Pathophysiology - The CO₂ Traffic Jam
- Foundation: Henderson-Hasselbalch Equation: $pH = pKa + log([HCO₃⁻] / [0.03 * PCO₂])$
- Definition: A primary acid-base disorder characterized by:
- ↓ pH < 7.35
- ↑ PaCO₂ > 45 mmHg
- Primary Disturbance: Alveolar hypoventilation is the root cause, impairing CO₂ elimination from the lungs. This leads to CO₂ accumulation in the blood (hypercapnia).
- Mechanism: As PaCO₂ rises, the equilibrium of the bicarbonate buffer system shifts right, increasing H⁺ concentration and decreasing pH.
- $CO₂ + H₂O ↔ H₂CO₃ ↔ H⁺ + HCO₃⁻$
⭐ In acute respiratory acidosis, plasma [HCO₃⁻] increases by ~1 mEq/L for every 10 mmHg increase in PaCO₂ above 40 mmHg.
Etiologies - Why the Lungs Loaf
⭐ In opioid overdose, the earliest and most specific sign of respiratory compromise is a decreased respiratory rate (bradypnea), a direct effect on the brainstem's respiratory centers.
The fundamental issue is alveolar hypoventilation, leading to inadequate $CO_2$ clearance. Causes can be remembered with the mnemonic 📌 DEPRESS:
| Category | Causes (Hypoventilation → ↑Pa$CO_2$) |
|---|---|
| Drugs / CNS Depression | * Opioids, Sedatives, Anesthetics: Suppress respiratory drive. - Brainstem Injury: Stroke, trauma, infection. - Central Sleep Apnea. |
| Edema / Airway Obstruction | * COPD/Asthma Exacerbation: Air trapping & obstruction. - Laryngospasm, Foreign Body. - Pulmonary Edema (late stage). |
| Pneumonia / Pulmonary | * Severe Pneumonia/ARDS: V/Q mismatch & ↑ dead space. - Interstitial Lung Disease. |
| Respiratory Muscle Weakness | * Neuromuscular: Myasthenia Gravis, Guillain-Barré, ALS. - Toxins: Botulism. - Muscular Dystrophy. |
| Emboli / Chest Wall | * Chest Wall Restriction: Kyphoscoliosis, flail chest, obesity. - Massive Pulmonary Embolism (can cause late respiratory failure). |
| Spinal Cord / Secretions | * High Spinal Cord Injury (above C3-C5). - Obesity Hypoventilation Syndrome (Pickwickian). |
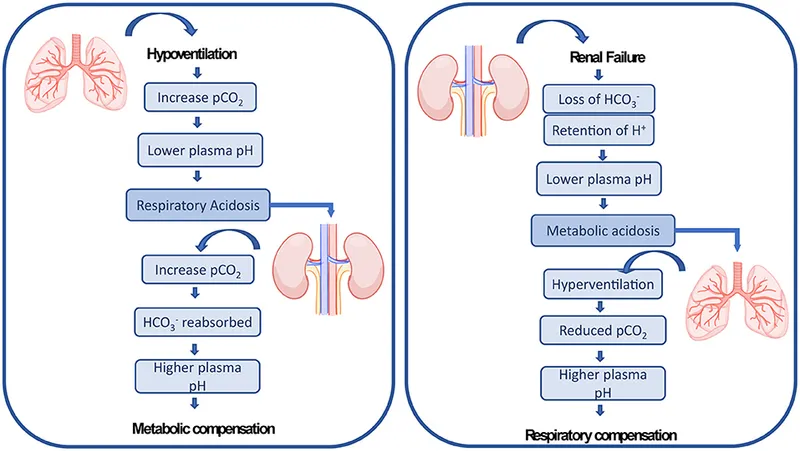
Compensation - The Kidney Cleanup Crew
The body employs two main strategies to counteract respiratory acidosis:
-
Acute (Cellular Buffering): An immediate, but limited, first line of defense.
- Intracellular proteins and hemoglobin bind $H⁺$.
- Formula: For every 10 mmHg ↑ in PCO₂, $HCO₃⁻$ ↑ by 1 mEq/L.
-
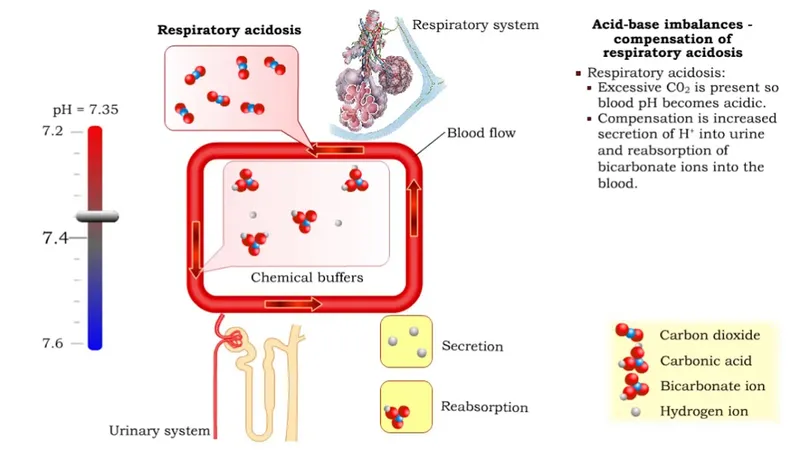
Chronic (Renal Compensation): A slower, more powerful response taking 3-5 days.
- The kidneys enhance the excretion of acid ($H⁺$, primarily as $NH₄⁺$) and increase the reabsorption of base ($HCO₃⁻$).
- Formula: For every 10 mmHg ↑ in PCO₂, $HCO₃⁻$ ↑ by 3-4 mEq/L.
⭐ In chronic respiratory acidosis, the resulting increase in serum bicarbonate is a direct compensatory action by the kidneys, not a separate metabolic alkalosis. Evaluating the anion gap can help differentiate complex disorders.
Diagnosis - Cracking the ABG Code
- Clinical Features: Headache, anxiety, blurred vision, & restlessness, which can progress to confusion, somnolence, asterixis, and coma.
- Arterial Blood Gas (ABG): Key findings are a ↓ pH (< 7.35), ↑ PaCO₂ (> 45 mmHg), and a compensatory ↑ HCO₃⁻.
- Compensation Check: Calculate the expected HCO₃⁻ to determine if a mixed disorder is present.
⭐ In chronic respiratory acidosis, for every 10 mmHg increase in PaCO₂, the HCO₃⁻ is expected to increase by 3.5-4 mEq/L. A value outside this range points to a mixed disorder.
High-Yield Points - ⚡ Biggest Takeaways
- Respiratory acidosis is driven by hypoventilation, leading to CO₂ retention (↑ PaCO₂) and subsequent acidemia (↓ pH).
- Key causes include CNS depression (e.g., opioids), airway obstruction (COPD), and neuromuscular disease (e.g., Guillain-Barré).
- Acute compensation is minimal; for every 10 mmHg ↑ in PaCO₂, HCO₃⁻ rises by ~1 mEq/L.
- Chronic compensation is renal; kidneys increase HCO₃⁻ reabsorption, raising it by ~4 mEq/L per 10 mmHg ↑ in PaCO₂.
- Always look for a primary ↑ in PaCO₂ as the initiating event.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

