Glucagon Basics - The Glucose Guardian
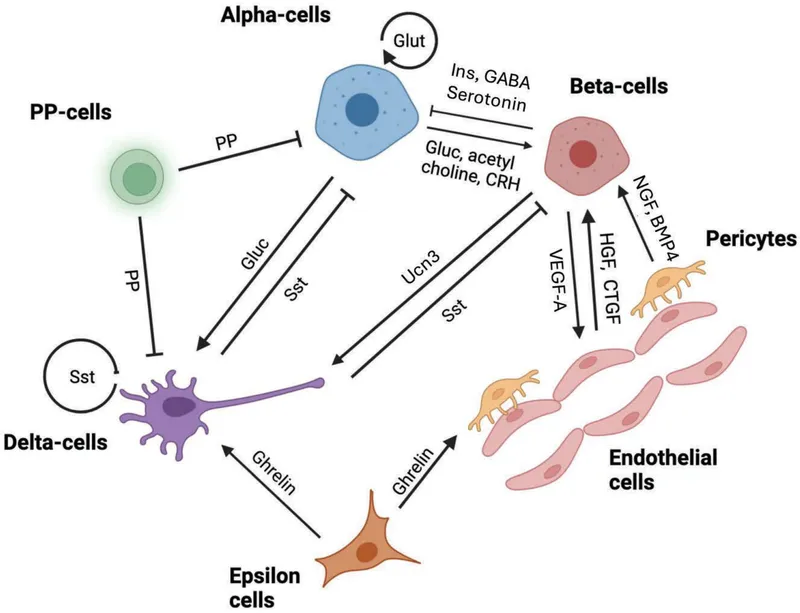
- Source: α-cells of pancreatic islets of Langerhans.
- Action: ↑ blood glucose. The primary counter-regulatory hormone to insulin.
- Mechanism: Binds to G-protein coupled receptors (GPCRs) on hepatocytes → activates adenylyl cyclase → ↑ cAMP → PKA activation.
- Primary Target: Liver.
⭐ Glucagon, not epinephrine, is the most important glucose counter-regulatory hormone in protecting against hypoglycemia.
Regulation of Secretion - The 'Hangry' Hormone
- Primary Stimulus: ↓ Blood glucose (triggers release when < 70 mg/dL).
- Other Stimulators:
- ↑ Amino acids (esp. arginine, alanine) → prevents hypoglycemia after a pure protein meal.
- Sympathetic stimulation (β₂-receptors).
- Vagal (cholinergic) stimulation.
- Stress (e.g., cortisol).
- Inhibitors:
- ↑ Blood glucose.
- Insulin (paracrine effect).
- Somatostatin (paracrine effect).
- GLP-1.
⭐ After a protein-rich meal, both insulin and glucagon rise. Amino acids stimulate glucagon to offset insulin's hypoglycemic effect, maintaining normal blood sugar.
Mechanism of Action - The Liver's Taskmaster
- Receptor: Binds to G-protein coupled receptors (GPCRs) on hepatocytes.
- Pathway: Utilizes a Gs-alpha subunit to activate adenylyl cyclase.
- Second Messenger: ↑ intracellular cyclic AMP ($cAMP$) from ATP.
- Kinase Activation: $cAMP$ activates Protein Kinase A (PKA).
⭐ Exam Favorite: Muscle cells lack glucagon receptors; therefore, glucagon does not cause glycogenolysis in skeletal muscle. Its primary effect is hepatic.
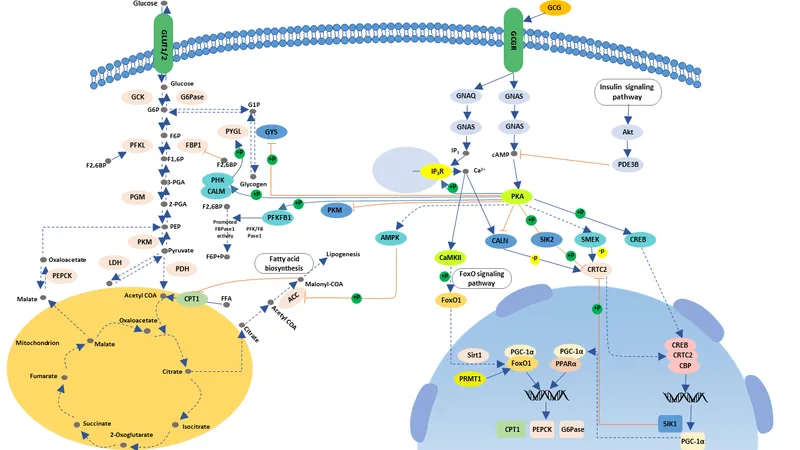
Metabolic Effects - Flipping the Switch
Glucagon's primary role is to mobilize energy stores, acting as a counter-regulatory hormone to insulin. It primarily targets the liver to raise blood glucose.
- Liver (Main Target Organ):
- ↑ Glycogenolysis: Rapid breakdown of stored glycogen.
- ↑ Gluconeogenesis: Synthesis of new glucose from amino acids, lactate, and glycerol.
- ↑ Ketogenesis: Promotes fatty acid oxidation to produce ketone bodies.
- Adipose Tissue:
- ↑ Lipolysis: Breaks down triglycerides, releasing Free Fatty Acids (FFAs) and glycerol.
⭐ Glucagon is used to treat severe hypoglycemia in diabetic patients and can also be an antidote for beta-blocker overdose due to its ability to increase cAMP in the myocardium, leading to increased heart rate and contractility.
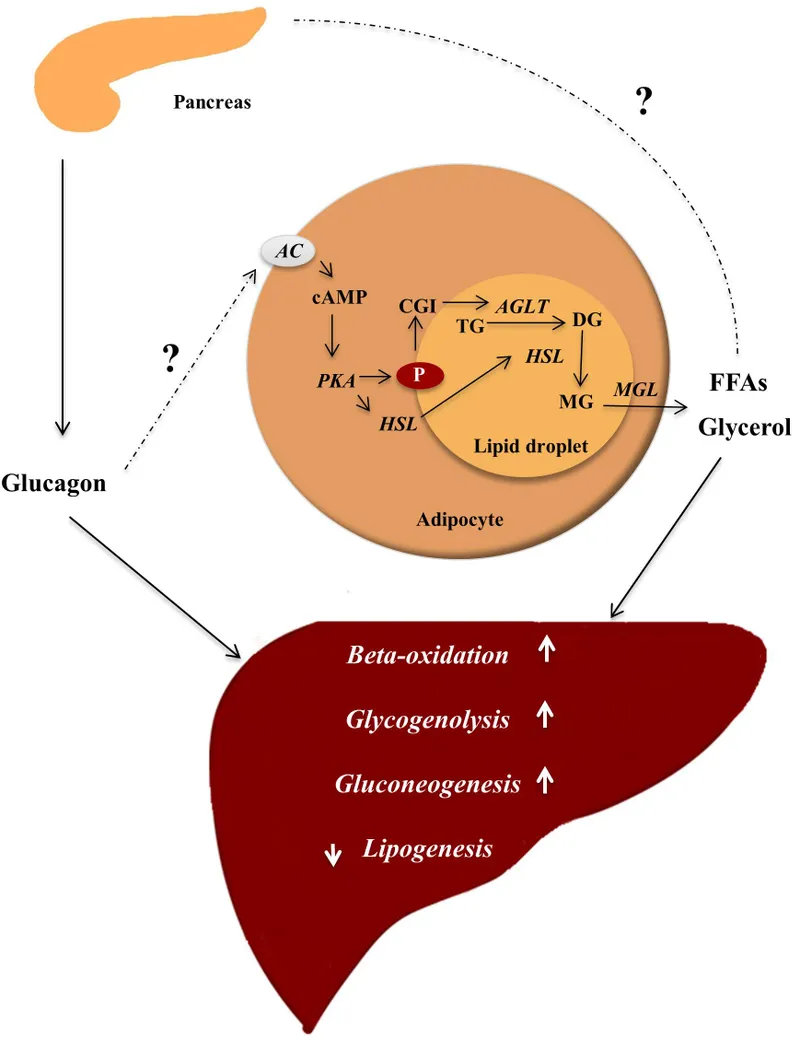
Clinical Correlates - When Glucagon Goes Rogue
- Glucagonoma: Rare pancreatic α-cell tumor → ↑↑ glucagon.
- 📌 Mnemonic (The 5 D's):
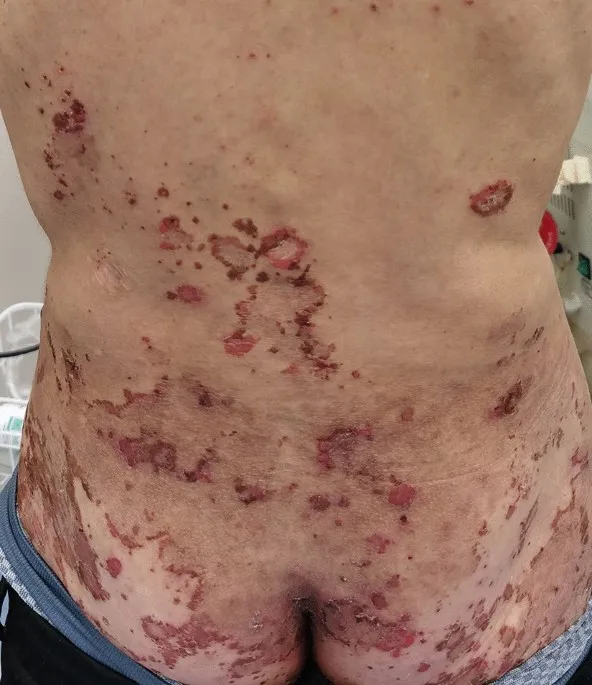
- Dermatitis (Necrolytic Migratory Erythema)
- Diabetes (new, mild)
- DVT (Deep Vein Thrombosis)
- Declining weight
- Depression
- Diagnosis: Markedly ↑ glucagon > 500 pg/mL.
⭐ Necrolytic migratory erythema (NME) is the presenting sign in 70% of glucagonoma cases.
High‑Yield Points - ⚡ Biggest Takeaways
- Glucagon, from pancreatic α-cells, is the key catabolic hormone of the fasting state.
- Its primary goal is to ↑ blood glucose by stimulating hepatic glycogenolysis and gluconeogenesis.
- It acts via a Gs-coupled GPCR, leading to an increase in intracellular cAMP.
- Secretion is stimulated by hypoglycemia and amino acids (e.g., after a protein-rich meal).
- Secretion is inhibited by hyperglycemia, insulin, and somatostatin.
- Glucagonoma classically presents with diabetes, necrolytic migratory erythema, and DVT.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

