Structural Changes - Old Heart, New Shape
-
Myocardium & Chambers:
- ↓ Myocyte & pacemaker cell count.
- ↑ Myocyte size → Left Ventricular Hypertrophy (LVH), often concentric.
- ↑ Interstitial collagen & fibrosis → ↑ myocardial stiffness, impaired relaxation.
- "Sigmoid septum": Basal septum hypertrophies, bulging into LV outflow tract.
- ↑ Left atrial size.
-
Vasculature (Arteriosclerosis):
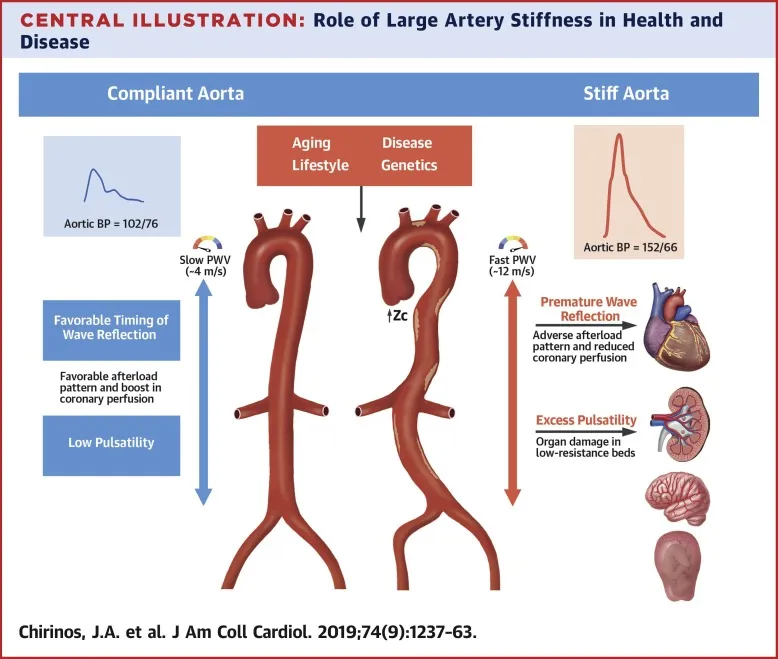
- Large arteries stiffen: ↓ elastin, ↑ collagen & calcification.
- Leads to ↑ systolic BP & pulse pressure.
-
Valves:
- ↑ Fibrosis & calcification (esp. aortic & mitral).
⭐ The classic aging heart develops a "sigmoid septum" shape, where the base of the interventricular septum thickens and bulges into the LV outflow tract. This can cause a dynamic obstruction, mimicking hypertrophic cardiomyopathy.
Functional Consequences - The Pressure's On
-
Arterial Stiffening & Pressure Changes:
- ↓ Arterial compliance (elastin fragmentation) → ↑ afterload.
- Results in ↑ systolic blood pressure (SBP) & ↓ diastolic blood pressure (DBP).
- Leads to a widened pulse pressure ($SBP - DBP$).
-
Cardiac Adaptations & Limitations:
- Concentric left ventricular hypertrophy (LVH) develops to overcome ↑ afterload.
- Leads to diastolic dysfunction (impaired ventricular relaxation).
- ↓ Stroke volume & cardiac output, especially during exercise.
- ↓ Maximal heart rate & β-adrenergic responsiveness.
⭐ Isolated systolic hypertension (ISH), defined as SBP ≥140 mmHg with DBP <90 mmHg, is the most common form of hypertension in older adults.
Autonomic & Hormonal Shifts - Control System Drift
- Baroreflex Sensitivity: ↓ Decreased responsiveness to blood pressure changes.
- Leads to impaired heart rate response to hypotension or hypertension.
- Major contributor to orthostatic hypotension in the elderly.
- Sympathetic Tone: ↑ Increased baseline plasma norepinephrine (NE).
- Due to ↑ NE spillover & ↓ clearance.
- Paradoxically, β-adrenergic receptor responsiveness is ↓ (desensitization), blunting stress responses.
- Hormonal Regulation:
- ↓ Plasma renin & aldosterone levels → blunted response to volume depletion.
- ↑ Atrial Natriuretic Peptide (ANP) levels.
⭐ Decreased baroreceptor sensitivity is a key factor in the high incidence of orthostatic hypotension, increasing the risk of falls and syncope in geriatric patients.
Clinical Implications - The Geriatric Syndromes
- Syncope & Falls: Common due to ↑ cardiovascular vulnerability.
- Orthostatic Hypotension: Result of ↓ baroreceptor sensitivity & autonomic dysfunction. Leads to dizziness and falls upon standing.
- Arrhythmias: Sick sinus syndrome or AV block can cause transient cerebral hypoperfusion.
- Aortic Stenosis: Fixed cardiac output may precipitate exertional syncope.
- Frailty: A state of ↑ vulnerability to stressors, often exacerbated by underlying cardiovascular diseases like heart failure or CAD. Associated with poor post-procedural outcomes.
- Cognitive Impairment: Chronic hypoperfusion from atherosclerosis or low cardiac output contributes to vascular dementia, complicating medication management.
⭐ Orthostatic Hypotension: Defined as a drop in systolic BP of ≥20 mmHg or diastolic BP of ≥10 mmHg within 3 minutes of standing.
High‑Yield Points - ⚡ Biggest Takeaways
- Arterial stiffening (arteriosclerosis) leads to ↑ systolic BP and widened pulse pressure.
- Concentric left ventricular hypertrophy develops due to chronic ↑ afterload.
- Diastolic dysfunction results from impaired myocardial relaxation and ↑ LV stiffness.
- ↓ Maximal heart rate and ↓ cardiac output with exercise due to ↓ adrenergic responsiveness.
- ↓ Baroreceptor sensitivity increases the risk of orthostatic hypotension.
- Fibrosis of the conduction system can lead to arrhythmias and AV block.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

