PR Interval - The Basics
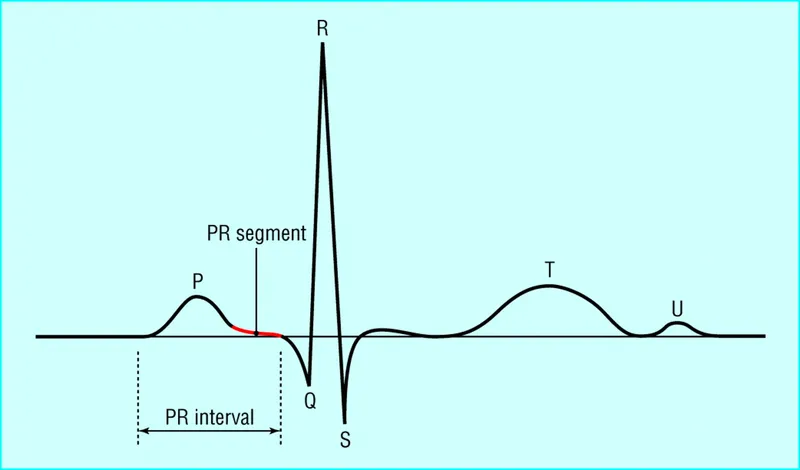
- Represents the time from the start of atrial depolarization to the start of ventricular depolarization.
- Components: P wave + PR segment.
- Normal duration: $0.12 - 0.20$ seconds (3-5 small squares on ECG paper).
- Clinically, it reflects the conduction time through the AV node.
⭐ A consistently short PR interval (<0.12s) may suggest a pre-excitation syndrome, like Wolff-Parkinson-White (WPW), due to an accessory pathway bypassing the AV node.
Short PR Interval - Speedy Conduction
A PR interval < 0.12s indicates accelerated atrioventricular conduction, often by bypassing the AV node's physiological delay. This suggests ventricular pre-excitation.
- Key Causes:
- Wolff-Parkinson-White (WPW) Syndrome: An accessory pathway (Bundle of Kent) directly connects the atria to the ventricles. Look for the classic triad: short PR, a wide QRS, and a slurred upstroke on the QRS complex (Delta Wave).
- Lown-Ganong-Levine (LGL) Syndrome: An accessory pathway (James fibers) bypasses the AV node and connects to the His bundle. Results in a short PR but a normal QRS complex.
- Junctional Rhythm: The electrical impulse originates from the AV junction, leading to a shorter conduction time to the ventricles.
📌 Mnemonic: Wolves Pounce Low (WPW, P-Junctional, LGL).
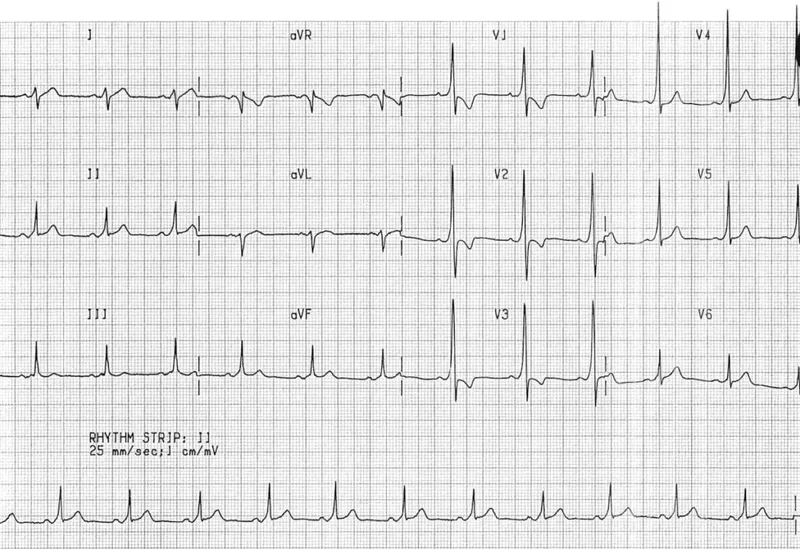
⭐ Exam Favorite: In a patient with WPW who develops atrial fibrillation, AV nodal blocking agents (adenosine, β-blockers, CCBs) are contraindicated. They can accelerate conduction through the accessory pathway, potentially precipitating ventricular fibrillation.
Long PR Interval - Conduction Delays
A PR interval exceeding 0.20 seconds (one large box on ECG) signifies a delay in the electrical impulse traveling from the atria to the ventricles. This is the defining feature of atrioventricular (AV) blocks.

-
First-Degree AV Block:
- Characterized by a constant, prolonged PR interval > 0.20s.
- A 1:1 relationship between P waves and QRS complexes is maintained.
- Usually benign.
-
Second-Degree AV Block: Involves intermittently dropped QRS complexes.
- Mobitz I (Wenckebach): Progressive PR interval lengthening across several beats, culminating in a non-conducted P wave (a "dropped" beat).
- 📌 Mnemonic: "Longer, longer, longer, DROP! Now you have a Wenckebach."
- Mobitz II: The PR interval remains constant for all conducted beats, but some P waves are unexpectedly not followed by a QRS.
- Mobitz I (Wenckebach): Progressive PR interval lengthening across several beats, culminating in a non-conducted P wave (a "dropped" beat).
⭐ Mobitz II is considered more clinically significant than Mobitz I because it carries a higher risk of progressing to a complete heart block. It often points to structural damage below the AV node.
- The PR interval reflects AV conduction time; normal duration is 0.12-0.20 seconds.
- A short PR interval (<0.12s) suggests pre-excitation (e.g., Wolff-Parkinson-White syndrome).
- A prolonged PR interval (>0.20s) indicates an AV conduction block.
- First-degree AV block: Consistently prolonged PR interval without dropped beats.
- Second-degree AV block: Intermittent non-conduction of P waves (dropped QRS complexes).
- Third-degree AV block: Complete AV dissociation; P waves and QRS complexes are independent.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

