Heart Rate (HR):
- Rises via initial parasympathetic withdrawal, then increased sympathetic drive.
-
Stroke Volume (SV):
- Increases from ↑ preload (Frank-Starling) and ↑ contractility.
- Aided by ↓ afterload (peripheral vasodilation).
- Typically plateaus at 40-60% of VO₂ max in untrained individuals.
⭐ In elite athletes, stroke volume often doesn't plateau but continues to rise to maximum exercise capacity, allowing for a much higher cardiac output.
Blood Pressure & SVR - The Squeeze Play
- Systolic BP (SBP): ↑ Linearly with workload. Driven by ↑ cardiac output.
- Diastolic BP (DBP): Stays same or ↓ slightly. Due to vasodilation in active muscle, which ↓ SVR.
- Pulse Pressure: ↑ Widens significantly (SBP ↑, DBP constant).
- Mean Arterial Pressure (MAP): ↑ Modestly. Calculated as $MAP \approx DP + 1/3(SP - DP)$.
- Systemic Vascular Resistance (SVR/TPR): ↓↓ Markedly. Vasodilation outweighs sympathetic vasoconstriction in non-active tissues.
⭐ During dynamic exercise, a failure of SBP to increase (>10 mmHg drop) may indicate severe LV dysfunction or aortic stenosis.
Blood Flow Redistribution - The Great Diversion
- During exercise, blood is shunted from inactive tissues to meet the high metabolic demands of active muscle.
- Flow ↑ to:
- Active skeletal muscle (up to 85% of cardiac output)
- Heart (coronary arteries)
- Skin (thermoregulation)
- Flow ↓ from:
- Splanchnic circulation (GI tract, liver, spleen)
- Kidneys
- Brain blood flow is maintained.
- Mechanism: Sympathetic α1-mediated vasoconstriction in non-essential beds, overridden by local vasodilator metabolites (adenosine, K⁺, CO₂) in active muscle-a phenomenon called functional sympatholysis.
⭐ Coronary blood flow increases 4-5x primarily due to local metabolic hyperemia (adenosine release from myocyte activity), not direct sympathetic vasodilation.
High‑Yield Points - ⚡ Biggest Takeaways
- Cardiac output increases linearly with workload, driven primarily by ↑ heart rate; stroke volume plateaus at higher intensities.
- Systolic BP ↑ due to increased cardiac output, while diastolic BP remains stable or slightly ↓ due to decreased peripheral resistance.
- Total peripheral resistance (TPR) ↓ significantly due to profound vasodilation in active skeletal muscle.
- The arteriovenous O₂ difference widens markedly as muscles extract more oxygen.
- Blood flow is shunted from splanchnic circulation to exercising muscles.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

